Translate this page into:
Ipsilateral Medial and Lateral Discoid Menisci: A Rare Combination of Infrequent Anatomic Variants

*Corresponding author: Jonathan R. Wood, Department of Radiology, Tripler Army Medical Center, Honolulu, Hawaii, USA. jonathan.r.wood.mil@mail.mil
-
Received: ,
Accepted: ,
How to cite this article: Farlett J, Wood JR. Ipsilateral medial and lateral discoid menisci: A rare combination of infrequent anatomic variants. J Clin Imaging Sci 2020;10:11.
Abstract
A discoid meniscus is a thick, disk-shaped meniscus which is prone to tearing, degeneration, and loss of stability in the knee. A discoid meniscus most commonly affects the lateral meniscus, rarely the medial meniscus. Here, we present a case of an extremely rare medial and lateral discoid meniscus in the ipsilateral knee of a 10-year-old male. Ipsilateral medial and discoid menisci are incredibly rare and one must keep this entity in mind to avoid confusion while interpreting knee magnetic resonance imaging.
Keywords
Discoid meniscus
Medial discoid meniscus
Lateral discoid meniscus
INTRODUCTION
Discoid medial and lateral menisci in an ipsilateral knee are an extremely rare finding. To the best of our knowledge, only six cases have been reported in the literature to date.[1] The meniscus, due to their semilunar shape, adds stability to the knee as well as is thought to reduce stress and friction from motion. A discoid meniscus is an anatomic variant which reduces the stability of the knee and has higher rates of tearing and degenerating. Ipsilateral medial and lateral discoid menisci are incredibly rare. Knowledge of this entity is crucial as discoid menisci are frequently torn or contain abundant intrasubstance degeneration which may lead to confusion while interpreting the examination.
CASE REPORT
A 10-year-old male presented to the emergency department with chronic left knee pain. The pain was aggravated by kneeling and running, but was not present at rest. No limping or swelling was noticed by the patient or his mother. On examination, the left lower extremity was without erythema, edema, or ecchymosis. Pain was elicited by pressing on the medial joint line. The knee was stable to varus and valgus stress at 0 and 30° of knee flexion. Sensation was intact. The left knee radiographs demonstrated no acute findings, although there was increased distance qualitatively of the medial and lateral tibiofemoral compartments [Figure 1]. Magnetic resonance imaging (MRI) demonstrated incomplete lateral discoid menisci. In addition, there was a mass identified in the medial tibiofemoral compartment, which on closer inspection was contiguous with the medial meniscus, consistent with a complete medial discoid meniscus [Figure 2a and b]. In addition, there was a complex horizontal tear of the medial meniscus, extending into the posterior root attachment [Figure 2c].
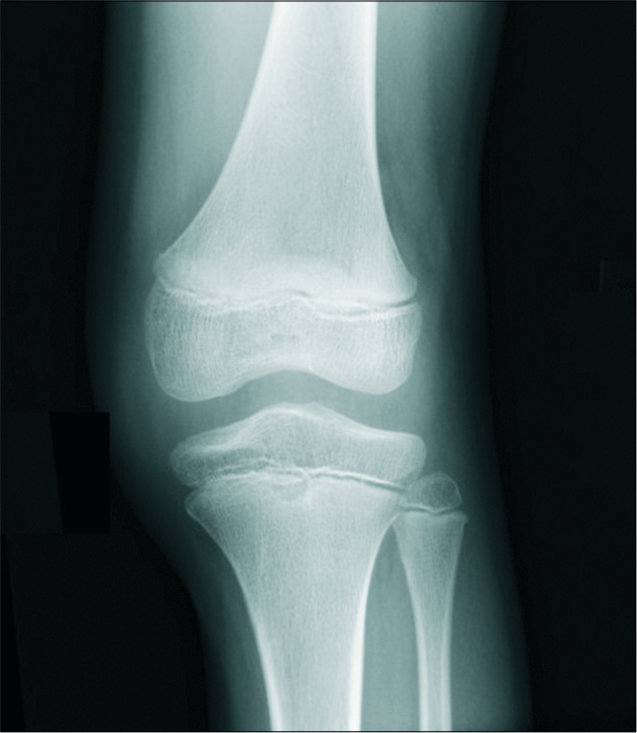
- A 10-year-old male with chronic left knee pain. Anteroposterior radiograph of the left knee shows widened medial and lateral tibiofemoral compartments, which can be seen with discoid menisci.
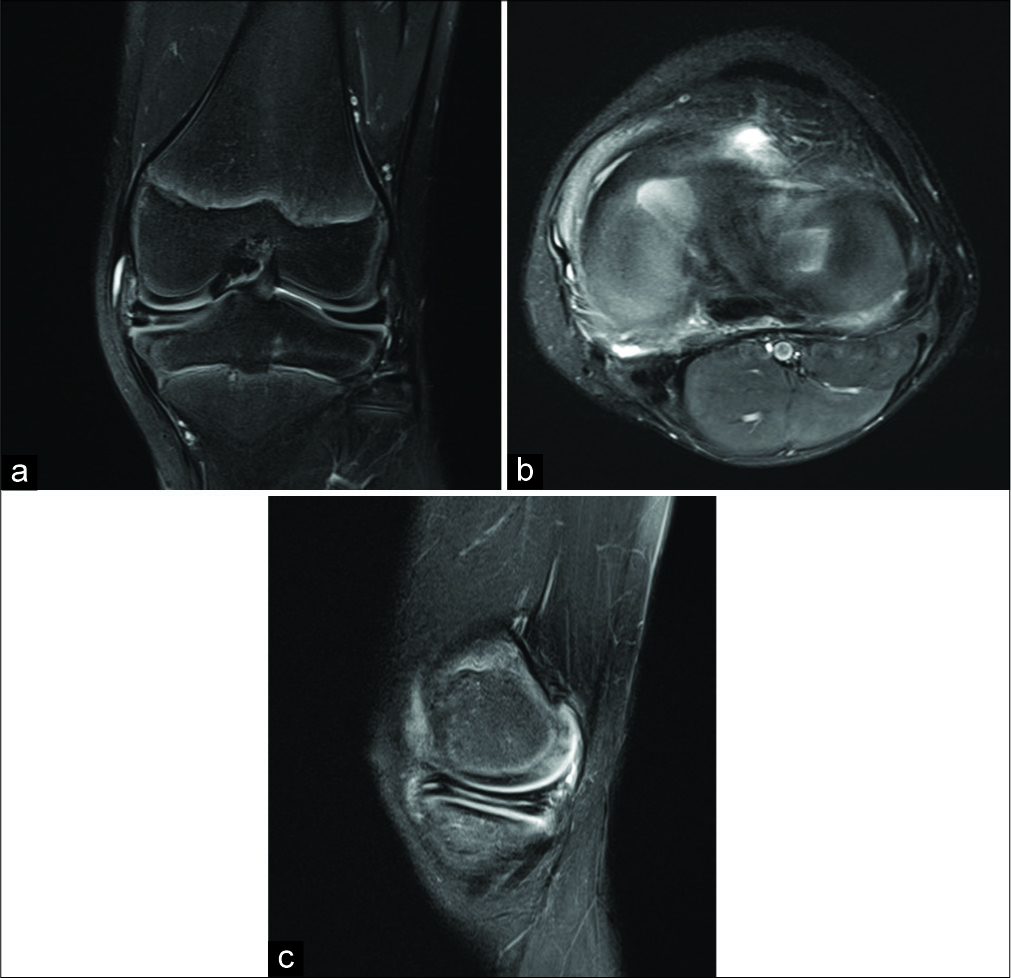
- (a) A 10-year-old male with chronic left knee pain. Coronal fluid weighted fat-saturated sequence shows a complete medial and incomplete lateral discoid meniscus. There is also a horizontal tear of the medial meniscus, (b) axial fluid weighted fat- saturated sequence shows a complete medial and incomplete lateral discoid meniscus, (c) sagittal fluid weighted fat-saturated sequence shows a horizontal tear of the medial discoid meniscus which propagated into the posterior root attachment.
The patient was taken for arthroscopy based on symptoms and MRI findings. Medial plica debridement and medial meniscal saucerization and repair were performed [Figure 3a and b]. The medial meniscus was the focus for intervention as the patient had a medial meniscal tear and was symptomatic on the medial side. The lateral meniscus was not fully investigated [Figure 3c]. There were no post-operative complications, and the patient is now full weight-bearing 4-month post-operative.
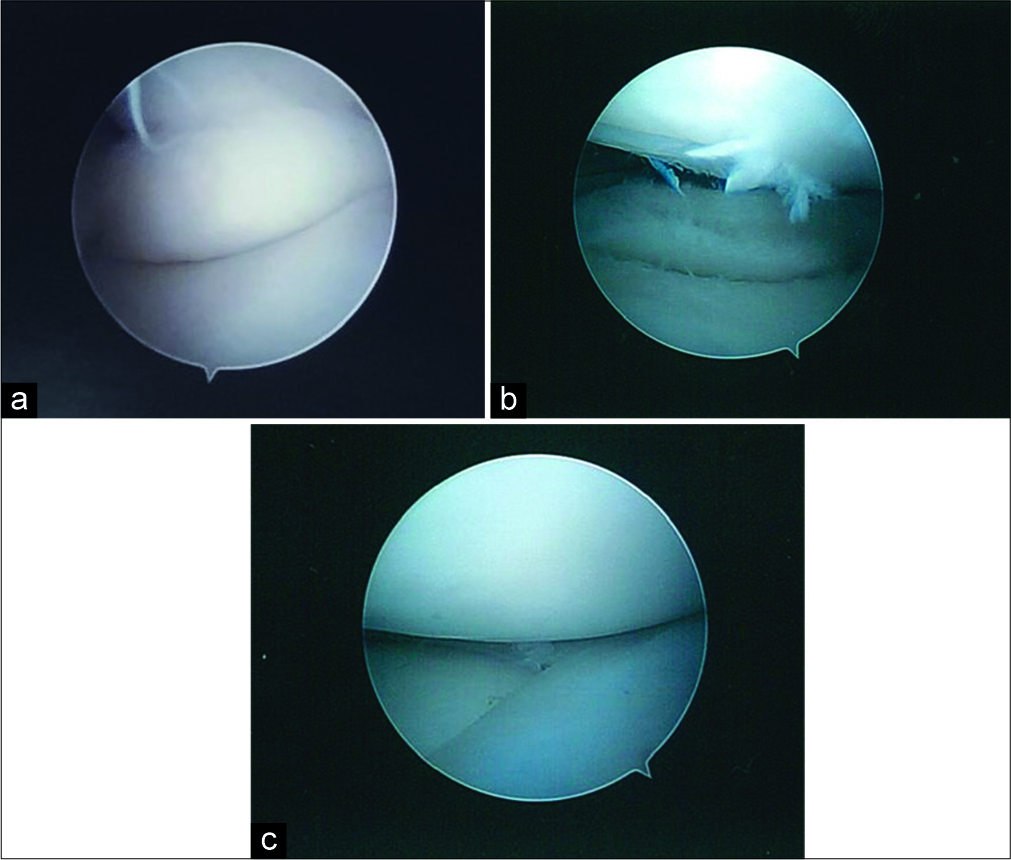
- (a) Arthroscopic view of the medial discoid meniscus between the medial femoral condyle and tibial plateau with the knee slightly extended. The femoral condyle pushed the posterior horn of the discoid meniscus into the joint. (b) Arthroscopic view of the medial discoid meniscus s/p saucerization revealing the horizontal tear noted on magnetic resonance imaging. (c) Arthroscopic view of the lateral discoid meniscus. This meniscus was not as markedly discoid as the medial meniscus.
DISCUSSION
Discoid menisci are thick and disk shaped, making them prone to tearing, degeneration, and loss of stability in the knee. The lateral meniscus is more commonly affected than the medial.[2,3] A discoid medial meniscus is much less common, with a prevalence of only 0.03–0.3% while the prevalence of a lateral discoid meniscus is 3–5%.[4] They have been only a handful of cases reported with both medial and lateral discoid menisci in an ipsilateral knee.
The discoid meniscus is an abnormally developed meniscus that is thicker and extends further onto the tibial plateau, establishing its disk-like shape. Discoid menisci are typically diagnosed on MRI after suspicious history of chronic knee pain and physical examination findings. On MRI, normal menisci are hypointense and typically appear as a “bow-tie” sign on two consecutive 5 mm sagittal MRI images. Three or more consecutive sagittal sections of the bow-tie sign are suspicious for discoid meniscus. On coronal sections, diagnosis can be made when the width is 15 mm or greater.
The Watanabe classification categorizes discoid menisci into three categories: Complete, incomplete, or the Wrisberg variant. Complete type is when the meniscus extends over more than 80% of the tibial plateau. Incomplete discoid menisci extend over <80% of the tibial plateau. The Wrisberg variant is characterized by the lack of the typical posterior meniscocapsular attachments as well as the coronary ligamentous attachments to the tibia and is, therefore, only attached posteriorly by the Wrisberg ligament.[5] This predisposes to instability of the discoid meniscus, leading to meniscal tears and joint instability and degeneration.
CONCLUSION
We report an extremely rare case of ipsilateral medial and lateral discoid menisci. Although uncommon, it is crucial to keep this entity in mind while interpreting knee MRI. The findings of increased size of the medial and lateral tibiofemoral compartments should also raise the suspicion for underlying discoid menisci. Lateral discoid menisci are easily identified, although a concomitant medial discoid meniscus may be misinterpreted, given their rarity. These menisci are frequently torn or degenerated which can give them a confusing and irregular appearance.
Acknowledgement
The views expressed in this manuscript are those of the authors and do not reflect the official policy or position of the Department of the Army, Department of Defence, or the United States Government. The authors have no financial, personal, or other vested interests in the information contained within this document.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Ipsilateral medial and lateral discoid meniscus with medial meniscus tear. J Orthop Case Rep. 2016;6:9-12.
- [CrossRef] [PubMed] [Google Scholar]
- Discoid menisci of the knee: MR imaging appearance. Radiology. 1989;173:351-4.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence of abnormal findings in magnetic resonance images of asymptomatic knees. J Orthop Sci. 2002;7:287-91.
- [CrossRef] [PubMed] [Google Scholar]
- Lateral meniscal variants: Evaluation and treatment. J Am Acad Orthop Surg. 1996;4:191-200.
- [CrossRef] [PubMed] [Google Scholar]






