Translate this page into:
Two Cases of Thyroid Metastasis from Head and Neck Squamous Cell Carcinoma Detected by FDG-PET/CT
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
We present two cases of head and neck squamous cell carcinoma (SCC) metastasizing to the thyroid gland. This is the first report that shows (18) F-fluorodeoxyglucose-positron emission tomography/computed tomography (FDG-PET/CT) images of tonsillar and supraglottic SCCs invading the thyroid gland. Alcohol and tobacco use are the two most important risk factors for head and neck cancers, but recently human papilloma virus (HPV) infection has become a significant risk factor in the United States. FDG-PET/CT is very useful for SCC staging/restaging and follow-up.
Keywords
(18) F-fluorodeoxyglucose-positron emission tomography/computed tomography
squamous cell carcinoma
supraglottic
thyroid
tonsillar
INTRODUCTION

Squamous cell carcinoma (SCC) of the head and neck represents 4% of all diagnosed neoplasms worldwide.[1] In the United States, head and neck SCC accounts for about 3% of all cancers.[1] Alcohol and tobacco use are the two most important risk factors for head and neck cancers. Recently, human papilloma virus (HPV) infection has become a significant risk factor in the United States. HPV-related SCC occurs in young patients. Laryngeal cancers can arise from above the true vocal folds (supraglottic region), below the true vocal folds (subglottic region), or from the true vocal folds (glottic region). Glottic cancers represent greater than 75% of all laryngeal cancers. Head and neck SCC most often metastasizes by the lymphatic route. Hematogenous distant metastasis of head and neck SCC is rare.[2] The lungs are the most common site of distant metastasis, followed by bones, liver, and skin.[2] Selection of treatment for head and neck SCC depends on whether extension of the primary tumor and/or lymph node metastases are present. Death from head and neck SCC is related to metastasis to regional lymph nodes and resistance to treatment.[3]
CASE REPORTS
Case 1
A 58-year-old male complained of difficulty in swallowing. He had a history of Helicobacter pylori infection and was first diagnosed with p16 protein (p16) positive SCC of right tonsil in 2009. He had a 30-year history of smoking. He was treated with cisplatin, cetuximab, and radiation therapy for the T2N2M0 SCC. A new primary SCC of left tonsil was diagnosed in 2011. After this, the patient underwent another round of chemotherapy with cisplatin, cetuximab, and fluorouracil. In May 2013, an (18) F-fluorodeoxyglucose-positron emission tomography/computed tomography (FDG-PET/CT) was done to assess the response to chemotherapy. A 3.4 cm mass was found in the right thyroid gland, which exhibited irregularity, causing deviation of the underlying trachea [Figure 1]. Fine needle aspiration (FNA) of both lobes of the thyroid gland revealed tonsillar SCC.

- Case 1. 58-year-old male with difficulty in swallowing was diagnosed with squamous cell carcinoma of right tonsil. a) Maximum Intensity Projection (MIP) image shows tonsillar SCC infiltration in both lobes of the thyroid gland (arrows). b) Axial CT image for attenuation correction and anatomic localization. c) Axial PET image shows diffuse tracer uptake in both lobes of the thyroid gland (arrows). d) Axial PET/CT fusion image reveals SUVmax of the right and left thyroid lobes was 7.5 and 5.9, respectively (arrows).
Case 2
A 66-year-old male presented with a complaint of a mass in the neck. He was diagnosed with P16 positive T2N2M0, stage 4B supraglottic SCC in December 2012. He has a history of heavy drinking and is a current smoker with a 40-year history of smoking. He was treated with cisplatin and radiation therapy. He was unable to complete the last 3 days of radiation therapy due to persistent emesis. On a restaging FDG-PET/CT in January 2014, a new intensely hypermetabolic, multifocal, infiltrative mass was found in multiple areas of the thyroid gland [Figure 2]. FNA of both lobes of thyroid gland revealed supraglottic SCC. The patient was referred to hospice care.
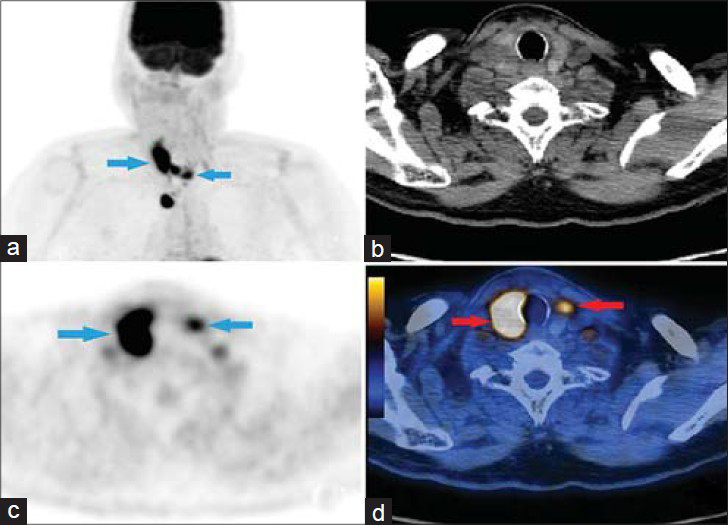
- Case 2. 66-year-old male complaining of a mass in the neck was diagnosed with supraglottic squamous cell carcinoma. a) Maximum Intensity Projection (MIP) image shows supraglottic SCC metastasis in both lobes of the thyroid gland (arrows). b) CT image for attenuation correction and anatomic localization. c) Axial PET image shows intense metabolic activity in both lobes (arrows). d) Axial PET/CT fusion image reveals SUVmax of the right thyroid lobe was 20.3 and SUVmax of the left lobe was 7 (arrows).
DISCUSSION
This is the first report that shows FDG-PET/CT images of tonsillar and supraglottic SCCs invading the thyroid gland. There is only one prior report of tonsillar SCC metastasis to the thyroid and no prior reports of supraglottic SCC metastasis to the thyroid.[4] Patient 1 had treatment with cisplatin, cetuximab, and fluorouracil, and this regimen is a good option for systemic treatment in advanced cases and has a well-tolerated toxicity profile.[1]
Prognostic factors for head and neck SCC include site of disease, node density, and HPV infection. Proper staging can save the patients from undue surgical procedures. FDG-PET/CT allows early diagnosis and staging before morphologic changes are evident. Tobacco- and alcohol-induced carcinogenesis has a synergistic relation with HPV carcinogenesis. Both our patients had extensive history of smoking. There is a strong association between p16 positivity and presence of HPV.[5] In both our patients, p16 was positive; however, they were not tested for HPV. Presence of p16 is associated with favorable prognosis and increased patient survival because the tumors are less aggressive, have higher response rates to chemo-radiation treatment, have less chromosome instability, longer disease-free periods, and the primary tumor size tends to be small.[3] Furthermore, H. pylori has also been implicated in the development of laryngeal SCC, particularly for the supraglottic SCC.[6] Interestingly, patient 1 had a history of H. pylori infection.
CT and MRI are the two most frequently used imaging methods for head and neck SCC. Li et al., reported that tumor volume cannot be accurately assessed by conventional CT imaging.[7] Tumor volume is still being overestimated by CT and MRI, resulting in unnecessary total laryngectomies in a few patients.[7] Bilateral focal FDG uptake was observed in both our patients. This is consistent with the findings by Chen et al., who reported that bilateral focal intense FDG uptake suggests the possibility of malignancy.[8]
A focal thyroid lesion with significant uptake is likely to be malignant, whereas diffuse increased uptake in the thyroid glands favors several thyroidal disorders which include chronic thyroiditis, Graves’ disease, diffuse goiter, and multinodular goiter.[9] The risk of malignancy is as high as 63.6% in thyroid lesions with focal uptake.[10]
CONCLUSION
FDG-PET/CT exam can scan the whole body in one non-invasive exam. Proper staging can save the patients from undue surgical procedures. FDG-PET/CT allows early diagnosis and staging before morphologic changes are evident. Thus, FDG-PET/CT should be used more frequently in the staging/restaging and follow-up of head and neck SCC.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2014/4/1/62/145850
Source of Support: Nil
Conflict of Interest: None declared.
REFERENCES
- Cetuximab plus platinum-based chemotherapy in head and neck squamous cell carcinoma: A retrospective study in a single comprehensive European cancer institution. PLoS One. 2014;9:e86697.
- [Google Scholar]
- Distant muscular (gluteus maximus muscle) metastasis from laryngeal squamous cell carcinoma. Acta Otolaryngol. 2005;125:678-82.
- [Google Scholar]
- Expression of BMI1 and p16 in laryngeal squamous cell carcinoma. Head Neck. 2013;35:847-51.
- [Google Scholar]
- Case report. Isolated intrathyroid metastasis from undifferentiated and squamous carcinoma of the head and neck: The case for surgery and re-irradiation. Br J Radiol. 2008;81:e154-61.
- [Google Scholar]
- Correlation between human papillomavirus and p16 overexpression in oropharyngeal tumours: A systematic review. Br J Cancer. 2014;110:1587-94.
- [Google Scholar]
- Association between infection of virulence cagA gene Helicobacter pylori and laryngeal squamous cell carcinoma. Med Sci Monit. 2013;19:584-91.
- [Google Scholar]
- Spectral CT imaging of laryngeal and hypopharyngeal squamous cell carcinoma: Evaluation of image quality and status of lymph nodes. PLoS One. 2013;8:e83492.
- [Google Scholar]
- The significance of FDG uptake in bilateral thyroid glands. Nucl Med Commun. 2007;28:117-22.
- [Google Scholar]
- Chronic thyroiditis in patients with advanced breast carcinoma: Metabolic and morphologic changes on PET-CT. Eur J Nucl Med Mol Imaging. 2009;36:894-902.
- [Google Scholar]
- Evaluation of thyroid FDG uptake incidentally identified on FDG-PET/CT imaging. Nucl Med Commun. 2009;30:240-4.
- [Google Scholar]






