Translate this page into:
Role of Advanced MRI Brain Sequences in Diagnosing Neurological Complications of Scrub Typhus
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Scrub typhus is a rare disease affecting many organs and causing vasculitis by affecting the endothelium of blood vessels. Review of literature shows that there are only a few case reports describing the neuroradiological manifestations of scrub typhus. This case report describes how newer and advanced MRI sequences are able to diagnose neurological complications of scrub typhus, such as hemorrhages, meningoencephalitis, infarctions, cranial nerve involvement, thrombosis, and hypoperfusion, that are not picked up on routine magnetic resonance imaging (MRI) sequences.
Keywords
Eschar
hypoperfusion
scrub typhus
vasculitis
INTRODUCTION

Scrub typhus, also known as tsutsugamushi disease, is an acute febrile illness caused by infection due to Orientia tsutsugamushi. The causative agent affects the endothelial lining of the blood vessels resulting in perivascular cellular infiltrates, which result in vasculitis. People engaged in agricultural activities become victims of this disease on being bitten by trombiculid mite found in areas with heavy scrub vegetation.[1] Infection spreads through both hematogenous and lymphatic routes. The description of a classic case includes an eschar at the site of chigger bites, regional lymphadenopathy, and a maculopapular rash.[123] Chills and fever occur 3–4 days after the bite. Rash and lymphadenopathy appear at end of the first week.[14] Myocarditis and encephalitis are the most life-threatening complications. We present a case report of an 18-year-old female who was diagnosed with scrub typhus. The neurological complications which were missed on routine MRI sequences were identified on advanced MRI sequences.
CASE REPORT
An 18-year-old female presented to the emergency department in an unconscious state. She had developed fever and rash 3 days earlier. On examination, the patient was unconscious, febrile, had maculopapular rash throughout her body, and an eschar was noted on the right side of the pubic region [Figure 1]. Based on the clinical diagnosis of scrub typhus, MRI brain was done immediately. Scan revealed micro-hemorrhages in the body and splenium of corpus callosum, as well as in the sub-cortical white matter in bilateral centrum semiovale region [Figure 2a and b]. There was no mass effect or perilesional edema. These petechial hemorrhages were appreciated only in the susceptibility-weighted minimum intensity projection images. In post-contrast magnetization prepared rapid acquisition gradient recall echo (MP RAGE) sequence, there was enhancement of the pachymeninges along bilateral frontotemporoparietal lobes [Figure 2c]. Rest of the brain parenchyma was normal. No restriction was visualized on diffusion-weighted (DW) and apparent diffusion coefficient (ADC) sequences and there was no altered signal intensity on T2 and fluid-attenuated inversion recovery (FLAIR) sequences [Figure 3]. Time of flight (TOF) MRI angiography revealed normal vessels of circle of Willis. Arterial spin labeling (ASL) perfusion showed normal cerebral blood flow. A diagnosis of scrub typhus was made with the radiological findings identifying the pathology of vasculitis and meningitis.
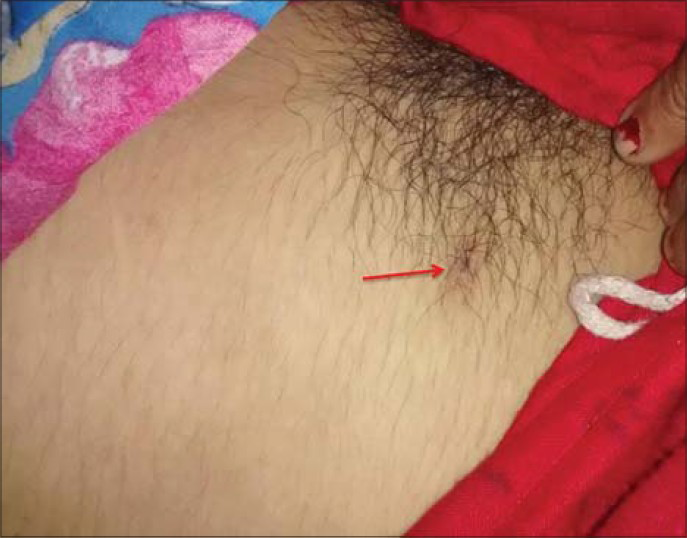
- 18-year-old adult female who presented to the emergency department in an unconscious state with fever and rash was diagnosed with scrub typhus. The photograph of the patient shows presence of eschar on the right side of the pubic region (red arrows).
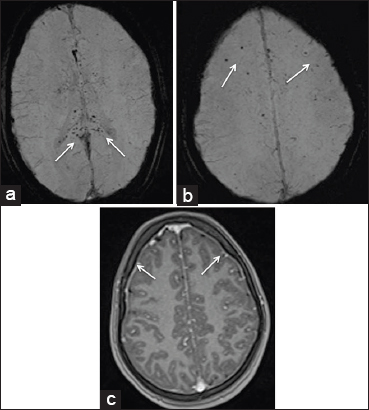
- 18-year-old adult female who presented to the emergency department in an unconscious state with fever and rash was diagnosed with scrub typhus. (a and b) SWI images of MRI brain show multiple petechial hemorrages in the splenium and body of corpus callosum (white arrows in 2a) and in the subcortical white matter (white arrows in 2b). (c) Post-contrast MP RAGE axial image shows enhancement of pachymeninges along the frontal lobe bilaterally (white arrows).
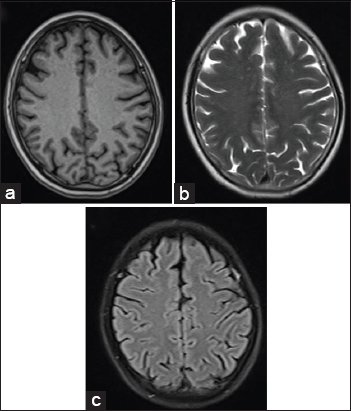
- 18-year-old adult female who presented to the emergency department in an unconscious state with fever and rash was diagnosed with scrub typhus. The routine MRI sequences (a) T1, (b) T2, and (c) FLAIR show no abnormal signal intensity in the brain parenchyma.
On enzyme-linked immunosorbent assay (ELISA), antibody IgM was positive for scrub typhus showing an optical density (OD) of 2.546 which was much greater than the baseline OD of 0.4. The patient was put on intravenous azithromycin. There was marked clinical improvement in her rash, fever, and level of consciousness.
DISCUSSION
Scrub typhus is a major health problem. The disease is clinically important because of its serious complications and fatality rates that were upto 50% in the pre-antibiotic era.
Scrub typhus was known in China in the 3rd century AD. In 1810 BC, it was described by Hakuju Hashimoto in people living on the banks of the Shinano river, and later by Baelz and Kawakami. In Japanese, it is known as “flood fever.” Tsutsugamushi is a Japanese term. Tsutsuga means “illness” and mushi means “insect/creature.” Taiwan is the center of the tsutsugamushi triangle.
In India, the first reported case was in Himachal Pradesh in 1934 and, interestingly, this case report is also from the same state of India.[4] We do not have definite statistics of scrub typhus in India due to lack of awareness, unavailability and high cost of diagnostic kits, and the fact that it is not a reportable illness. There are only a few case reports on the neuroradiological manifestations of scrub typhus in the literature.
Both the central and peripheral nervous systems are involved in scrub typhus. Aseptic meningitis occurs in about 11% of patients with scrub typhus.[34] Other CNS complications include meningoencephalitis, infarction,[2456] cerebellitis,[34] hemorrhages,[47] encephalitis, demyelination,[48] subdural hematoma,[4] and typhus nodules.[2456] Low platelet counts and disseminated intravascular coagulation (DIC) contribute toward hemorrhage.[4]
Susceptibility-weighted imaging (SWI) is a high-spatial-resolution 3D gradient-echo MR imaging technique with phase post-processing that accentuates the paramagnetic properties of blood products such as deoxyhemoglobin, intracellular methemoglobin, and hemosiderin. It is particularly useful for detecting intravascular venous deoxygenated blood as well as extravascular blood products. Vasculopathies and vasculitis are associated with cerebral microbleeds, which are well detected on SWI.
In this case, we want to emphasize the fact that newer and advanced MRI sequences such as SWI and contrast-enhanced MP RAGE sequence, which is a 3-dimensional T1-weighted gradient sequence that provides excellent gray and white matter differentiation, were able to pick up the abnormality in the brain while these were not seen in routine MRI sequences. More research work is required to prove that new MRI sequences like arterial spin labeling (ASL), diffusion tensor imaging (DTI), magnetic resonance spectroscopy (MRS) time of flight (TOF), and dynamic susceptibility-weighted perfusion play a major role in diagnosing this rare and life-threatening, yet a treatable disease which has high mortality and morbidity rates.
CONCLUSION
In patients having scrub typhus and presenting with altered sensorium, neurological complications should be suspected, as early diagnosis and treatment will alter the prognosis and reduce the mortality rate. Advanced MRI sequences play an important role in diagnosing the neurological complications of scrub typhus.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2015/5/1/11/152340
Source of Support: Nil
Conflict of Interest: None declared.
REFERENCES
- Scrub typhus: Clinical, pathologic, and imaging findings. Radiographics. 2007;27:161-72.
- [Google Scholar]
- Central nervous system involvement in patients with scrub typhus. Clin Infect Dis. 1997;24:436-40.
- [Google Scholar]
- Scrub typhus complicated by intracranial hemorrhage - A case report. Tzu Chi Med J. 2005;17:111-4.
- [Google Scholar]
- Scrub typhus meningitis in South India - A retrospective study. PLoS One. 2013;8:e66595.
- [Google Scholar]
- Scrub typhus with central nervous system involvement: A case report with CT and MR imaging features. Neurol J Southeast Asia. 1999;4:53-7.
- [Google Scholar]
- Scrub typhus encephalomyelitis with prominent focal neurologic signs. Arch Neurol. 2000;57:1770-2.
- [Google Scholar]
- Polyneuropathy and cerebral infarction complicating scrub typhus. J Clin Neurol. 2008;4:36-9.
- [Google Scholar]
- Scrub typhus meningo-encephalitis with focal neurologic signs and associated brain MRI abnormal findings: Literature review. Clin Neurol Neurosurg. 2011;113:250-3.
- [Google Scholar]






