Translate this page into:
Chronic esophageal dissection: Delayed diagnosis in a 15-year-old male

*Corresponding author: Nilesh Vakharia, Department of Head and Neck Surgery, University College London Hospitals NHS Foundation Trust, London, United Kingdom. nilesh.vakharia@nhs.net
-
Received: ,
Accepted: ,
How to cite this article: Vakharia N, Nadeeka Sirisena UD, Mandalia U. Chronic esophageal dissection: Delayed diagnosis in a 15-year-old male. J Clin Imaging Sci 2022;12:16.
Abstract
Esophageal dissection is a rare condition, characterized by disruption of the submucosa from the muscular layer of the esophageal wall. It is commonly iatrogenic in etiology and patients typically present with acute onset dysphagia, odynophagia, and retrosternal pain. The condition can be diagnosed endoscopically; however, contrast swallow studies either with CT or fluoroscopy carry less risk and are the imaging investigations of choice for this condition. Patients are managed conservatively in the majority of cases. In this case report, we present a case of chronic esophageal dissection in a 15-year-old male who had undergone endoscopic removal of a foreign body from the esophagus several years prior. We discuss the clinical features, radiological diagnosis, and management of this condition.
Keywords
Esophageal dissection
Dysphagia
Contrast swallow
Fluoroscopy
INTRODUCTION
Esophageal dissection, first described as “esophageal laceration” in 1957 by Williams, is the disruption of the submucosal space of the esophagus, resulting in the formation of a hematoma within the esophageal wall.[1] Other terms in the literature for this condition include esophageal hematoma, dissecting hematoma, spontaneous intramural rupture, and esophageal apoplexy.[2] Esophageal dissection is most commonly seen in female patients and in the seventh or eighth decade,[3] with coagulation abnormalities reported in one-third of cases.[2] It most commonly presents with acute retrosternal or epigastric pain, along with dysphagia, odynophagia, and small volume hematemesis.[4] Causes are most commonly iatrogenic (including endoscopy and nasogastric tube insertion), sudden pressure changes in the esophagus, blunt trauma, and rarely, idiopathic. More recently, esophageal dissection associated with eosinophilic oesophagitis is increasingly recognized.[5] We describe a unique case of esophageal dissection in a 15-year-old male, with no preexisting medical conditions, presenting 7 years after the causative intervention.
CASE REPORT
A 15-year-old male was referred to Ear, Nose and Throat (ENT) surgeons at their local hospital with a prolonged history of dysphagia, throat spasms, and poor weight gain. His symptoms started following the endoscopic removal of a tablet lodged in his throat, 7 years prior. He had no preexisting medical conditions nor a history of coagulopathy.
A contrast swallow study, using barium, was performed. This demonstrated the presence of a false passage within the esophageal wall [Figures 1a-c]. Based on this imaging study, a diagnosis of esophageal dissection was made.
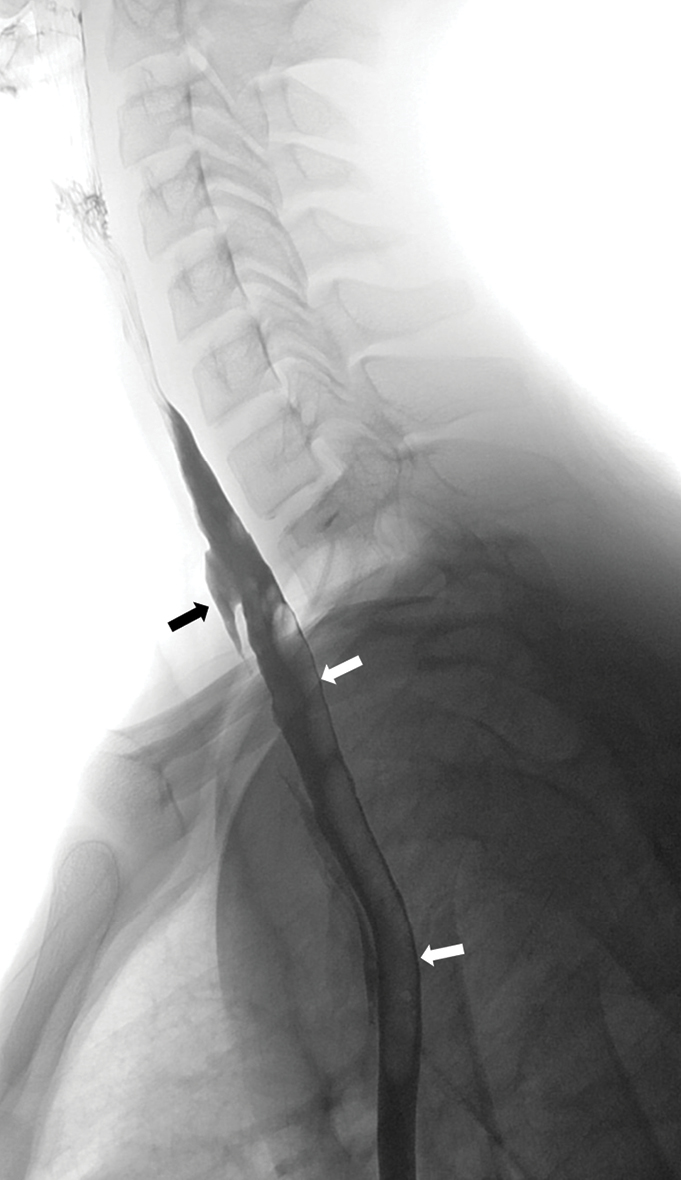
- A 15-year-old boy was referred for a barium swallow investigation as part of a workup for chronic dysphagia and odynophagia. His symptoms commenced after the endoscopic removal of an impacted tablet several years earlier. (a) A lateral projection of the thorax demonstrates barium within the true lumen of the esophagus (white arrows) and a defect within the anterior esophageal mucosa through which there is the passage of barium into a false passage (black arrow); features consistent with an oesophageal dissection.
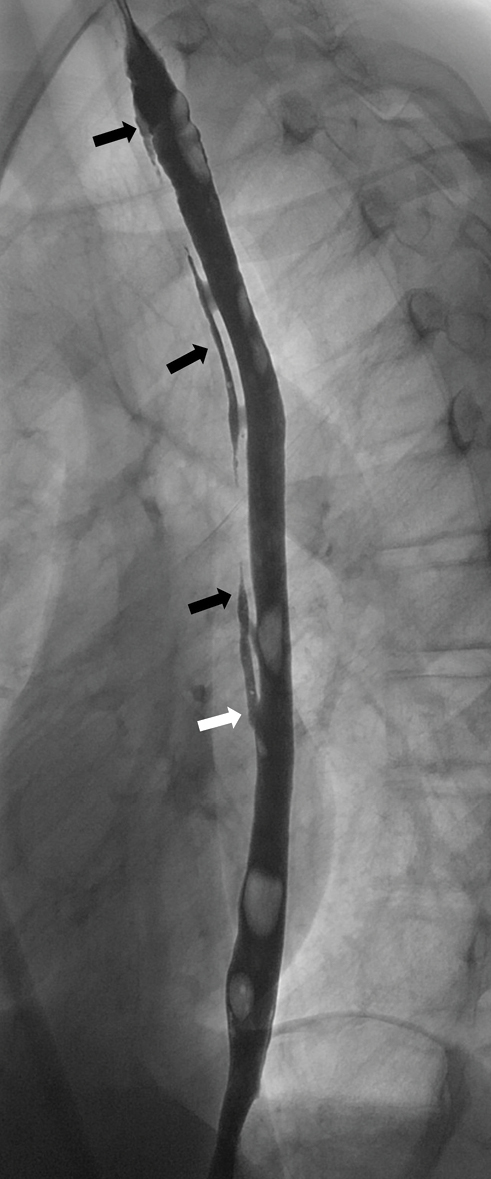
- A 15-year-old boy was referred for a barium swallow investigation as part of a workup for chronic dysphagia and odynophagia. His symptoms commenced after the endoscopic removal of an impacted tablet several years earlier. (b) A lateral image of the full length of the thoracic esophagus demonstrates the entirety of the esophageal dissection and a so-called “double-barrel esophagus” (black arrows). The false lumen is seen to merge distally into the true lumen (white arrow).
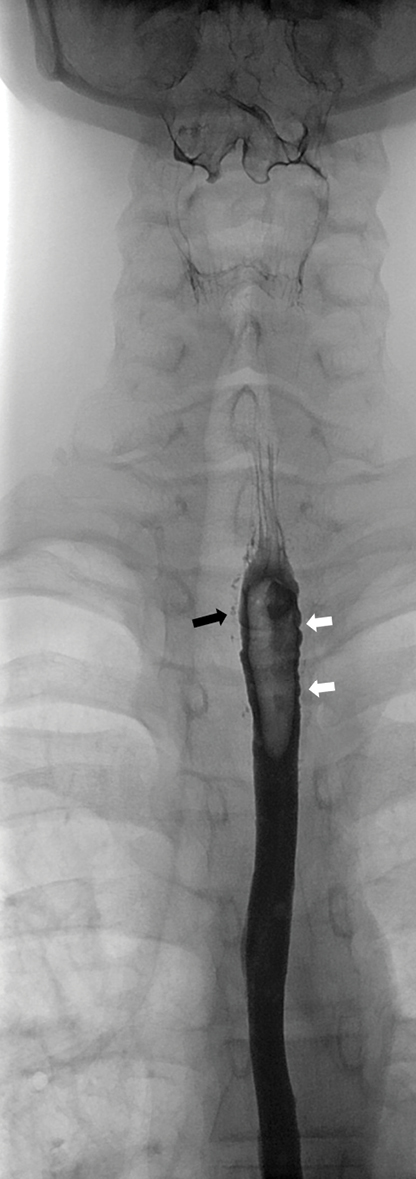
- A 15-year-old boy was referred for a barium swallow investigation as part of a workup for chronic dysphagia and odynophagia. His symptoms commenced after the endoscopic removal of an impacted tablet several years earlier. (c) An AP projection of the esophagus, from the same study, shows traces of contrast in the false lumen (black arrow) and evidence of dysmotility, characterized by nonperistaltic contractions at the site of dissection.
Due to the long duration since the initial iatrogenic injury, the risk of perforation was thought to be low and conservative treatment was considered. However, given the longstanding symptoms and the effect on the child’s nutrition, a decision was made to proceed with definitive endoscopic repair at a specialist pediatric unit.
DISCUSSION
Following a review of the literature, we describe a unique case of chronic esophageal dissection, presenting 7 years after the endoscopic intervention to remove a lodged tablet. Whilst there have been previous reports of esophageal dissection secondary to pill-related ulceration,[6] in this case, no ulceration of the esophageal mucosa was noted at the time of endoscopy to remove the tablet. Esophageal dissection typically presents with acute pain and dysphagia, which would ordinarily prompt timely presentation for medical review. However, in the case we have described, the clinical presentation differs from reports in the literature as our patient had insidious but progressive symptoms of dysphagia, throat spasms, and subsequent poor weight gain. As a result, referral to an ENT specialist was delayed for several years.
The youngest reported case of esophageal dissection in the literature is of an 11-year-old boy with eosinophilic oesophagitis.[7] Given that the patient in our case had the causative intervention 7 years prior to diagnosis, he is likely to have sustained esophageal dissection at 8 years of age which would be the youngest case of iatrogenic esophageal dissection in the literature.
Diagnosis of esophageal dissection can be made on endoscopy, where a mucosal tear may be noted, along with a false lumen, blue discoloration of the esophageal wall, and separation of the submucosal layer from the muscular wall. However, there is a risk that endoscopy may worsen the esophageal dissection and result in perforation.[2] Fluoroscopic investigation in the form of a contrast swallow, with barium or water-soluble contrast, is safe, readily available, and easily performed with relatively low radiation exposure, which makes it the imaging modality of choice. A contrast swallow typically shows a mucosal stripe or a “double-barrel esophagus.” Whilst CT imaging is often more readily available and may also show a double lumen, fine dissection tracks may be missed and the radiation exposure may be more. However, contrast-enhanced CT may be useful to identify other findings including esophageal wall thickening, intramural masses, and submucosal hematoma.[8] CT can also assess for associated complications of dissection such as esophageal perforation or mediastinal collection. In this case, barium swallow alone was sufficient to establish the presence of an esophageal dissection.
Initial management of esophageal dissection is typically conservative, keeping the patient nil-by-mouth, feeding via parenteral nutrition or nasogastric tube, along with broad spectrum antibiotic cover and proton pump inhibitors.[3] Surgical or endoscopic management is reserved for those in which conservative management fails or those who develop complications such as esophageal perforation. Perforation secondary to an intramural dissection is rare and most often seen during instrumentation in an acute setting, for example, to remove an obstructing food bolus.[9] In the absence of perforation, endoscopic division of the mucosal septum between the true and false lumens has been successful in management of esophageal dissection.[2] In cases with associated perforation, options for operative management include primary closure of the defect or esophageal resection with reconstruction in the stable patient, or T-tube drainage in the unstable patient.[3] In the case we describe, the esophageal dissection went undiagnosed, resulting in the patient continuing oral intake for many years, albeit with difficulty and resulting in poor weight gain. We postulate that continued oral intake is likely to have prevented the mucosal flap from repairing as expected in an otherwise healthy patient, allowing the false channel to remain patent until the patient was diagnosed and treated. As a result, conservative management was not deemed likely to be successful, and the child was referred for specialist endoscopic repair, despite the risk of acute and chronic complications of perforation and stricture formation.[10]
CONCLUSION
Esophageal dissection is a rare condition that usually presents with acute onset retrosternal or epigastric pain, dysphagia, and hematemesis. We present an atypical, presentation of a child with chronic esophageal dissection which, to the best of our knowledge, has not previously been described. Although it is most commonly reported in older, female patients, it can occur in the pediatric age range. It is an important differential in all patients with a history of dysphagia following esophageal instrumentation. Contrast swallow studies either with fluoroscopy or CT are able to delineate a false channel, the diagnostic feature of esophageal dissection. Chronic esophageal dissection is unlikely to resolve with conservative management and referral for specialist surgical repair is advised.
Declaration of patient consent
Patient’s consent is not required as patient’s identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Oesophageal laceration following remote trauma. Br J Radiol. 1957;30:666-8.
- [CrossRef] [PubMed] [Google Scholar]
- Iatrogenic intramural esophageal dissection and perforation: Causes, clinical course, and management. Am Surg. 2015;81:E57-E60.
- [PubMed] [Google Scholar]
- Endoscopic and radiological features of intramural esophageal dissection. Endoscopy. 2001;33:379-81.
- [CrossRef] [PubMed] [Google Scholar]
- Recurrent spontaneous esophageal dissection. J Soc Laparoendosc Surg. 2014;18:342-5.
- [CrossRef] [PubMed] [Google Scholar]
- Pill-related esophageal intramural dissection treated by an endoscopic procedure. Gastrointest Endosc. 2011;74:1422-4.
- [CrossRef] [PubMed] [Google Scholar]
- Circumferential mucosal dissection and esophageal perforation in a patient with eosinophilic esophagitis. World J Gastroenterol. 2008;14:803-4.
- [CrossRef] [PubMed] [Google Scholar]
- Intramural hematoma of the esophagus: A pictorial essay. Emerg Radiol. 2008;15:13-22.
- [CrossRef] [PubMed] [Google Scholar]
- Intramucosal esophageal dissection leading to esophageal perforation: Case report and review of the literature. Gastroenterol Hepatol. 2008;4:362-5.
- [PubMed] [Google Scholar]
- Circumferential intramural esophageal dissection successfully treated by endoscopic procedure and metal stent insertion. J Gastroenterol. 2005;40:1065-9.
- [CrossRef] [PubMed] [Google Scholar]






