Translate this page into:
Sonographic Appearance of the Median Nerve Following Revision Carpal Tunnel Surgery
-
Received: ,
Accepted: ,
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
The main objective of this pictorial essay is to illustrate the sonographic appearance of the postoperative carpal tunnel and median nerve. Carpal tunnel surgical treatment failures have been shown to occur in up to 19% of a large series requiring re-exploration. Surgical management options for recurrent carpal tunnel syndrome (CTS) include revision release, neurolysis, vein wrapping, and fat grafting procedures. While several descriptions of median nerve entrapment in CTS exist in the ultrasound literature, little is written regarding its postoperative appearance. We report the sonographic changes in the appearance of the median nerve and postoperative carpal tunnel.
Keywords
Carpal tunnel
orthopedic surgery
ultrasound
median nerve
INTRODUCTION

Carpal tunnel syndrome (CTS) is the most common compression neuropathy,[12] affecting 10% of the general population[3] and 3% of adults 40–60 years of age.[4] Along with clinical impressions, the gold standard for diagnosing CTS is electromyogram (EMG). In recent years, ultrasound has emerged as both a diagnostic tool and an aid for treatment.[567] First-line treatment consists of conservative medical management including night splints, nonsteroidal inflammatory drugs, and corticosteroid injections.[2] However, despite good conservative management, symptoms may sometimes persist, and carpal tunnel release is the definitive management.[2]
Carpal tunnel release is a highly successful procedure, with success rates of up to 100% in some series.[8] However, treatment failures have been shown to occur in up to 19% of a large series, requiring re-exploration in as many as 12% for various reasons.[910] In many cases of failed carpal tunnel release, perineural fibrosis is the cause.[10] Surgical management options for such cases include exploration and revision release, neurolysis, vein wrapping, and fat grafting procedures.[3910] Revision carpal tunnel surgery may be less successful than the primary procedure, and EMG studies are unreliable postoperatively.[7]
Ultrasound has been documented as a useful tool for diagnosing enlargement of the median nerve in CTS and can have similar utility in imaging or following the postoperative median nerve appearance.[7] While several descriptions of median nerve entrapment and contents of the carpal tunnel exist in the ultrasound literature, little is written regarding its postoperative appearance and even less on its postrevision appearance. It is of value to consider the varying sonographic changes in the appearance of the postoperative carpal tunnel and median nerve.
Normal and abnormal appearance of median nerve
The normal median nerve seen by ultrasound and an enlarged median nerve in a patient with CTS are shown in Figures 1 and 2. When imaged transversely via ultrasound, the normal median nerve at the entrance of the carpal tunnel appears as a round or oval honeycomb structure positioned just deep to the transverse carpal ligament, and superficial to the flexor digitorum tendons. The cross-sectional area of the median nerve in asymptomatic volunteers averages 9 mm2.[5] In patients with CTS, the nerve appears swollen and enlarged with cross-sectional surface area measurements of >10 mm2 demonstrating high sensitivity and specificity for clinical CTS symptoms.
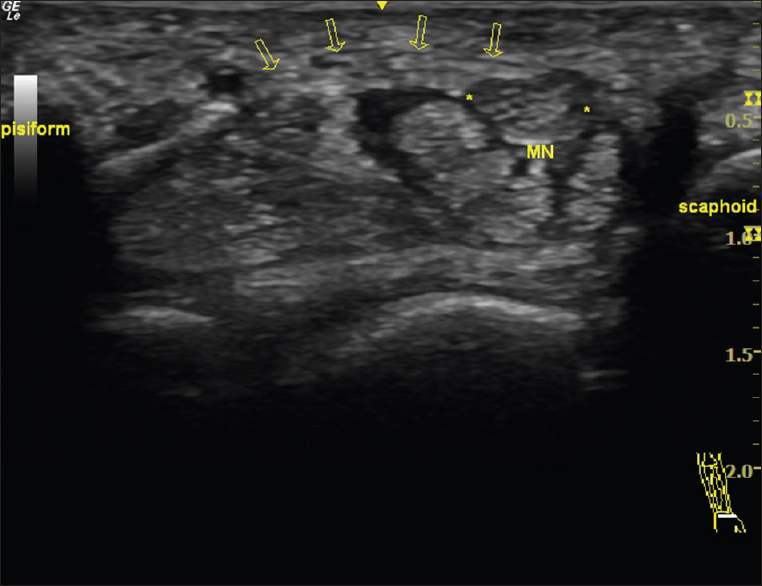
- Transverse view of a left wrist carpal tunnel in a 30-year-old female without carpal tunnel syndrome shows normal size and appearance of the median nerve (asterisks) as well as intact transverse carpal ligament (arrows).
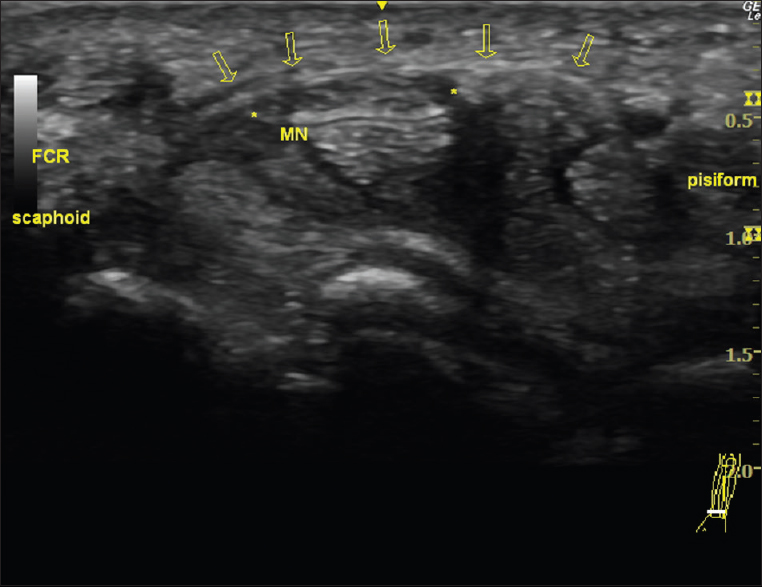
- Transverse view of a right wrist ultrasound in a 41-year-old male patient with carpal tunnel syndrome shows markedly enlarged median nerve (asterisks) and intact transverse carpal ligament (arrows). FCR: Flexor carpi radialis.
Surgical procedures for carpal tunnel syndrome treatment
Carpal tunnel release is performed as an open or endoscopic surgery that transects the transverse carpal ligament to relieve pressure on the median nerve. Figure 3 shows the sonographic appearance of the carpal tunnel and median nerve after carpal tunnel release surgery, and Figure 4 shows magnetic resonance imaging (MRI) correlation. In both images postoperatively, the median nerve is found to be enlarged. The ultrasound appearance of the transverse carpal ligament is absent, whereas on MRI, the ligament is seen as a dark fibrous band transected just superficial to an enlarged median nerve.
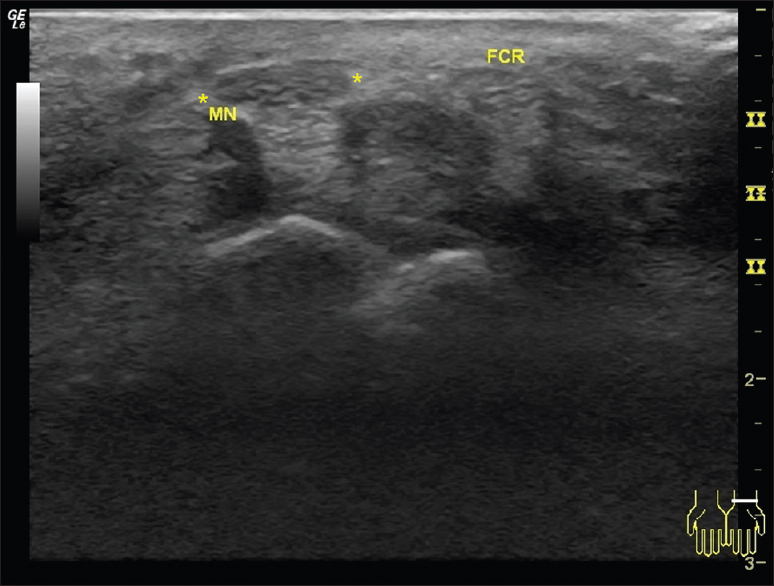
- 55-year-old female with recurrent pain and paresthesias of the left wrist and hand after carpal tunnel release surgery. Postoperative ultrasound of the carpal tunnel demonstrates an enlarged median nerve (asterisks) with transection (absence) of the transverse carpal ligament. FCR: Flexor carpi radialis.
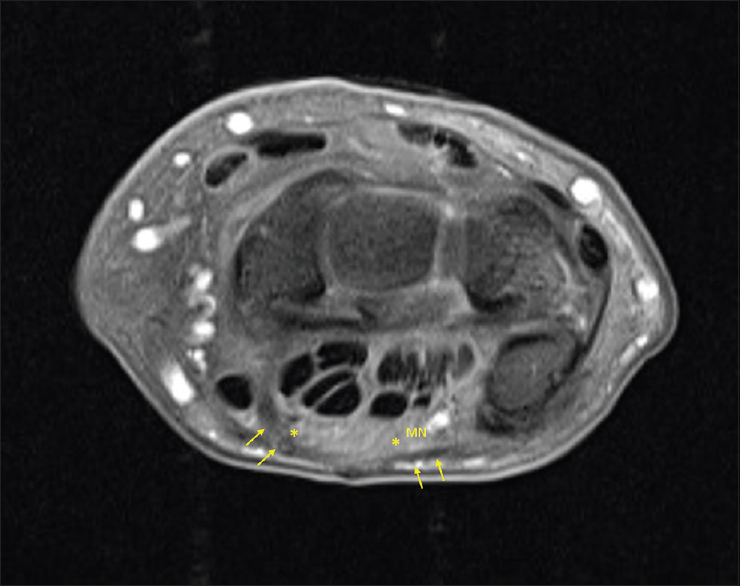
- Right wrist magnetic resonance imaging correlation in a 57-year-old female who previously underwent carpal tunnel release. Axial spin echo T1-weighted image with fat saturation shows enlarged median nerve (asterisks) and transverse carpal ligament (arrows). The ligament is visibly transected in the image superficial to the median nerve.
Post-surgical revision appearance of median nerve
Failure of carpal tunnel release surgery may be due to scarring and perineural fibrosis. Median nerve gliding may be improved in revision carpal tunnel release surgery by treating perineural fibrosis and protecting the nerve from further scarring by wrapping the nerve in an autologous vein as shown sonographically in Figure 5 and graphically illustrated in Figure 6. Another option for protecting the median nerve from scarring after surgical re-exploration harvests fat from the ipsilateral hypothenar fat pad to be placed between the nerve and any residual fibers of the transverse carpal ligament. The resulting appearance of the carpal tunnel, median nerve, and fat graft is shown sonographically in Figure 7.
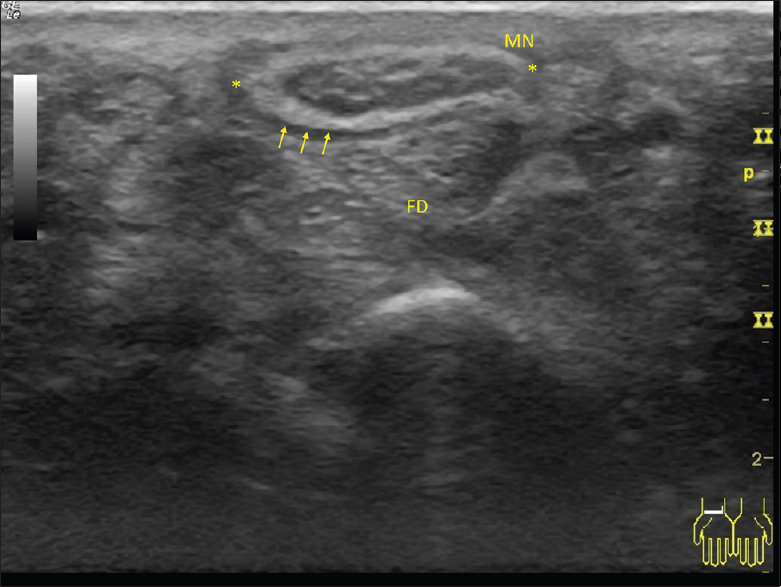
- 57-year-old female with recurrent right wrist carpal tunnel syndrome symptoms underwent revision surgery. Sonographic appearance of the transverse carpal tunnel after revision carpal tunnel release, and ipsilateral leg saphenous vein wrap to the median nerve (asterisks, MN) shows the increased hyperechoic appearance of the vein wrap (arrows) surrounding the nerve and absence of the transverse carpal ligament. FD: Flexor digitorum tendons in transverse view.
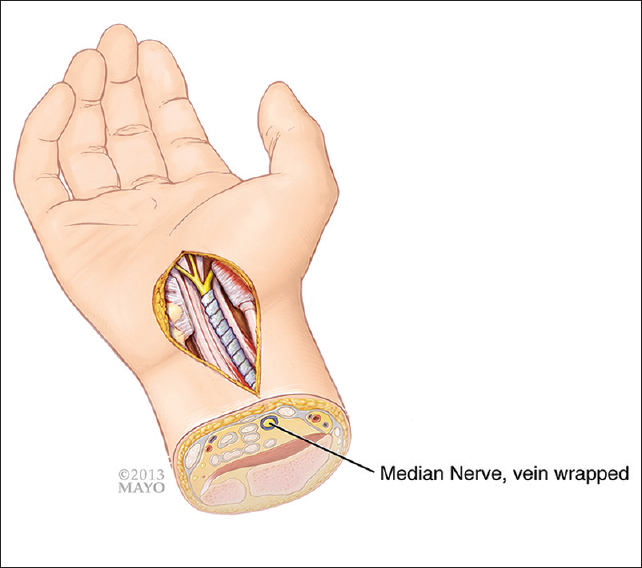
- Illustration shows the vein-wrapping procedure. By permission of Mayo Foundation for Medical Education and Research. All rights reserved
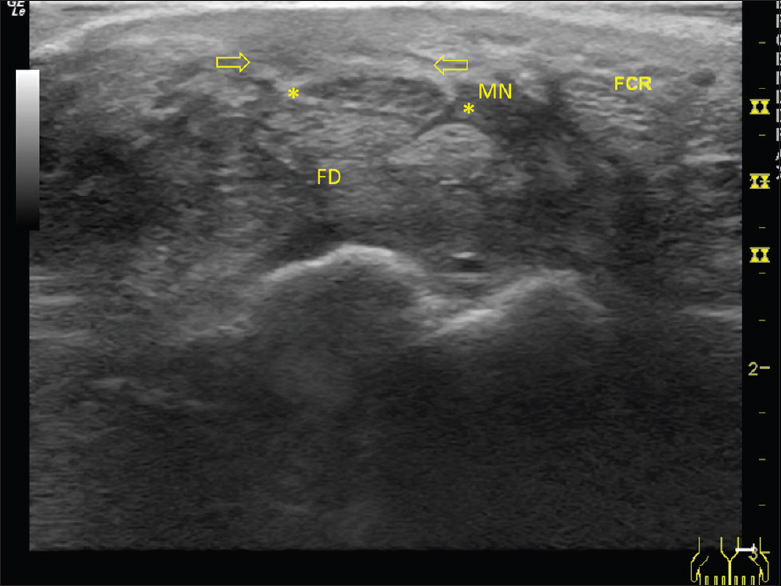
- A 74-year-old male with recurrent carpal tunnel syndrome who underwent revision surgery of the left wrist. Sonographic appearance of revision carpal tunnel release and fat graft with absent transverse carpal ligament and increased adipose tissue from fat graft (open arrows) superficial to the median nerve (asterisks) and carpal tunnel. FD: Flexor digitorum and FCR: Flexor carpi radialis tendon
CONCLUSION
Recurrent carpal tunnel syndrome remains a problem for a small percentage of patients even after carpal tunnel release surgery. To gain better insight, we demonstrate the sonographic changes of the median nerve within the carpal tunnel in several postoperative scenarios. These sonographic images may help further guide clinicians’ understanding of anatomical changes within the carpal tunnel related to such surgical techniques.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2016/6/1/11/179419
REFERENCES
- Prevalence of carpal tunnel syndrome in a general population. JAMA. 1999;282:153-8.
- [Google Scholar]
- Carpal tunnel syndrome-try these diagnostic maneuvers. J Fam Pract. 2012;61:726-32.
- [Google Scholar]
- Autogenous vein wrapping for treatment of recurrent carpal tunnel syndrome. Egypt J Plast Reconstr Surg. 2010;34:173-80.
- [Google Scholar]
- Prevalence of work-related dermatitis in the working population: Authors’ response to letter from Rosenman and Fussman. Am J Ind Med. 2014;57:127-8.
- [Google Scholar]
- The use of diagnostic ultrasound in carpal tunnel syndrome. J Hand Surg Am. 2006;31:726-32.
- [Google Scholar]
- Diagnostic utility of ultrasonography versus nerve conduction studies in mild carpal tunnel syndrome. Arthritis Rheum. 2008;59:357-66.
- [Google Scholar]
- High definition ultrasound as diagnostic adjunct for incomplete carpal tunnel release. Hand Surg. 2011;16:289-94.
- [Google Scholar]
- Treatment of recurrence of the carpal tunnel syndrome. Ann Chir Main. 1987;6:203-9.
- [Google Scholar]
- Surgical options for recalcitrant carpal tunnel syndrome with perineural fibrosis. Hand (N Y). 2012;7:23-9.
- [Google Scholar]






