Translate this page into:
Silicone-induced Penile Sclerosing Lipogranuloma: Magnetic Resonance Imaging Findings
-
Received: ,
Accepted: ,
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Sclerosing lipogranuloma is a rare benign disease, representing a peculiar granulomatous reaction of fatty tissue. The majority of cases are secondary to injection of exogenous foreign bodies, such as silicone, paraffin, mineral, or vegetable oils. To the best of our knowledge, we present the first case of a silicone-induced penile lipogranuloma in a 52-year-old man evaluated with a multiparametric magnetic resonance imaging (MRI) protocol, including diffusion-weighted imaging, magnetization transfer imaging, and dynamic contrast-enhanced MRI. MRI of the penis by combining both conventional and functional information represents an important imaging tool in the preoperative workup of silicone-induced penile lipogranuloma.
Keywords
Diffusion-weighted magnetic resonance imaging
magnetic resonance imaging
penis
sclerosing lipogranuloma
silicone

INTRODUCTION
Penile sclerosing lipogranuloma is a rare mass of the male genitalia.[1234] The disease is divided into primary and secondary types. The primary type is caused by the breakdown of endogenous lipids and the secondary type by injection of exogenous foreign bodies.[1234] Foreign materials, including silicone, paraffin, mineral oil, metallic mercury, petroleum jelly, vaseline, and cod liver oil have been used to provide an improvement in penile shaft contour and dimensions.[567] Arthaud et al., reported the first case of liquid silicone injected to the penis in 1973, on one subject who had an injection of silicone from a nonprofessional person.[5] Liquid injectable silicone for penile augmentation may have debilitating effects, requiring surgical intervention to correct complications.[567]
Although sonography represents the primary modality for cross-sectional imaging of the penis, magnetic resonance imaging (MRI) may provide important diagnostic information in the investigation of penile pathology, especially in cases of inconclusive or nondiagnostic sonographic findings.[8] Recently, functional MRI, including diffusion-weighted imaging (DWI), magnetization transfer imaging (MTI), and dynamic contrast-enhanced (DCE) MRI have been used in the interpretation of scrotal diseases.[910] To our knowledge, no reports regarding these techniques in the evaluation of penile diseases exist in the English literature. Herein, we present the MRI findings of a silicone-induced penile lipogranuloma. A multiparametric MRI protocol was used, including DWI, MTI, and DCE-MRI.
CASE REPORT
A 52-year-old man was referred to the Urology Department with significant enlargement of the penis and sexual dysfunction of 1-year duration. The patient reported a history of subcutaneous injection of liquid silicone in the penis by a nonmedical practitioner, 10 years ago. Clinical examination revealed large, painless enlargement of the penile shaft due to the presence of a hard mass invading the skin and the subcutaneous tissues, but not the corpora cavernosae. Migration of particles of the mass to the scrotum was also observed. Laboratory examination showed normal findings.
MRI examination was done on a 1.5-T system, with the penis in the flaccid state. The MR protocol included axial spin-echo T1-weighted sequences, fast spin-echo T2-weighted sequences in the three orthogonal planes and transverse DW sequences with b-values of 0 and 900 s/mm−2. MTI was followed in the same plane. Magnetization transfer ratio (MTR) was calculated from the following equation:
SIo − SIm/SIo × 100%
Where, SIm and SIo refer to signal intensities with and without the saturation pulse, respectively. After a rapid injection of gadopentetate dimeglumine, sagittal DCE subtraction MRIs were also obtained.
A heterogeneous, ill-defined mass involving the subcutaneous tissues around the penis and extending into the intertesticular and retrotesticular region were detected [Figure 1]. The lesion was asymmetrically Y-shaped with the arms of Y around corpora carvenosae, slightly hyperintense, and extremely hypointense on T1- and T2-weighted images [Figure 1a], respectively when compared to the penile shaft. No fatty components were revealed within the mass. Lesion heterogeneity was seen on the apparent diffusion coefficient (ADC) maps. The mean ADC was 1.53 × 10−3 mm2/s [Figure 1b], similar to that of corpora carvenosae and suggestive of benignity. MTIs showed the very low signal intensity of the mass, with a mean MTR of 67%, suggestive of the presence of macromolecules [Figure 1c and d]. On dynamic imaging, the lesion enhanced strongly and heterogeneously, with an initial upstroke, followed by gradual increase of enhancement in late postcontrast phase [Figure 1e]. Both the corpora cavernosae and the corpus spongiosum were normal, with intact tunica albuginea. The spermatic cords, the epididymis, and the testes were not involved. Based on MRI findings and the clinical history, the diagnosis of silicone-induced penile lipogranuloma was strongly suggested, and the patient was referred for surgical excision of the lesion.
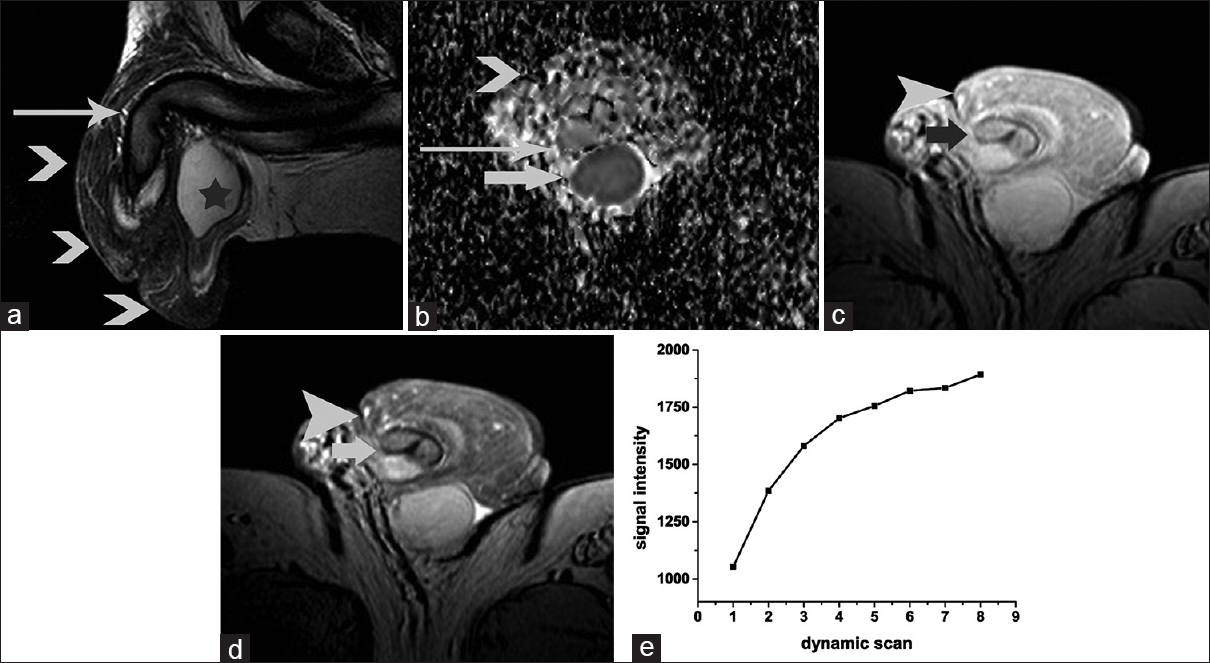
- 52-year-old man with silicone-induced penile sclerosing lipogranuloma. (a) Sagittal T2-weighted image of the penis demonstrates heterogeneous lesion, with ill-defined margins surrounding the penis. The mass (arrowheads) was mainly of low signal intensity on T2-weighted images, a finding suggestive of the presence of fibrous tissue. Corpora cavernosa are intact (long arrow). Image shows normal right testis (asterisk). (b) Transverse apparent diffusion coefficient map (b = 900 mm2/s) shows heterogeneous mass (arrow) surrounding the penile shaft. The lesion appears mainly isointense when compared to the normal corpora cavernosa (long arrow). The apparent diffusion coefficient value of the mass was 1.53 × 10−3 mm2/s (right corpus cavernosum: 1.49 × 10−3 mm2/s; left corpus cavernosum: 1.60 × 10−3 mm2/s). Normal left testis (arrow). Transverse three-dimensional gradient-echo images acquired (c) without and (d) with the application of the magnetization transfers pulse. The magnetization transfer signal of the mass lesion (arrowhead) was qualitatively lower than that of the corpora cavernosa (arrow). The magnetization transfer ratio (in percent) of the lesion was 67%. (e) Time-signal intensity curve of the lesion shows an initial upstroke after which the signal intensity gradually increases in the late contrast-enhanced phase.
During surgery the removal of approximately 80% of the mass was possible. The lesion was solid and white, invading the skin, the subcutaneous tissues, and the dartos muscle of the penis. The cut surface of the tissue was solid and whitish-yellow in color. Histopathological examination demonstrated vacuoles of variable size corresponding to exogeneous substance, embedded in collageneous stroma. Multinucleated giant cells were seen around the vacuoles and infiltrates of lymphocytes perivascularly. The diagnosis of sclerosing lipogranuloma was made on histology [Figure 2]. The patient had an uneventful recovery and was advised to return for follow-up 2 months after surgery.
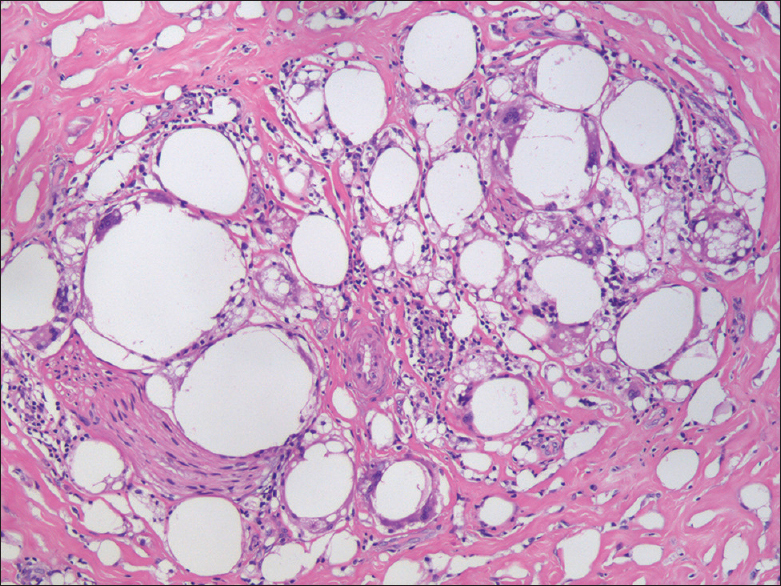
- 52-year-old man with silicone-induced penile sclerosing lipogranuloma. Histopathologic evaluation of the excised tissue reveals vacuoles of variable size in the dermis corresponding to exogeneous substance. Multinucleated giant cells and abundant fibrosis is seen around the vacuoles (Hematoxylin and Eosin stain, magnification ×20).
DISCUSSION
Penile sclerosing lipogranuloma is a granulomatous reaction that occurs after injury of the adipose tissue. The secondary type of the disease is caused by foreign body injections directly into the penis, such as silicone, paraffin oil, paraffin balm, and mineral oils.[1234567] Secondary penile sclerosing lipogranuloma usually requires an aggressive treatment including partial or total excision of granulomas, with or without reconstructive skin flaps depending on the extent of excision.[567] An imaging technique accurately characterizing and assessing the extent of the disease would be valuable in the appropriate preoperative planning of these patients.
MRI is now increasingly used as either a problem-solving tool in cases of indeterminate sonographic findings or as a primary imaging modality in the evaluation of penile diseases.[8] Specifically, MRI has been proved useful in the differentiation between benign and malignant penile lesions and in defining the extent of inflammatory processes and traumatic injuries. It is also considered the most accurate imaging technique in the assessment of primary penile carcinomas.[8]
Motoori et al., described the MRI findings of a primary scrlerosing lipogranuloma of the male genitalia in a 55-year-old man.[4] The lesion was symmetrically Y-shaped, with the arms of the Y surrounding the penile shaft. The mass showed similar and moderately high signal intensity when compared to muscles on T1- and T2-weighted images, respectively, with irregular enhancement after gadolinium administration.[4] Small areas within the lesion, hyperintense on T2-weighted sequences, without contrast enhancement, suggested the presence of cystic or necrotic parts.[4] The MRI features of the same entity were reported also by Nishizawa et al.[3] The mass demonstrated an ill-defined symmetrical Y-shape, situated just beneath the corpus spongiosum with the arms of the Y around the penile shaft. The lesion was mainly isointense on T1-weighted images, strongly enhancing, with low signal intensity on T2-weighted images, the latter related to the presence of fibrous tissue.[3]
An asymmetrically Y-shaped mass surrounding the carvenosal bodies and extending into the scrotum was revealed in our patient. The lesion was slightly hyperintense on T1-weighted images and predominantly hypointense on T2-weighted images. The hypointensity of the mass on T2-weighted sequences was suggestive of the presence of fibrous tissue, as subsequently proved on pathology and it is considered an important diagnostic feature in differentiating this entity from malignancy.
Lesion detection and characterization on DWI is mainly dependent on the extent of tissue cellularity, and increased cellularity is associated with restricted diffusion and reduced ADC.[9] The ADC values of malignancies are usually lower than those of benign lesions or normal tissues.[9] In this case, no areas of restricted diffusion were identified within the mass, and the ADC was similar to that of normal corpora cavernosae, findings strongly suggestive of benignity.
MTI sequences offer a different image contrast compared to T1- and T2-weighted images.[10] In conventional MRIs, tissue contrast depends mainly on the presence of free protons, whereas, on MTIs, the signal is determined by the restricted macromolecular protons.[10] The MT phenomenon is quantified by the MTR. Tissues containing macromolecules, a classical example is fibrous tissue, transfer magnetization more efficiently detected as hypointense on MTIs, with high MTR, as in this patient.
DCE-MRI evaluates the kinetics of the distribution of the paramagnetic contrast medium in the micro-vessels and the interstitial spaces of the tissues used. The technique may provide useful information in lesion characterization.[9] Malignancies usually present with the rapid uptake of the contrast medium, followed by washout in the delayed phase, whereas benign lesions often enhance strongly and rapidly, followed by either a plateau or gradual increase of enhancement in the late post-contrast phase.[9] Although, there are no reports on the DCE-MRI characteristics of penile lesions in the English literature, penile lipogranuloma in this case enhanced intensely, followed by a gradual increase of enhancement in the late post-contrast phase, findings that could suggest the benign nature of the lesion.
CONCLUSION
MRI examination using both morphologic and functional data provided valuable information in the preoperative planning in our case, by estimating the precise extent of the mass and helping in the characterization of the benign nature of disease.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Acknowledgments
The authors would like to thank Eleni Papakonstantinou from Department of Histopathology, Thriassion General Hospital, Athens, Greece, for the valuable help in the interpretation of the histologic data.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2016/6/1/3/175084
REFERENCES
- Primary sclerosing lipogranuloma of the rectum: CT findings. Br J Radiol. 2006;79:e190-2.
- [Google Scholar]
- Sclerosing lipogranuloma of the scrotum: Sonographic findings and pathologic correlation. J Ultrasound Med. 2007;26:1231-3.
- [Google Scholar]
- Magnetic resonance imaging of sclerosing lipogranuloma of male genitalia. J Urol. 2002;168(4 Pt 1):1500-1.
- [Google Scholar]
- Sclerosing lipogranuloma of male genitalia: CT and MR images. J Comput Assist Tomogr. 2002;26:138-40.
- [Google Scholar]
- Low-grade liquid silicone injections as a penile enhancement procedure: Is bigger better? Urol Ann. 2012;4:181-6.
- [Google Scholar]
- Penile injection with silicone: Case report and review of the literature. J Sex Med. 2008;5:2231-7.
- [Google Scholar]
- Magnetization transfer imaging of normal and abnormal testis: Preliminary results. Eur Radiol 2015 [Epub online 12 Jun, 2015, ahead of print]
- [Google Scholar]






