Translate this page into:
Training for Rural Radiology and Imaging in Sub-Saharan Africa: Addressing the Mismatch Between Services and Population
Address for correspondence: Dr. Michael G Kawooya, ECUREI, c/o Mengo Hospital, Albert Cook Road, Albert Cook Building, P.O. BOX 7161 Kampala, Uganda. E-mail: kawooyagm@yahoo.co.uk
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
The objectives of this review are to outline the needs, challenges, and training interventions for rural radiology (RR) training in Sub-Saharan Africa (SSA). Rural radiology may be defined as imaging requirements of the rural communities. In SSA, over 80% of the population is rural. The literature was reviewed to determine the need for imaging in rural Africa, the challenges, and training interventions. Up to 50% of the patients in the rural health facilities in Uganda may require imaging, largely ultrasound and plain radiography. In Uganda, imaging is performed, on an average, in 50% of the deserving patients in the urban areas, compared to 10–13 % in the rural areas. Imaging has been shown to increase the utilization of facility-based rural health services and to impact management decisions. The challenges in the rural areas are different from those in the urban areas. These are related to disease spectrum, human resource, and socio-economic, socio-cultural, infrastructural, and academic disparities. Countries in Sub-Saharan Africa, for which information on training intervention was available, included: Uganda, Kenya, Tanzania, Rwanda, Zambia, Ghana, Malawi, and Sudan. Favorable national policies had been instrumental in implementing these interventions. The interventions had been made by public, private-for-profit (PFP), private-not-for profit (PNFP), local, and international academic institutions, personal initiatives, and professional societies. Ultrasound and plain radiography were the main focus. Despite these efforts, there were still gross disparities in the RR services for SSA. In conclusion, there have been training interventions targeted toward RR in Africa. However, gross disparities in RR provision persist, requiring an effective policy, plus a more organized, focused, and sustainable approach, by the stakeholders.
Keywords
Rural
radiology
Sub-Saharan Africa
training
INTRODUCTION

Rural radiology is, for purposes of this article, defined as radiology services to communities, residing in areas very isolated from the urban areas. For many Sub-Saharan African (SSA) countries, over 80% of the population is rural.[1] The global health goals cannot be met unless key health needs facing the majority of the world's population are addressed.[23] For a majority of the SSA countries, human resource shortage is the limiting factor to attaining the millennium development goals.[45] Introduction of imaging services in some rural communities has led to increased utilization of facility-based health services,[67] Imaging has also been shown to impact management decisions.[89]
In general, most countries in SSA have few or no radiologists [Table 1], and the majority of these are deployed in the cities and metropolitan areas.[10]
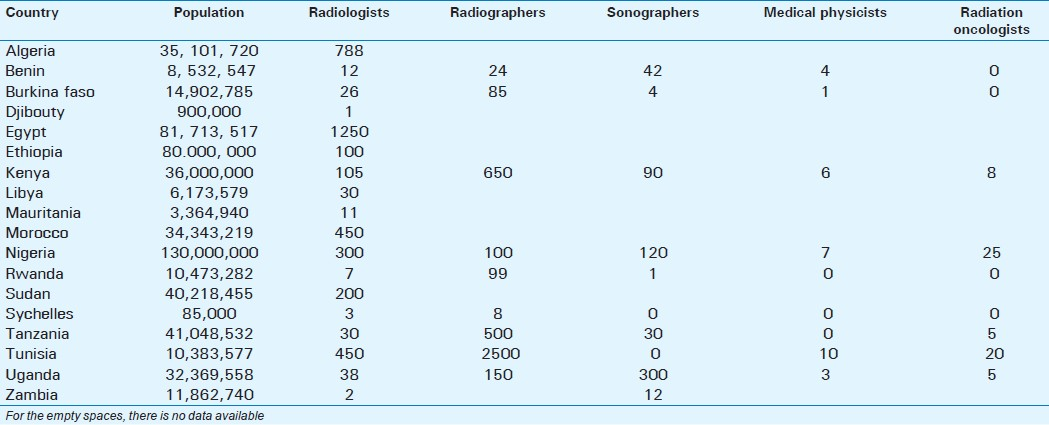
Several players, including national governments, training institutions, and professional bodies have designed interventions for rural radiology (RR).
The objectives of this article are to: Outline the need for RR in SSA, highlight the challenges facing RR training, list the training interventions, evaluate their effectiveness, and propose future strategies.
The more commonly used intervention has been in-service training, to allow for multitasking. This approach takes a shorter time and is cheaper, besides, the trainee already has some basic biomedical sciences and clinical knowledge. Through such in-service training, skills like ultrasound and film interpretation, which are the most needed in rural areas, have been taught. There are, however, disadvantages of this in-service training. There is no increase in the total number of health workers, as such, although there is an increase in the number of those providing RR services. The health worker, who is multitasking may be overloaded by the additional imaging tasks, and this may impinge on the overall performance. Third, the multitasking health worker may change preference to the newly acquired imaging role and neglect the earlier role, thereby creating a deficit in another critical health service area. There are additional challenges in learning new skills, as the health workers often have insufficient foundational knowledge in biomedical sciences, which are necessary for acquiring imaging skills.[11]
Other innovative ways to deal with disparities in human resource for health in rural areas have included scaling up of pre-service training that targets rural health. This is being tried in India, although with some resistance.[1213] This method will be effective, but will take a longer time to produce the required number of rural workers.
Uganda
Uganda's developments in training for RR are guided by the country's health policy. Uganda has a National Health Equipment Policy,[14] which spells out the type and specification of equipment at each health level. As per this policy, there should be an ultrasound machine at the primary health care level (Health Centre 4), serving every 100,000 patients, and one X-ray machine at the level of a General Hospital, serving 200,000 – 300,000 patients. The routine practice is to couple equipment supply and rural health units with a training component. Through such an arrangement, over 300 non-physician health workers from rural areas have been trained in ultrasound and up to 25 in plain x-ray film interpretation, at the Ernest Cook Ultrasound Research and Education Institute (ECUREI), a private health training institution. Uganda's Private–Public partnership policy provided the framework for this training.[15]
Uganda, however, has one unfavorable policy, which negatively impacts rural health provision, including provision of imaging services. The country sets a ceiling on its health budget, with a result that only 30% of the budget for health is funded, and this impacts the training and service provision for rural imaging, consequently, only about 30% of the imaging needs are covered by the existing budget.[16]
Tanzania
The major developments in training for rural imaging in Tanzania have partly been through foreign, private initiatives. The Kilimanjaro Christian Medical College (KCMC), which trains assistant medical officer (AMO) radiologists for rural Tanzania, is a private Faith-Based Medical University. Ultrasound training in Zanzibar and Pemba is also a private initiative. The foreign-driven rural training interventions in Tanzania and Pemba contrast with the local initiatives in Uganda. Local initiatives are more likely to be sustainable compared to the foreign ones, which sometimes result in overdependence.
Kenya, Rwanda, Sudan, Zambia, and Ghana
Training for rural imaging in these countries has been through government projects. Often, the training ceases or significantly ebbs at closure of the project. For training interventions of projects to be sustainable, they have to become institutionalized and locally owned.
The need for rural imaging in Sub-Saharan Africa
Approximately 500 / 1000 patients seen per year, in the rural health facilities in Uganda may require imaging, largely ultrasound and plain radiography.[8] The need for ultrasound and plain radiography in rural communities has been noted in other publications.[917–23]
Need for more sophisticated imaging like computed tomography (CT), magnetic resonance imaging (MRI) and radionuclide imaging is less.[1724]
Fifty-six percent of patients requiring imaging services in urban areas are imaged compared to 10–13% in rural areas.[8] Currently, up to 90% of the people living in rural Uganda, who would benefit from ultrasound are not scanned,[8] and it is estimated that 90% of the plain X-ray films from rural areas carry no imaging report. The situation may be similar in other SSA countries.
CHALLENGES OF HEALTH SERVICE PROVISION FOR RURAL COMMUNITIES
The challenges for RR in rural communities are very different from those in urban communities. These are related to human resource, and the socioeconomic, sociocultural, infrastructural, and academic disparities, albeit with a more complex disease spectrum and lower prioritization for imaging.
Human resource disparities
In general, there are proportionally higher numbers of health workers in the urban areas compared to rural areas.[25] Urban Zambia has 20 times more doctors and over five times more midwives and nurses than rural Zambia. In Malawi, where 87% of its people live in rural areas, 96.6% of the doctors are in urban areas. In Burkina Faso, there is one nurse to 4,000 patients in the urban area, compared to one nurse for 430,000 patients in the rural areas.[26] In Uganda, 73% of the country's doctors are urban and 46% of the country's doctors are in the capital city of Kampala.[12728] Thirty out of Uganda's 38 radiologists are in Kampala City and the rest are in major towns, with not even one in the rural area. Fifty percent of the total number of 180 radiographers are in Kampala City and 25% are in rural areas. Before the current interventions to boost the number of sonographers in rural areas, less than 5% of the countries’ 50 sonographers were in the rural areas. In Kenya, 80 (76%) out of the 105 radiologists are in three cities, and the rest in major towns. There are none outside the cities and towns. A very similar distribution was observed in Africa, almost 30 years ago,[29] and the same trend has also been observed in Australia.[30]
Socioeconomic and sociocultural disparities and differences in disease spectrum
There are inequalities in income in SSA between the urban and rural residents.[31] The inequalities between the rich and poor are far worse in these low income countries compared to developed countries. The Gini coefficients for low income countries in SSA are 0.4 – 0.5 compared to developed countries with 0.2 - 0.3.[31] The rural communities are largely agricultural-based, with hardly any industrialization or commerce. There are higher levels of non-employment, and less health-related benefits like health insurance, resulting in lower health-purchasing power, especially for more sophisticated health services like imaging. The families are comparatively larger, with overcrowding, resulting in a struggle for meagre home income. They are less exposed to hygiene and health education, and their level of schooling is lower. This spectrum of socioeconomic factors sets the stage for a disease of higher complexity. These factors may impact diseases, whose diagnosis requires imaging.
Poor transport and communication
Rural communities are disadvantaged by poor transport and telecommunication facilities, albeit the longer distances to the neighboring health facilities.[32] Transportation costs may be unaffordable resulting in delay or failure to access health services. The poor transport and communication also results in delays in accessing maintenance and service for imaging equipment. This may further be compounded by either lack of or unreliability of electricity supply, and unpredictable power surges. Imaging equipment, which depends on availability of internet for diagnosis of faults or software updates are also affected resulting in long downtimes.[8]
Academic isolation
Health workers residing in rural areas may find it more difficult to access continuing medical education (CME) seminars or other academic gatherings. They may not be aware of the opportunities due to absence or delays in communication, and if there are attendant financial requirements, these may be beyond their means. Fewer staff manning rural hospitals is a disadvantage for them, as it prevents them from taking study leave.[11] Long distances from training facilities further compound this.[33]
Prioritization of imaging, in comparison to other health interventions
The health priorities in rural areas, especially in SSA, are more focused on prevention of infectious diseases.[34] Consequently imaging may be less prioritized. This may explain the paucity of imaging equipment in rural areas. In addition, the imaging equipment is less sophisticated, older, and in poor functional state.[8] Prioritization also affects human resource. Higher priority disciplines like surgery, obstetrics, and pediatrics, usually have specialists in nearby larger hospitals, but not in radiology. Radiographers and sonographers are often fewer. The imaging units are often headed by radiographers, furthermore, in some remote areas, there are no radiographers, but just auxiliary staff, who have trained on the job.
TRAINING INTERVENTIONS FOR RURAL RADIOLOGY IN SUB-SAHARAN AFRICA
The interventions which will be described in this section are those that have specifically targeted RR. These do not include training at urban-based institutions, which do not have a specific agenda for rural health. This section will highlight interventions in eight SSA countries namely: Uganda, Kenya, Tanzania, Rwanda, Zambia, Malawi, Sudan, and Ghana.
Uganda
Training for RR in Uganda has focused on ultrasound and plain X-ray film interpretation. Prior to the training interventions in ultrasound, less than 5% of the sonographers were from rural areas. Through a joint effort by ECUREI, located in Kampala City, Mengo Hospital, and Jefferson Ultrasound Research and Education Institute (JUREI), of Thomas Jefferson University, Philadelphia- USA, Fontys / Meduprof-S from the Netherlands, and the governments of Uganda, up to 350 health workers have undergone ultrasound training to a diploma level. Fifty percent of these trainees are from rural Uganda, and these have included nurses, midwives, radiographers, assistant physicians, and a few doctors. Trainees have also come from other African countries: Tanzania, Kenya, Rwanda, Congo, Sudan, Ghana, and Zambia.[11]
A survey of the rural hospitals has shown that 76% of the graduates are still in their hospitals and practising ultrasound for two years after the training.
In addition, ECUREI has launched a one-year intensive course in plain X-ray film interpretation. Twenty health workers who include radiographers and assistant physicians have completed this course and five of them are from rural areas. ECUREI in partnership with Fontys / Meduprof-S have also launched an E-learning course in plain film interpretation, offered free of charge to those who may find it inconvenient or unaffordable to undertake the residential course, with the aim of reaching health workers in rural areas. ECUREI has embarked on training biomedical technologists specifically for imaging equipment, also targeting the maintenance of imaging equipment in the rural areas.
Kenya
The efforts began in 1996, as part of the first ORET project. (ORET stands for ‘Ontwikkelings Relevante Export Transacties’, which in English means Development Relevant Export Transactions). Ten courses, each lasting two weeks were conducted by the government of Kenya and the Netherlands, in partnership with the Fontys University, under this first ORET project. Currently, through a second ORET project, certificate courses in ultrasound are being conducted. The courses are in six modules, each lasting two weeks, and include ultrasound physics, anatomy, general abdominal, obstetrics, and gynecology ultrasound.[35] Plain film interpretation for non-radiologists has not yet been addressed, although it is estimated that 90% of the radiologists work in urban settings.
Moi University, located in a small town in Eastern Kenya, has recently launched a radiology residency program, targeting the rural areas.
Tanzania
Training for RR in Tanzania owes much of its success to Prof Helmut Diefenthal, a missionary doctor, at the KCMC, in rural Moshi. He launched a two-year course for training Assistant Medical Officers (AMOs), in imaging, with the aim of providing imaging services to the remote and under-served people of Tanzania. To date, up to 68 AMOs have been trained in this program, and 67 of these are deployed in different parts of rural Tanzania. Only one has left the country. In 1998, Prof Helmut launched a residency training program at KCMC, but of the 12 graduates from this program, only eight are in Tanzania, and of the eight, only one is working in rural Tanzania.
In 1997, the governments of Tanzania and the Netherlands, in partnership with Fontys / Meduprof-S, within the framework of the ORET project, conducted short ultrasound courses lasting two weeks, for 300 health workers (radiographers, nurses, and midwives) from 98 rural hospitals. The training also included refresher courses in radiography, train the trainers’ courses, and radiography curriculum development. Eighty-five of the participants were still active in their stations one year after completion of the courses.[35]
For Zanzibar and Pemba Islands, through the efforts of Dr. Franca Meloni from Italy, World Medical Colors, Ivo de Caneri Foundation, and the Mediterranean and African Society of Ultrasound (MASU), there is an ongoing program to train health workers in ultrasound through a modular course lasting five years. To date, up to 20 health workers residing in these islands have completed the course.[36]
Malawi, Ghana, and Zambia
Between 1996 and 2007, the national governments of Malawi, Ghana, and Zambia, and the government of the Netherlands, in partnership with the Fontys University (Meduprof-S, under various national ORET projects conducted short, two-to-six week ultrasound training programs, for radiographers, nurses, midwives, assistant physicians, and a few physicians.[35]
In Malawi, ten two-week long ultrasound courses and three refresher courses in radiography were held. In addition, a train the trainers’ course in ultrasound was also conducted and 75% of the Malawi trainees were still working in their hospitals one year after training.[35]
In Ghana, 10 ultrasound courses, three radiography refresher courses, plus one train the trainers’ course were held. Seventy-five percent of the trainees were still working in their hospitals one year after training.[35]
In Zambia, the activities under the ORET project included: Fifteen ultrasound courses for radiographers and midwives, 10 radiography refresher courses, curriculum review for the radiography school, and setting up a radiography and ultrasound skills laboratory. Eighty-five percent of the trainees were still working in their hospitals, one year after training.[35]
These short courses, although imparting only basic knowledge, raised the level of awareness for ultrasound and helped to attract and motivate participants to enrol for longer formal courses in ultrasound.
Rwanda
Efforts are still rudimentary. An ultrasound training curriculum has been developed and piloted.[37] There is also an ongoing program to train maintenance technicians.
Sudan
Through the efforts of Dr. Franca Meloni from Italy, World Medical Colors, Ivo de Caneri Foundation, and MASU, there is an ongoing program to train health workers in ultrasound through a modular course lasting five years, similar to the project in Zanzibar.[38]
Contributions by global, regional, and local professional societies
The World Federation of Ultrasound in Medicine and Biology (WFUMB) has facilitated ECUREI, to offer ultrasound courses. WFUMB has also run several short ultrasound workshops, in conjunction with the Mediterranean and African Society of Ultrasound (MASU) and various national ultrasound societies. Countries where WFUMB and MASU have been active are Uganda, Kenya, Tanzania, Sudan, Tunisia, Libya, and Morocco.
THE WAY FORWARD: RESPONSIBILITY OF THE STATE AND TRAINING INSTITUTIONS
Meeting the training needs of rural communities is largely the responsibility of the state, and not a primary mandate for academic institutions, but from a moral–ethical viewpoint, these institutions should actively engage in training for rural health.[183940] Professional societies and research institutions also have a moral obligation.
Teleradiology is increasingly being suggested as a solution for providing imaging services to underserved communities,[4142] but this may be too expensive for SSA.[43] Furthermore, tele-ultrasound, although promising, is still under investigation. Rural areas in Africa have poorer coverage of their imaging burdens and the health services are less efficient in comparison to urban areas. Training focussed on scaling up the numbers of human resource for imaging in these rural areas is key in increasing coverage and health-systems efficiency.[844]
CONCLUSIONS AND RECOMENDATIONS
There is a need to address imaging for rural SSA communities, who form over 80% of the population and whose imaging needs are largely ultrasound and plain film interpretation. The interventions so far have not adequately catered to these immense imaging needs. Meeting the imaging needs of rural communities is primarily the responsibility of the state. There is a need for a policy by governments in Africa toward RR. Training lower cadres or non-physicians for multitasking is one approach, but it has its disadvantages. Formal pre-service training targeted toward RR has to be explored and training institutions have a moral obligation to conduct this.
Source of Support: Nil
Conflict of Interest: None declared.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2012/2/1/37/97747
REFERENCES
- Republic Of Uganda. Uganda Demographic and Health Survey. The Republic of Uganda 2006 1 1
- [Google Scholar]
- High-Level-Forum-For-MDGs. In: Addressing Africa's Health Workforce Crisis: An Avenue for Action. 2004.
- [Google Scholar]
- Focused martenal ultrasound by midwives in rural Zambia. Ultrasound Med Biol. 2010;36:1267-72.
- [Google Scholar]
- Syrian women's perceptions and experiences of ultrasound screening in pregnancy: Implications for antenatal policy. Reprod Health Matters. 2005;13:147-54.
- [Google Scholar]
- Assessing the diagnostic Imaging needs for five selected hospitals in Uganda. J Clin Imaging Sci. 2011;1:53.
- [Google Scholar]
- A two-level ultrasonographic service in a maternity care unit of a rural district hospital in Tanzania. Trop Doct. 2008;38:125-6.
- [Google Scholar]
- Numbers of imaging personnel in African countries. Archives of African Society of Radiology (ASR) 2010
- [Google Scholar]
- Evaluation of US training for the past 6 years at ECUREI, the World Federation for Ultrasound in Medicine and Biology (WFUMB) Centre of Excellence, Kampala, Uganda. Acad Radiol. 2010;17:392-8.
- [Google Scholar]
- The new rural doctor: Qualified quack or appropriate healthcare provider? Indian J Med Ethics. 2010;7:2.
- [Google Scholar]
- Ministry Of Health Uganda. National Health Equipment Policy Document. Uganda: Ministry Of Health; 2005.
- [Google Scholar]
- Public Private Partnership for Health in Uganda: Will HSSP II Deliver on the Expections? Health Policy Dev J. 2010;5:48-56.
- [Google Scholar]
- Trends in Radiology and Imaging Service in the Tropics. London: Saunders Ltd; 2009.
- [Google Scholar]
- Feasibility of an ultrasound service on district health care in Botswana. Trop Med Int Health. 2001;6:1023-31.
- [Google Scholar]
- Ultrasonography as an aid to diagnosis and treatment in a rural African hospital: A prospective study of 1,119 cases. Am J Trop Med Hyg. 1999;60:119-23.
- [Google Scholar]
- Utility of portable ultrasound in a community in Ghana. J Ultrasound Med. 2008;27:1735-43.
- [Google Scholar]
- Introduction of a portable ultrasound unit into the health services of Lugufu refugee camp, Kigoma District, Tanzania. Int J Emerg Med. 2008;1:261-6.
- [Google Scholar]
- Rural and remote Australian general practitioners’ educational needs in radiology. J Contin Educ Health Prof. 2010;21:140-9.
- [Google Scholar]
- WHO. Future use of new imaging technologies in developing countries. Report of a WHO Scientific Group. World Health Organization Technical Report Series 723 1984:1-64.
- [Google Scholar]
- WHO. Increasing access to health workers in remote and rural areas through improved retention. Geneva: WHO; 2009.
- [Google Scholar]
- Health workers needed: poor left without care in Africa's rural areas. World Bank 2010 12 23
- [Google Scholar]
- Uganda 2002 Population and Housing census special analysis on health workers considered by the EU DHRH Project. 2005
- [Google Scholar]
- MInistry Of Health Uganda. Ministry of Health [Uganda] In: Human Resource Inventory. Uganda: Ministry of Health; 2004.
- [Google Scholar]
- Diagnostic radiology: Geography of a high technology. AJR Am J Roentgenol. 1979;132:339-44.
- [Google Scholar]
- Australian radiology workforce report. Workforce advisory Board, Royal Australian and New Zealand College of Radiologists. 2000
- [Google Scholar]
- Rural incomes, inequality and poverty dynamics in Kenya.Tegemeo Institute of Agricultural Policy and Development. Egerton University 2009 2010 12 16
- [Google Scholar]
- United-Nations. Policy issues for the Escap region: Balanced development of Urban and rural areas and regions within the Countries of Asia and the Pacific. In: United Nations Economic and Social Council. 2001.
- [Google Scholar]
- Challenges to rural medical education: A student perspective. Aust J Rural Health. 2002;10:168-72.
- [Google Scholar]
- Public Health in Africa: A report of the CSIS Global Health Policy Centre. Centre for Strategic and International Studies 2009
- [Google Scholar]
- Willem-Van-Proiijen. The Dutch approach to healthcare development aid. Medu Prof-S 2010
- [Google Scholar]
- Sonographic Training Program at a District Hospital in a Developing Country: Work in Progress. AJR Am J Roentgenol. 2010;189:119-22.
- [Google Scholar]
- Development of an ultrasound training curriculum in a limited resource international setting: Successes and challenges of ultrasound training in rural Rwanda. Int J Emerg Med. 2008;1:193-6.
- [Google Scholar]
- WFUMB. Report from Mediterranean and African Society of Ultrasound, MASU. ECHOES 12, 8 2008
- [Google Scholar]
- Accounting to society: Radiologic concern to patient care. AJR Am J Roentgenol. 1978;130:221-2.
- [Google Scholar]
- The impact of new imaging technology on worldwide health care, research, and teaching: Fifth international symposium. AJR Am J Roentgenol. 1992;160:195-201.
- [Google Scholar]
- The changing face of radiology: From local practice to global network. Med J Aust. 2009;190:20-3.
- [Google Scholar]
- Rural Radiology: Who is Producing Images and Who is Reading Them? J Rural Health. 2010;13:136-44.
- [Google Scholar]
- Radiology services for remote communities: Cost minimisation study of telemedicine. BMJ. 1996;312:1333.
- [Google Scholar]
- Assessing the performance of imaging health systems in five selected hospitals in Uganda. J Clin Imaging Sci. 2012;2:12.
- [Google Scholar]






