Translate this page into:
First Report of Preoperative Imaging Diagnosis of a Surgically Confirmed Case of Valentino's Syndrome
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Perforation of a duodenal ulcer (DU) into the retroperitoneal space presenting with clinical features of acute appendicitis is known as Valentino's syndrome. Post duodenal perforation, the gastric and duodenal fluids tend to settle in the right paracolic gutter causing peritonitis and clinically mimicking acute appendicitis. Only three cases of Valentino's syndrome have been reported till date in the published literature and there is only one previous report of its preoperative imaging diagnosis. To our knowledge, this is the first reported case of preoperative imaging diagnosis in a surgically confirmed case of Valentino's syndrome. In most cases, patients with undiagnosed Valentino's syndrome are operated for acute appendicitis, and on finding a normal appendix, search is made for the cause of peritonitis, which then leads to retroperitoneal perforation of duodenum. The diagnosis of Valentino's syndrome by computed tomography (CT) imaging is easy and can help in avoiding the surgery or directing the surgeon directly to the repair of the duodenal perforation. It is, therefore, essential for emergency physicians, surgeons, and radiologists to know about this entity and consider it in the differential diagnosis.
Keywords
Acute appendicitis
duodenal ulcer perforation
laparoscopy
pneumoretroperitoneum
Valentino's syndrome
INTRODUCTION

Peptic ulcer is a defect in the mucosal lining of the stomach or duodenum. Perforation of the stomach or duodenum is one of the serious complications of peptic ulcer that requires emergency medical care.[1] Valentino's syndrome is the retroperitoneal perforation of a duodenal ulcer (DU) causing right lower quadrant (RLQ) abdominal pain and thus mimics acute appendicitis.[23] Rudolph Valentino was a very popular actor in the United States of America during the silent film era, after whom the syndrome is named. He was hospitalized after collapsing in a New York hotel and was initially diagnosed with acute appendicitis and gastric ulcers. He was operated and found to have retroperitoneal perforation of duodenum. He later died due to post-surgical complications. The RLQ pain in Valentino's syndrome is caused by gastric and duodenal fluids that tend to settle in the right paracolic gutter inciting peritoneal inflammation.[23] Only three cases of Valentino's syndrome have been reported till date in the published literature and there is only one previous report of its preoperative imaging diagnosis.[234] In most cases, patients with undiagnosed Valentino's syndrome are operated for acute appendicitis, and on finding a normal appendix, search is made for the cause of peritonitis, which then leads to retroperitoneal perforation of duodenum.
CASE REPORT
A 21-year-old gentleman presented to the emergency department with complaints of severe right lower abdominal pain, epigastric pain, vomiting, and fever of 8 h duration. On examination, he was febrile and had rebound tenderness in the right iliac fossa. Blood examination revealed leukocytosis with white blood cell count being 23,000 per microliter (normal 4000-10,000). 7-days earlier he had undergone a minor surgery for his right toe and was treated with nonsteroidal anti-inflammatory drugs (NSAIDs) for a week to relieve pain. Clinically, acute appendicitis was suspected and the patient was referred for computed tomography (CT) scan of abdomen and pelvis and a chest radiograph. CT scan of abdomen and pelvis without and with intravenous (IV) contrast [Figures 1 and 2] revealed air in the retroperitoneum (pneumoretroperitoneum), predominantly around the right kidney. Right kidney revealed normal parenchymal enhancement without any focal lesions. Air and significant fat stranding were noted in the region of the duodenum tracking along the subhepatic region up to the right perinephric region. Minimal fluid collection was noted in the right paracolic gutter with adjacent fat stranding. Minimal free fluid and free air were also noted in the peritoneal cavity. Appendix was normal in caliber with no CT evidence of acute appendicitis. There was no evidence of colonic diverticulosis or acute diverticulitis. The chest radiograph revealed air around the visualized part of the right kidney [Figure 3]. The diagnosis of retroperitoneal duodenal perforation causing pneumoretroperitoneum was made. The imaging diagnosis and the clinical features were suggestive of Valentino's syndrome. The patient was operated upon within 1 h.
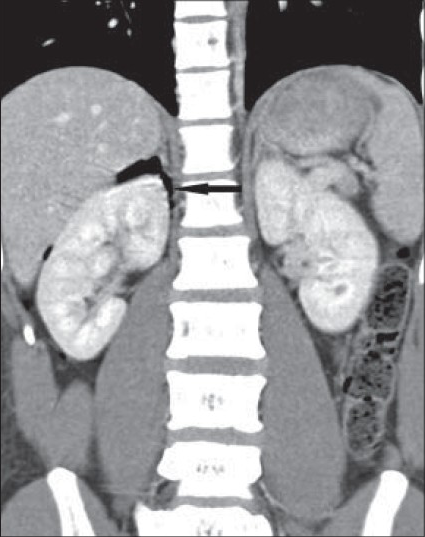
- 21-year-old man with an 8-h history of severe right lower abdominal pain, epigastric pain, vomiting, and fever, diagnosed with Valentino's syndrome. Post contrast computed tomography (CT) scan of abdomen, coronal reformatted image shows air in the retroperitoneum on the right, predominantly around the right kidney (arrow). Normal right renal parenchyma is noted.
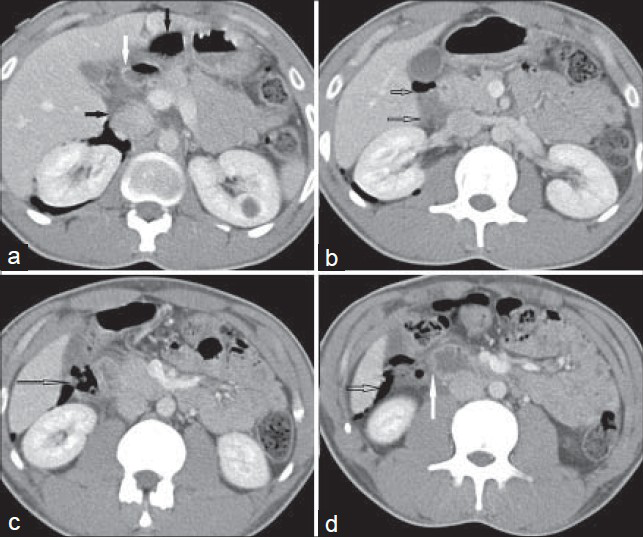
- 21-year-old man with an 8-h history of severe right lower abdominal pain, epigastric pain, vomiting, and fever diagnosed with Valentino's syndrome. (a-d) Serial post contrast axial computed tomography (CT) scans of abdomen (a) Above the level of renal hila demonstrating the first part of duodenum; (b) At the level of renal hila demonstrating the second part of duodenum; (c) Just below the level of renal hila; and d): At left infrarenal level show significant fat stranding and air in and around the region of the duodenum (solid black arrow), duodenal wall thickening (white arrow), significant fat stranding, retroperitoneal fluid collection, and air in the subhepatic region (hollow black arrow).
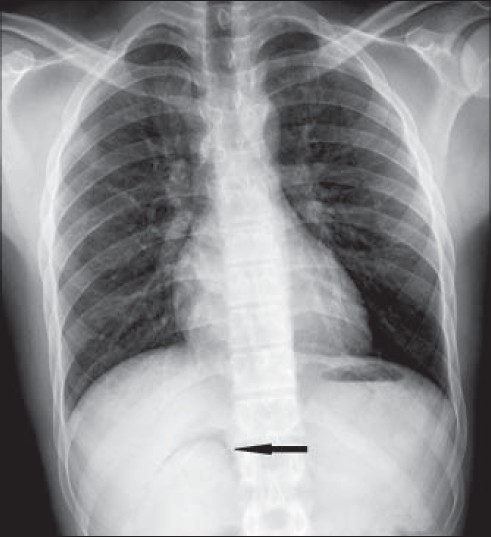
- 21-year-old man with an 8-h history of severe right lower abdominal pain, epigastric pain, vomiting, and fever diagnosed with Valentino's syndrome. Chest radiograph (frontal view) shows right perinephric air (arrow).
Diagnostic laparoscopy revealed minimal amount of turbid fluid in the subhepatic region related to the first part of the duodenum which was covered anteriorly by peritoneum. Upon retraction of the liver and gall bladder, a small peritoneal rent was seen with bilious fluid leaking through the rent. Extension of the peritoneal rent laterally exposed the first part of the duodenum with the perforation in its anterior wall. The retroperitoneal space in relation to the second part of the duodenum and the right kidney showed moderate inflammatory reaction evidenced by edema of the posterior peritoneum in that area [Figure 4 and Video 1].
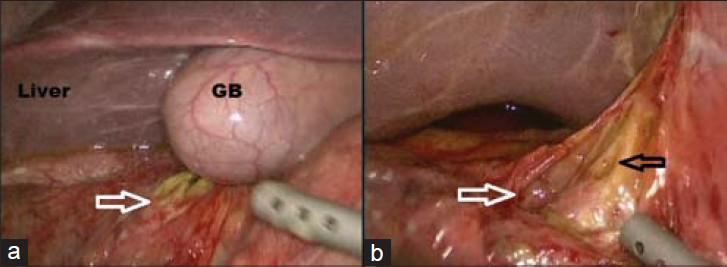
- 21-year-old man with an 8-h history of severe right lower abdominal pain, epigastric pain, vomiting, and fever diagnosed with Valentino's syndrome. Intraoperative photographs show (a) retroperitoneal duodenum and the peritoneal rent (white arrow) and (b) shows the perforation in the anterior wall of the duodenum (black arrow). (GB: Gall bladder).
The procedure was completed laparoscopically. The opened retroperitoneal space was irrigated using normal saline. The perforation was closed using two Vicryl 2/0 sutures reinforced by omentum. The rest of the peritoneal cavity was irrigated using warm normal saline. A J-Vac (Ethicon) drain was placed in the subhepatic region and the abdomen was closed in layers [Figure 4 and Video 1].
The postoperative period was smooth and uneventful. The patient was kept on IV fluids, IV antibiotics, and IV Ranitidine. Nasogastric tube was removed on the first postoperative day. Oral intake was resumed on the second postoperative day and was increased gradually from oral fluids to full diet. The patient was discharged on the sixth postoperative day after removal of the J-Vac drain.
The patient was in good general condition and free of any symptoms during the regular follow-up examination 3-months after surgery.
DISCUSSION
Major part of the duodenum is retroperitoneal except for the duodenal bulb (first or superior part) and a very small distal part near the ligament of Treitz.[5] In our case, even the first part of duodenum was retroperitoneal, which is a rare finding. Perforation of the duodenum can be intraperitoneal or retroperitoneal.[5] In both cases, it is considered a surgical emergency.[15] Intraperitoneal perforation of the duodenum usually causes pneumoperitoneum.[5] Retroperitoneal perforation of the duodenum is rare and may cause pneumoretroperitoneum.[5] In our case, there was retroperitoneal perforation of the first part of duodenum and an adjacent small peritoneal rent as well. The small peritoneal rent was the cause of minimal fluid and free air within the peritoneal cavity. Retroperitoneal duodenal rent was larger and was the cause of the predominantly retroperitoneal inflammatory reaction and the pneumoretroperitoneum.
A peptic ulcer is necrosis of the mucosa of the stomach or duodenum causing a distinct breach in the mucosa due to caustic effects of gastric secretions in the lumen.[1] Helicobacter pylori is one of the most common causes of peptic ulcer.[1] Ulcers can also be caused or worsened by drugs such as aspirin, ibuprofen, and other NSAIDs.[1] Four times as many peptic ulcers arise in the duodenum as in the stomach itself. Duodenal ulcers are generally benign.[1]
CT is the imaging modality of choice for the diagnosis of Valentino's syndrome. It should always be suspected when signs and symptoms of acute appendicitis are accompanied by epigastric pain, and history of acid peptic disease and/or recent consumption of NSAIDs. Characteristic features on CT imaging include air in the retroperitoneum on the right side, predominantly around the right kidney, fat stranding and retroperitoneal air in and around the region of the duodenum, and duodenal wall thickening. Right perinephric air can also be visualized on an abdominal radiograph or a chest radiograph (as in our case). Air around the right kidney leads to masking of the right kidney from artifacts on ultrasound examination, known as veiled right kidney sign.[3] Commonest cause of retroperitoneal air around right kidney is emphysematous pyelonephritis. Presence of normal enhancing renal parenchyma without any focal lesions on CT scan excluded this possibility in our case.
Urgent surgical intervention to repair the duodenal perforation is the preferred treatment for Valentino's syndrome. There was one report of successful management of Valentino's syndrome with only conservative treatment.[3] Some consider initial conservative management and surgical intervention only if the patient's condition deteriorates.[23] In our case, the patient was managed with urgent surgical intervention and discharged on the sixth postoperative day. Follow-up in out-patient department done 3-months after surgery showed the patient was in good general condition and free of any symptoms.
CONCLUSION
In conclusion, we present a very rare case of preoperative diagnosis and successful surgical management of Valentino's syndrome. To our knowledge, this is the first reported case of preoperative imaging diagnosis in a surgically confirmed case of Valentino's syndrome. The diagnosis of Valentino's syndrome by CT imaging is easy and can help in avoiding the surgery or directing the surgeon directly to the repair of the duodenal perforation. It is, therefore, essential for emergency physicians, surgeons, and radiologists to know about this entity and consider it in the differential diagnosis. Our aim is to increase the awareness of this condition, as a high degree of suspicion is essential in its preoperative diagnosis and the preoperative diagnosis may reduce patient morbidity and mortality.
Video available on www.clinicalimagingscience.org
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2014/4/1/28/133263
Source of Support: Nil
Conflict of Interest: None declared.
REFERENCES
- An Overview of History, Pathogenesis and Treatment of Perforated Peptic Ulcer Disease with Evaluation of Prognostic Scoring in Adults. Ann Med Health Sci Res. 2014;4:22-9.
- [Google Scholar]
- Valentino's syndrome a perforated peptic ulcer mimicking acute appendicitis. BMJ Case Rep 2012
- [Google Scholar]
- Images in clinical medicine. Veiled right kidney sign in a patient with Valentino's syndrome. N Engl J Med. 2006;354:e9.
- [Google Scholar]
- A pregnant woman presenting to the ED with Valentino's syndrome. Am J Emerg Med. 2005;23:217-8.
- [Google Scholar]






