Translate this page into:
Perirenal PEComa: Computed Tomography Findings and Differential Diagnosis
Address for correspondence: Prof. Athina C Tsili, Department of Clinical Radiology, Medical School, University of Ioannina, 45110 Ioannina, Greece. E-mail: a_tsili@yahoo.gr
-
Received: ,
Accepted: ,
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
The World Health Organization defines perivascular epithelioid cell tumors (PEComas) as mesenchymal tumors and tumor-like conditions composed of epithelioid cells with a perivascular distribution. These tumors may show benign or malignant histology and/or biological behavior. However, the pathological features of malignancy may not correlate with biologic aggressiveness, and the criteria for malignancy are not clearly defined. Abdominopelvic PEComas are very rare and have been reported in various locations, including kidney, liver, pancreas, gastrointestinal tract, genitourinary tract, peritoneum, and retroperitoneum. Cross-sectional imaging techniques, including computed tomography (CT) may play an important role in the accurate detection and characterization of these tumors. We present the third case of an extremely rare PEComa with perirenal location, discuss CT findings and differential diagnosis.
Keywords
Computed tomography
differential diagnosis
PEComa
perirenal
perivascular epithelioid cell tumors

INTRODUCTION
Perivascular epithelioid cell tumors (PEComas) are a rare group of mesenchymal neoplasms composed of distinctive cells which show a focal association with the walls of blood vessels and usually express melanocytic and smooth-muscle markers.[12345] These tumors include renal angiomyolipoma, lymphangioleiomyomatosis, clear cell sugar tumor of the lung, and similar neoplasms occurring in the retroperitoneum, kidney, uterus, pancreas, or other visceral and soft-tissue sites.[123] Imaging findings of these tumors are usually nonspecific.[345]
To our knowledge, in the English literature, there are only two publications referring to PEComas with perirenal manifestation with no report on computed tomography (CT) findings.[67]
CASE REPORT
We examined the case of a 44-year-old woman who presented with left lumbar pain of 4 months duration. The patient had no history of cancer or infectious disease. No clinical evidence of tuberous sclerosis was present. Physical examination was uremarkable. Laboratory analysis showed normal findings, except for the presence of mild neutrophil leukocytosis. Sonography revealed the presence of a large, heterogenous, well-margined mass, located in the left perirenal space [Figure 1a]. The lesion was partly cystic solid, with solid components detected with moderate vascularity at Doppler examination [Figure 1b]. A multidetector computed tomography scan was followed on a 16-row scanner. The presence of a large, inhomogeneous left perirenal mass [Figure 2a], in close proximity to the renal capsule was confirmed. The dimensions of the lesion were 6 cm × 7 cm × 10 cm, approximately. The tumor had cystic parts, with CT density similar to that of water, not enhancing after intravenous contrast medium administration, and solid parts, with strong, heterogeneous enhancement [Figure 2b]. Nonenhancing areas within the solid components were attributed to the presence of necrosis. Neither areas of macroscopic fat nor foci of calcification were detected within the lesion. Peritumoral vascularity, seen as asymmetrically increased vessels adjacent to the mass within Gerota fascia, was also identified [Figure 2c]. Mass effect to the surrounding organs was noted, particularly to the left kidney, without obvious findings of invasion. Neither signs of metastatic lymphadenopathy nor distant metastases were seen.
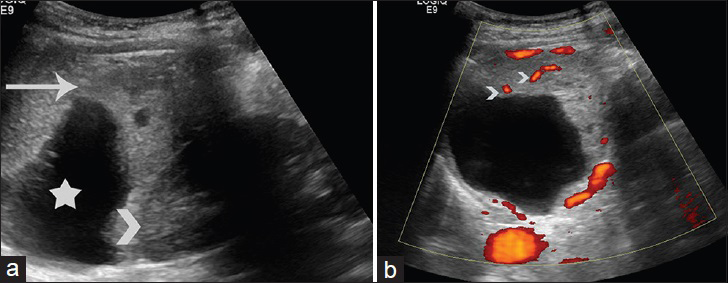
- 44-year-old woman with 4-month history of lumbar pain diagnosed with perivascular epithelioid cell tumor. (a) Sagittal sonographic image of the left hypochondrium depicts the presence of a large heterogenous left perirenal mass. The lesion has cystic parts (asterisk) and solid, heterogeneous components (long arrow). The mass is in close proximity to the ipsilateral kidney (arrowhead). (b) Sagittal power Doppler image of the left perirenal mass reveals vascularity of the solid parts (arrowheads).
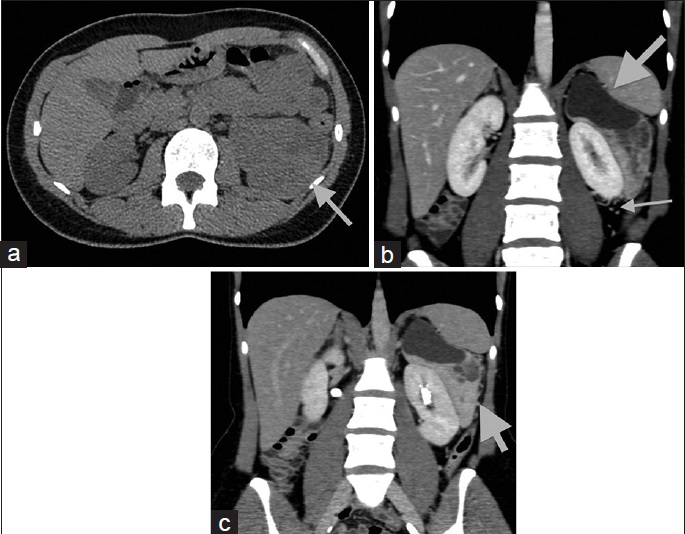
- 44-year-old woman with 4-month history of lumbar pain diagnosed with perivascular epithelioid cell tumor. (a) Transverse noncontrast computed tomography image demonstrates inhomogeneous solid parts of the lesion (arrow). The mean computed tomography density of the solid components is 35 HU on unenhanced images, similar to that of normal renal parenchyma. Coronal reformations during (b) the portal phase and (c) the excretory phase depict sharply demarcated left perinephric mass (arrow), partly cystic and solid, in close proximity to the renal capsule. The solid parts of the tumor enhance intensely and heterogeneously, with a mean portal phase attenuation of 100 HU. The left renal parenchyma is intact. Prominent vessels are seen in the left perirenal space adjacent to the lesion (long arrow).
Intraoperatively, the mass was separated from the renal capsule by a thin layer of fibrous tissue and tumorectomy was performed. Histologically, the neoplasm was composed of spindle and epithelioid cells, immunoreactive for vimentin, desmin, smooth muscle actin, HMB45, CD56, CD99, B cell lymphoma-2, ER, NSE, and focally for MART-1 and CD31. Mitoses were rare (<1/50 HPF). Cellularity was moderate, without nuclear atypia. Areas of myxoid, partly cystic degeneration and areas of hemorrhage were identified within the tumor. Pathology showed absence of fat and calcifications within the tumor. The mass was surrounded by fibrous tissue, without signs of renal invasion. Overall, the findings were consistent with the diagnosis of PEComa of uncertain malignant potential. Resection margins were tumor-free. The patient had an uneventful recovery and was advised to return for follow-up, 3 months after the operation.
DISCUSSION
The category “PEComa” was first suggested in 1992 by Bonetti and includes neoplasm primarily composed of HMB-45-positive epithelioid cells with a perivascular distribution.[123] An association with the tuberous sclerosis complex has been reported. These tumors are often benign and curable after surgical resection. However, a minority shows aggressive behavior, with local recurrence and/or distant metastases, more often in lungs, liver, and peritoneum.[1234567] Malignant PEComas have been reported to be associated with two or more of the following risk factors: Size >5 cm, high nuclear grade and cellularity, mitotic rate >1 mitosis/HPF, and presence of necrosis or vascular invasion.[1234567] Long-term surveillance is strongly recommended in these patients.[1234567]
Imaging features of PEComas are often nondiagnostic. Tan et al. in a retrospective analysis of 32 PEComas reported a mean tumor diameter of 5.1 cm, well-defined margins, hypodensity on CT, low and high signal intensity on T1- and T2-weighted magnetic resonance imaging (MRI) images, respectively, and strong, heterogeneous enhancement.[4] Tirumani et al., in a retrospective study of 36 malignant PEComas reported large, well-circumscribed masses, heterogeneous on sonography, with CT density and signal intensity on T1-weighted images similar to that of skeletal muscles, heterogeneity on T2-weighted images and inhomogeneous enhancement.[5]
Approximately, 100 cases of PEComas have been reported up to date in the literature, most commonly involving the genitourinary tract, two of them with perirenal location.[67] Di Blasi et al. reported a case of renal capsuloma observed as an incidental finding, coexisting with a papillary transitional cell carcinoma of the pelvicaliceal system.[6] The second case of perirenal PEComa was reported on a 57-year-old woman by Gunia et al.[7] The authors described the MRI findings of this entity, as a predominantly solid mass, with occasional cystic changes. The tumor was mainly hypointense on T1 and fat-suppressed T2-weighted images, when compared to normal renal parenchyma, with delayed contrast enhancement.[7]
The CT findings of PEComa with perirenal manifestation have never been reported in the English literature. In our patient, a well-defined, inhomogeneous perirenal mass was detected, with cystic parts and solid components, the latter heterogeneously enhancing after contrast material administration. Abnormal vessels adjacent to the neoplasm were detected in the perirenal space. A variety of neoplastic and proliferative disorders may affect the perirenal space, with a wide array of cross-sectional imaging findings.[89] In cases of solitary partly cystic-solid masses of the perirenal space, differential diagnosis should include the following: Leiomyoma, hemangiopericytoma, malignant fibrous histiocytoma, hemangioma and more rarely leukemia, primary extragastrointestinal stromal tumor, and Castleman's disease.[8]
Perirenal leiomyoma represents a rare benign mesenchymal neoplasm, arising from the renal capsule and extending into the perirenal space.[810] Imaging findings include a well-demarcated soft-tissue mass that is supplied by renal capsular vessels. Large leiomyomas are usually heterogeneous, due to the presence of hemorrhage and/or cystic myxoid degeneration.[810] Hemangiopericytoma represents a rare retroperitoneal soft tissue neoplasm, more often detected as large, lobulated, well-defined, hypervascular soft tissue mass with areas of calcification and necrosis.[8] Malignant fibrous histiocytoma is seen in the retroperitoneum in approximately 15% of cases. It is usually detected as a large heterogeneous mass, displacing the kidney, with areas of necrosis and hemorrhage. The presence of calcifications is reported in 7–20% of cases.[8] Perirenal hemangioma is an extremely rare benign mesenchymal renal tumor, with nonspecific imaging features. However, the depiction of a soft tissue mass with phleboliths, hyperintensity on T2-weighted MRI images, and delayed or persistent enhancement are considered as suggestive of the diagnosis.[8] Isolated leukemic involvement and primary extragastrointestinal stromal tumor with perirenal location are extremely rare, with nonspecific imaging findings.[8] Isolated perirenal lesions in Castelman disease are also rare, detected as homogeneous soft tissue masses, with well-defined margins.[8]
CONCLUSION
The preoperative diagnosis of PEComa with perirenal manifestation based on CT findings is difficult. However, in the presence of a large, well-defined perirenal mass, partly cystic-solid, with solid components enhancing after contrast material administration, accompanied by peritumoral vessels, this rare entity should be included in the differential diagnosis.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2015/5/1/69/172977
REFERENCES
- Neoplasms with perivascular epithelioid cell differentiation (PEComas) In: Fletcher CD, Unni KK, Mertens F, eds. World Health Organization classification of tumors. Pathology and genetics of tumors of soft tissue and bone. Lyon: IARC Press; 2002. p. :221-2.
- [Google Scholar]
- Neoplasms of the perivascular epithelioid cell involving the abdomen and the pelvis: Cross-sectional imaging findings. J Comput Assist Tomogr. 2007;31:688-96.
- [Google Scholar]
- Perivascular epithelioid cell tumour: Dynamic CT, MRI and clinicopathological characteristics – analysis of 32 cases and review of the literature. Clin Radiol. 2013;68:555-61.
- [Google Scholar]
- Imaging features of primary and metastatic malignant perivascular epithelioid cell tumors. AJR Am J Roentgenol. 2014;202:252-8.
- [Google Scholar]
- Renal capsuloma: Description of a case with predominantly muscular differentiation. Pathologica. 2003;95:119-22.
- [Google Scholar]
- Perivascular epithelioid cell tumor (PEComa) with perirenal manifestation. Int J Urol. 2005;12:489-92.
- [Google Scholar]
- Neoplastic and non-neoplastic proliferative disorders of the perirenal space: Cross-sectional imaging findings. Radiographics. 2008;28:1005-17.
- [Google Scholar]
- Neoplastic and proliferative disorders of the perinephric space. Clin Radiol. 2012;67:e31-41.
- [Google Scholar]
- Evaluation of renal and perirenal leiomyoma on US, CT, and angiography. Radiat Med. 1993;11:81-5.
- [Google Scholar]






