Translate this page into:
Unusual Locations of Pancreatic Pseudocysts in Lumbar Triangle, Psoas Muscle and Intercostal Space, and Obturator Externus
-
Received: ,
Accepted: ,
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Pancreatic pseudocyst develops as a complication of both acute and chronic pancreatitis. Although the common location of pseudocyst is lesser sac, extension of pseudocyst can occur into mesentery, retroperitoneum, inguinal region, scrotum, liver, spleen, mediastinum, pleura, and lung. Extension of pseudocyst into psoas muscle and lumbar triangle is extremely rare. The development of pseudocyst in lumbar triangle is radiologically equivalent and further extension of Grey Turner's sign seen clinically in acute pancreatitis. This extension occurs due to the destructive nature of pancreatic enzymes. The lumbar triangle is the site of anatomic weakness in the lateral abdominal wall in the lumbar region. We report the case of a 35-year-old alcoholic male patient who presented with abdominal pain followed by distension and swelling in the right lumbar region for 1 week. On computed tomography scan of the abdomen, acute-on-chronic pancreatitis with multiple pseudocysts in the right posterior pararenal space, extending through the right lumbar triangle in the right lateral abdominal wall, right posterior paraspinal muscles, right iliopsoas, right obturator externus, and medial aspect of the right upper thigh, beneath anterior abdominal wall in the upper abdomen and in the right lateral thoracic wall through the right 11th intercostal space, was detected.
Keywords
Intercostal space
lumbar triangle
obturator externus
pancreatitis
pseudocyst
psoas muscle

INTRODUCTION
Pancreatic pseudocyst develops as a complication of pancreatitis.[1] The estimated prevalence of pancreatic pseudocyst in acute pancreatitis is 5%–16%, while in chronic pancreatitis, it is 30%–40%.[1]
The most commonest location of pancreatic pseudocyst is lesser sac; however, an extension of pseudocyst into mesentery, retroperitoneum, inguinal region, scrotum, liver, spleen, mediastinum, pleura, and lung has been described. Extension into psoas is extremely rare with very few cases described in literature.[12] Extension of pancreatic pseudocysts into psoas muscle, lumbar triangle, intercostal space, and obturator externus is extremely rare. Extension of pseudocysts in lumbar triangle and intercostal space has not been reported yet.
CASE REPORT
A 35-year-old male known alcoholic patient presented with pain in the abdomen for 1 month with abdominal distention for 2 weeks and swelling in the right lumbar region for 1 week. There was no history of fever and vomiting. There were no bladder or bowel complaints. On laboratory investigations, serum amylase was 1028 units/100 ml (reference range: 0–90), serum lipase was 254 IU/L (reference range: 0–60), and serum bilirubin was 0.6 mg/dl (reference range: 0.1–1.2). Serum glutamic-oxaloacetic transaminase, serum glutamic pyruvic transaminase, and serum alkaline phosphatase levels were normal.
Ultrasonography of the abdomen showed marked ascites with multiple septations and collection in right psoas muscle with extension in the lumbar region.
Computed tomography scan of the abdomen and pelvis showed bilateral basal pleural effusion, with the relaxation collapse consolidation noted in the right lower-lobe basal segments. Ascites was noted in the abdomen and pelvis. The pancreas appeared slightly bulky and showed a normal enhancement in contrast study. The pancreatic duct showed mild dilatation, 3 mm in the entire extent. No ductal calculus or parenchymal calcification was noted.
Large, thin-walled, well-defined fluid collection was noted in the retroperitoneum in the right posterior pararenal space posterior to the right kidney and right renal vein and artery which were compressed and displaced anterolaterally. Medially, it was extending between the aorta and inferior vena cava (IVC) compressing and displacing IVC anteriorly. Laterally, it was extending through the right lumbar triangle into the right lateral abdominal wall in the subcutaneous fat plane. It was extending into the right posterior paraspinal muscles and right iliopsoas muscle inferiorly up to its insertion at the greater trochanter of femur. Multiple pseudocysts were also noted in the right obturator externus. Multilocular cysts were noted within muscles on medial aspect of the right upper femur. Cysts in the right iliacus and right psoas were multilocular with multiple thin septations. Cyst in the right posterior pararenal space was extending superiorly posterior to the right hepatic lobe which was compressed and displaced anteriorly [Figures 1–3]. The walls of the cysts showed a mild enhancement in contrast study and measured 2 mm in thickness. All these cysts appeared to be communicating with each other and were multilocular. Cyst in the right posterior pararenal space measured approximately 12.4 cm × 8.8 cm, cyst in the right lumbar region measured approximately 16 cm × 12.5 cm, cyst in the right psoas measured approximately 8.5 cm × 6 cm, cyst in the right iliacus measured approximately 8.5 cm × 5.7 cm, cyst in the right obturator externus measured approximately 10.7 cm × 0.9 cm, and cyst in the right upper thigh measured approximately 5.4 cm × 3.4 cm at widest dimensions [Figures 4 and 5]. Filling defect was noted in portal vein measuring approximately 0.7 cm × 0.7 cm – suggestive of thrombosis with multiple collaterals at the porta hepatis. The findings were suggestive of acute-on-chronic pancreatitis with multiple pseudocysts in the right posterior pararenal space, extending through the right lumbar triangle in the right lateral abdominal wall [Figure 6], right posterior paraspinal muscles, right iliopsoas, right obturator externus, and medial aspect of the right upper thigh, beneath anterior abdominal wall in the upper abdomen. Extension of pseudocyst was also noted between the right 11th and 12th ribs through intercostal space into the adjoining right lateral thoracic wall [Figure 6]. There was portal vein thrombosis with portal cavernoma. The patient was managed conservatively as he was not willing for any surgical intervention.
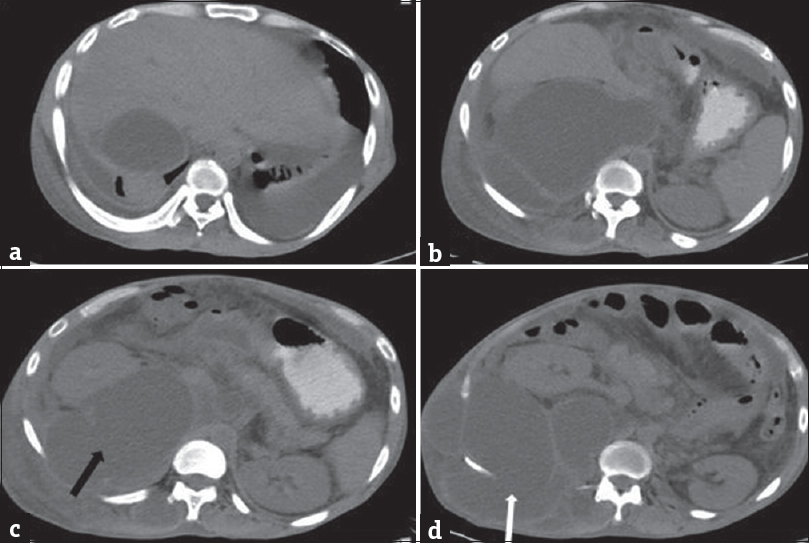
- A 35-year-old male with acute-on-chronic pancreatitis with pseudocysts, who presented with abdominal pain and distention with lump in the right lateral abdominal wall. Plain computed tomography scan of the abdomen showing pseudocyst in the right posterior pararenal space (black arrow) extending into the right lumbar triangle (white arrow).
- A 35-year-old male with acute-on-chronic pancreatitis with pseudocysts, who presented with abdominal pain and distention with lump in the right lateral abdominal wall. Plain computed tomography scan of the abdomen showing pseudocyst in the right lumbar triangle (black arrow).
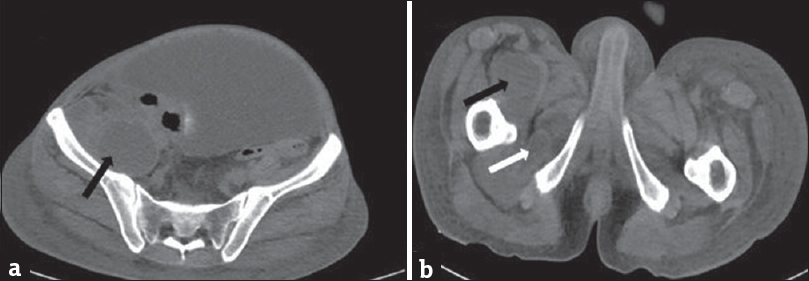
- A 35-year-old male with acute-on-chronic pancreatitis with pseudocysts, who presented with abdominal pain and distention with lump in the right lateral abdominal wall. Plain computed tomography scan of the abdomen showing (a) pseudocyst in the right ilio-psoas (black arrow) and (b) right obturator externus (white arrow).

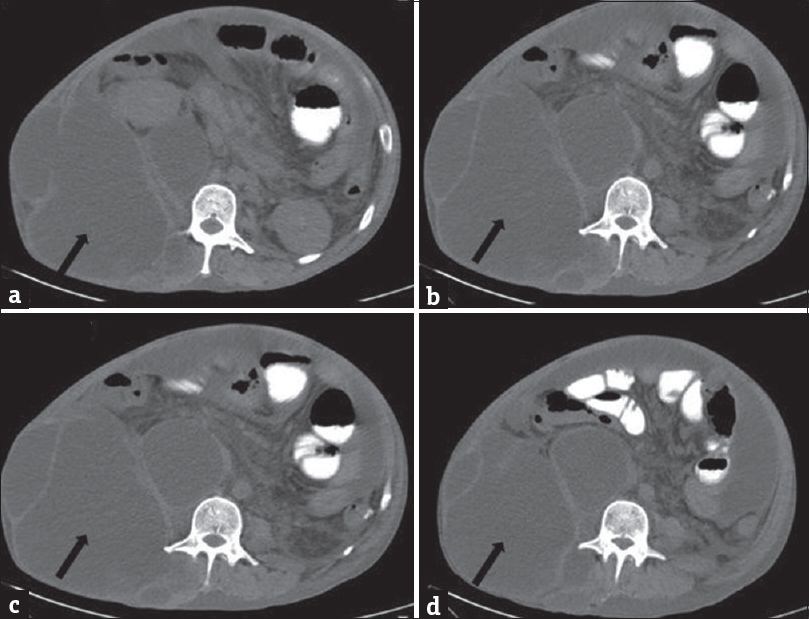
- A 35-year-old male with acute-on-chronic pancreatitis with pseudocysts, who presented with abdominal pain and distention with lump in the right lateral abdominal wall. Contrast-enhanced computed tomography scan of the abdomen showing pseudocyst in the right posterior pararenal space extending into the right lumbar triangle (black arrow) (a-c) and right ilio-psoas (white arrow) (c and d).
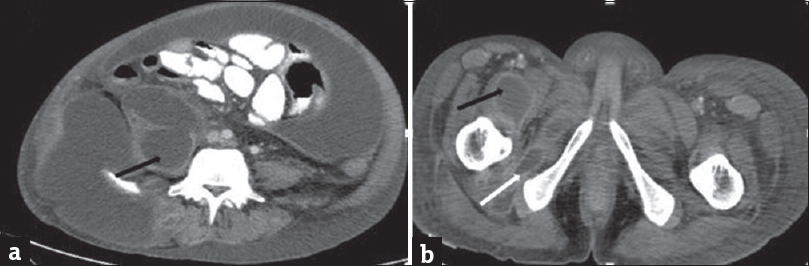
- A 35-year-old male with acute-on-chronic pancreatitis with pseudocysts, who presented with abdominal pain and distention with lump in the right lateral abdominal wall. Contrast-enhanced computed tomography scan of the abdomen showing pseudocyst in the right psoas muscle (black arrow) and right obturator externus (white arrow).
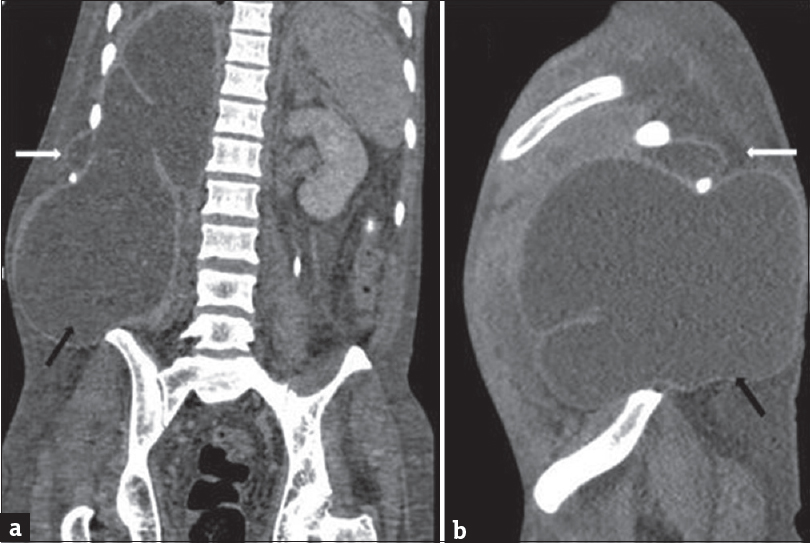
- A 35-year-old male with acute-on-chronic pancreatitis with pseudocysts, who presented with abdominal pain and distention with lump in the right lateral abdominal wall. Coronal (a) and sagittal (b) computed tomography scan images showing pseudocyst in the right posterior pararenal space extending through the intercostal space (white arrow) and right lumbar triangle (black arrow).
DISCUSSION
In acute pancreatitis, there is disruption of the pancreatic ductal system with resultant extension of pancreatic enzymes in the peri-pancreatic tissue with formation of fluid collection. The localized fluid collection is walled off by granulation tissue, forming a pseudocyst.[1]
According to the revised Atlanta classification, pancreatic pseudocyst develops in acute interstitial edematous pancreatitis after 4 weeks.[3] Due to the destructive nature of pancreatic enzymes, a pseudocyst may extend anywhere from the neck, mediastinum, and to the groin.[2]
The development of pseudocyst in lumbar triangle is radiologically equivalent and further extension of Grey Turner's sign seen clinically in acute pancreatitis. There is an extension of pancreatic enzymes and fluid collection in anterior pararenal space which dissects between the two leaves of posterior renal fascia and subsequently to the lateral edge of quadratus lumborum. A communication is established between the posterior pararenal space and structure of flank wall. The lumbar triangle is the site of anatomic weakness in the lateral abdominal wall in lumbar region.[4]
The lumbar region is defined superiorly by the 12th rib, inferiorly by the iliac crest, medially by the erector spinae, and laterally by the posterior border of the external oblique muscle.[4] Defects in the lumbar musculature or aponeurosis in lumbar triangle result in larger superior triangle of Grynfelt–Lesshaft hernia inferior to the 12th rib and smaller inferior triangle of Petit, just cranial to the iliac crest. The floor of the superior lumbar triangle is formed by the outer third of quadratus lumborum muscle and transversalis fascia. The floor of the inferior lumbar triangle is formed by the internal oblique and transverse abdominis muscle.[4]
As the lumbar triangle is a weakness, it can lead to lumbar hernias. Similarly, these structural defects predispose to transmission of extravasated pancreatic enzymes in the subcutaneous tissue of the flank with resultant pseudocyst formation. In acute pancreatitis, the peripancreatic fluid collection extends into the anterior and posterior pararenal spaces and extends through a cleft between the medial border of posterior pararenal space and lateral border of quadratus lumborum fat pad into the transversalis fascia and lumbar triangle.[4]
Extension of pancreatic pseudocyst in psoas muscle is rare. Pancreatico-psoas fistula commonly affects the right psoas muscle. It occurs as a complication of chronic pancreatitis and rarely following an attack of severe acute pancreatitis.[15] Our case is of acute-on-chronic pancreatitis with the extension of pseudocyst in the right psoas muscle and in the right lateral abdominal wall, which is rare.
Usually, pancreatic pseudocysts are managed conservatively, with more than 50% undergoing spontaneous resolution.[6] Pseudocysts become symptomatic if there is an infection, pain, and compression of adjacent structures. These are managed by image-guided percutaneous aspiration.[67] Only size is not an absolute criterion for its drainage. Image-guided percutaneous aspiration or drainage has the advantage of drainage of pancreatic secretions with minimally invasive methods. An endoscopic or internal drainage is needed in case of nonavailability of window to negotiate a pig tail catheter on imaging.
CONCLUSION
Pancreatic pseudocysts can be seen in unusual locations such as psoas muscle, lumbar triangle, iliacus, and obturator externus. Search for pancreatitis should be sought for when localized fluid collection is detected at these sites.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2018/8/1/33/239706
REFERENCES
- Pancreatico-psoas fistula: A rare complication of acute pancreatitis. BMJ Case Rep 2012 2012 pii: bcr1120115083
- [Google Scholar]
- Huge pancreatic pseudocyst migrating to the psoas muscle and inguinal region. Surgery. 2009;145:341-2.
- [Google Scholar]
- The revised Atlanta classification of acute pancreatitis: Its importance for the radiologist and its effect on treatment. Radiology. 2012;262:751-64.
- [Google Scholar]
- Grey turner's sign and Cullen's sign in acute pancreatitis. Gastrointest Radiol. 1989;14:31-7.
- [Google Scholar]
- Extension of pancreatic pseudocyst into psoas muscle in a setting of acute pancreatitis. BMJ Case Rep 2015 2015 pii: bcr2014207822
- [Google Scholar]






