Translate this page into:
Krukenberg Tumor: A Rare Cause of Ovarian Torsion
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Ovarian torsion is the fifth most common gynecological surgical emergency. Ovarian torsion is usually associated with a cyst or a tumor, which is typically benign. The most common is mature cystic teratoma. We report the case of a 43-year-old woman who came to the Emergency Department with rare acute presentation of bilateral Krukenberg tumors, due to unilateral ovarian torsion. In this case report, we highlight the specific computed tomography (CT) features of ovarian torsion and demonstrate the unique radiological findings on CT imaging. Metastasis to the ovary is not rare and 5 to 10% of all ovarian malignancies are metastatic. The stomach is the common primary site in most Krukenberg tumors (70%); an acute presentation of metastatic Krukenberg tumors with ovarian torsion is rare and not previously reported in radiology literature.
Keywords
CT torsion
Krukenberg tumor
ovarian torsion
INTRODUCTION

Ovarian torsion results from the rotation of the ovary about its pedicle, to an extent that the ovarian arteries and or veins are obstructed. This condition generally results from a benign tumor of the ovary and usually occurs in younger women. Clinical signs include sudden onset of lower abdominal pain associated with other constituitional symptoms like nausea and vomiting.
In 1896, Fredrick Krukenberg described a new type of ovarian tumor. This tumor was later identified as a malignancy in the ovary from a primary lesion in the gastrointestinal tract, and named “Krukenberg tumor” after him. Presentation of a Krukenberg tumor with ovarian torsion is a rare event which we will detail in this case report.
CASE REPORT
A 43-year-old female, (gravida 2, para 2) presented to the Emergency Department (ED) with an acute onset of right lower quadrant abdominal pain, which was severe and progressive in intensity. The pain was episodic, with associated diarrhea. Gynecological examination revealed a large fixed fluctuant abdominal mass within the pelvis, extending above the umbilicus. Working diagnosis in the ED was cystic abdominal mass of unknown origin, likely ovarian. The initial laboratory workup revealed anemia and hypokalemia. Urine analysis was positive for protein and ketones.
A contrast-enhanced CT scan of the abdomen and pelvis was ordered and revealed a large poorly enhancing, predominantly cystic mass arising from the left adnexa, measuring 21.6 cm craniocaudal × 11.7 cm AP (anteroposterior) × 22.8 cm transverse, with numerous thin non-enhancing septations and small vessels coursing throughout the lesion [Figure 1]. The mean attenuation value of the mass ranged from 8–14 Hounsfield Units, confirming its predominantly cystic nature.
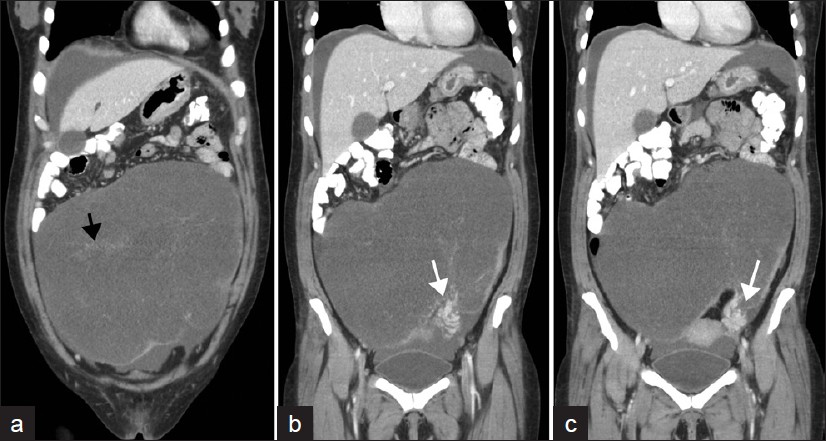
- Contrast-enhanced coronal CT images of the abdomen and pelvis, demonstrate a large predominantly cystic left adnexal mass containing multiple septations almost completely occupying the abdomen (black arrow). The twisted vascular pedicle in the left lower quadrant demonstrates a whirlpool sign (white arrows) (similar to what is described in the ultrasound literature).
The mass demonstrated a discrete vascular pedicle in the left hemi-pelvis in the vicinity of the round ligament of the ovary with enhancing engorged vessels in the pedicle. There was a discrete ‘vascular swirl sign’ appreciated at the left ovarian vascular pedicle, suggesting that this represented a massively enlarged left ovary with a significant torsion of greater than 270 degrees. These findings helped clinch the diagnosis of an ovarian torsion [Figure 4(a-d)].
A second large mass measuring 5.3 cm craniocaudal × 6.5 cm AP × 5.4 cm transverse, originating from the contralateral right ovary with enhancing solid rind and central hypoattenuation, representing the right ovarian Krukenberg tumor [Figure 2] was also noted. The uterus appeared unremarkable. A small amount of free fluid was noted in the abdomen and pelvis.
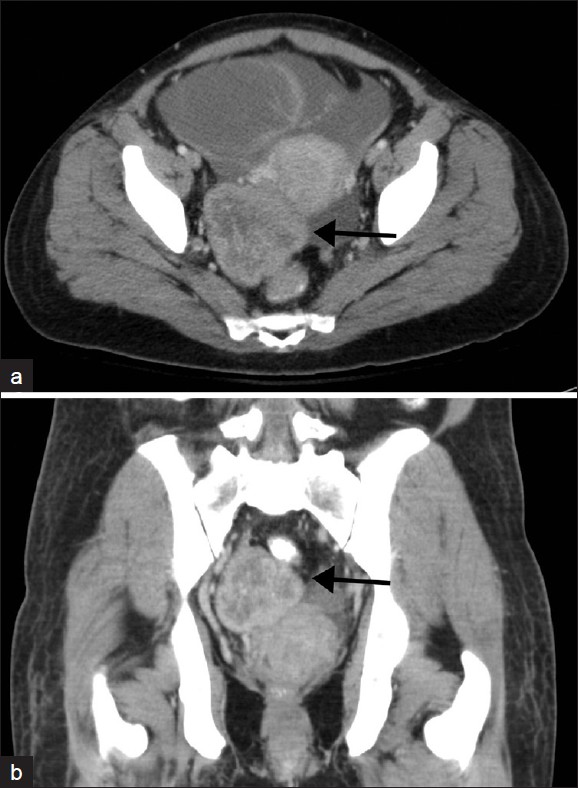
- (a) Contrast-enhanced axial and (b) coronal CT images through the pelvis demonstrate a solid heterogeneously enhancing right-adnexal mass, with a thick enhancing rind, consistent with a Krukenberg Tumor (arrow).
The presence of bilateral ovarian masses strengthened the initial diagnosis of Krukenberg tumors and an attempt was made to assess the primary lesion. There was an irregular plaque-like, mildly enhancing, mass-like area in the mid-gastric body, along the lesser curvature, relating to a primary gastric malignancy [Figure 3]. Other relevant findings included peritoneal / serosal implants and mild right hydroureteronephrosis due to extrinsic compression of the right ureter from the right adnexal mass.
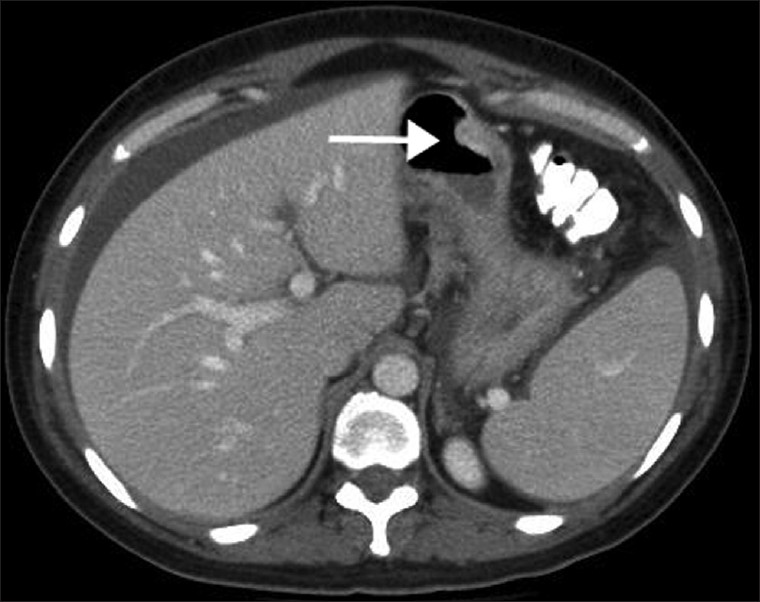
- Contrast-enhanced axial CT at the level of the liver reveals a focal nodular thickening of the gastric body along the greater curvature and antrum (arrow) suggestive of gastric carcinoma that was subsequently confirmed by histopathology.
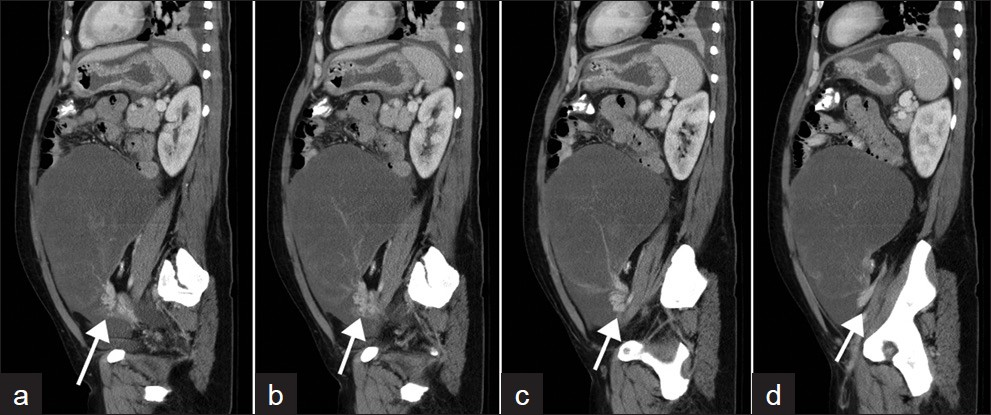
- Four contiguous sagittal images showing a discrete ‘swirl sign’ at the vascular pedicle (white arrows) at the base of the large left ovarian mass, consistent with the torsion of ovarian Krukenberg tumor at its pedicle.
The patient underwent esophagogastroduodenoscopy / colonoscopy showing a large friable ulcer located in the posterior wall of the stomach measuring approximately 10 cm, extending to both the lesser and greater curvature, showing a concern for malignancy [Figure 3]. Extrinsic compression of the pelvic colon was seen due to the large mass.
The patient subsequently underwent an exploratory laparotomy, bilateral salpino-oophrectomy, total gastrectomy, and esophagojejunostomy. A gross pathological examination revealed a 26 cm left ovarian tumor, smaller right ovarian tumor, disseminated metastases in the peritoneum, and gastric tumor within the body of the stomach.
Microscopic pathology from the gastric specimen revealed a poorly differentiated gastric adenocarcinoma of the signet cell type, while ovarian pathology showed metastatic bilateral Krukenberg tumors from the gastric carcinoma, with signet cell histology similar to the primary tumor [Figure 5].
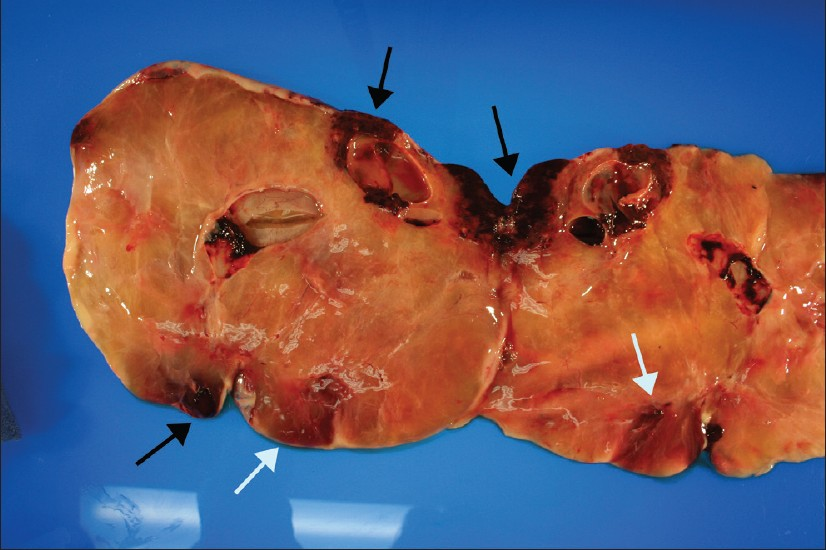
- A gross image of bi-valved left ovary weighing 2475 g and measuring 26 × 21 × 6 cm. Note the large hemorrhagic area on one end of the ovary (white arrow), measuring 11 × 5 × 2.5 cm, and other smaller areas of hemorrhage within the solid ovarian mass. The black arrows depict areas of infarction. (The deceptive cystic appearance on CT was due to a poor flow, with large areas of infarction).
DISCUSSION
Krukenberg tumors are defined as any malignant process metastatic to the ovaries. These tumors are relatively uncommon and account for only one to two percent of all ovarian tumors.[12] These tumors primarily originate from carcinomas of the gastrointestinal tract and less commonly from the breast, gallbladder, colon, appendix, or pancreas.[2] Microscopically, these tumors are characterized by mucin-secreting signet ring cells in the ovarian tissue and in the primary tumor site.[34] A review of literature indicates that 35 to 45% of the patients were younger than 40 years of age, with an average range of 40 to 46 years.[5]
Although unanswered for a long time, it is now apparent that a retrograde lymphatic spread is the most common route for the spread of metastasis of gastric carcinoma to the ovaries.[6] Less common pathways of metastasis to the ovary occur via the peritoneum and vasculature.[67]
Patients typically present with this problem in their fourth or fifth decade of life. The common presenting symptoms are related to the ovary and include abdominal pain and distension due to the bilateral, often large ovarian masses. In addition, ascites is a common presentation in the Krukenberg tumor and usually reveals malignant cells.[2] However, there has been a reported case of bilateral Krukenberg tumors with benign ascites and right hydrothorax that revealed no malignant cells. This is known as pseudo-Meig syndrome, in contrast to the Meig syndrome, which presents with a triad of benign ovarian tumor, ascites, and right-sided hydrothorax.[8]
In general, patients with a Krukenberg tumor have a poor prognosis, with most patients averaging two years life expectancy, with a median survival time of 14 months.[9] Studies have shown that prognosis is poor when the primary tumor is identified after metastasis of the cancer to the ovaries. Currently, no optimal treatment plan has been established for Krukenberg tumors.[210]
Our case is unusual in that, the initial presentation of a gastric malignancy was acute ovarian torsion due to an ovarian Krukenberg tumor acting as a lead point for torsion. Ovarian torsion is the twisting of an ovary on its ligamentous supports and can result in a compromised blood supply. Adnexal torsion is a term that is inclusive of either the ovary, fallopian tube, or both. Concomitant ovarian and tubal torsion has been shown to occur in up to 67% of the cases of adnexal torsion.[11]
An ultrasound is the first modality to evaluate the ovary and ovarian torsion. The main sonographic features of an ovarian torsion include a morphologically abnormal ovary, with or without ovarian blood flow. The presence of blood flow within the ovary does not exclude ovarian torsion, it suggests that the ovary is viable and can be salvaged with surgery. As this patient presented to the ER with severe abdominal pain and a significant increase in abdominal girth, the first imaging study ordered in the ED was a contrast-enhanced CT of the abdomen and pelvis, due to suspected malignancy or any other acute abdominopelvic process, thus bypassing the typical first line abdominopelvic ultrasound, to save time. Computed tomography is usually used as an adjunct modality when diagnosis is not straightforward on ultrasound and also when a wider field of view is needed, as in the case of our patient. The CT features of an ovarian torsion are summarized in Table 1.

On magnetic resonance imaging (MRI), the appearance of the Krukenberg tumor is dependent on the degree of stromal overgrowth and mucin production. Dense stromal reaction gives a hypointense signal and mucin material usually gives a hyperintense signal on T2W images. The presence of hypointense solid components within an ovarian solid mass is a characteristic, but a nonspecific finding for Krukenberg tumors.
Although the patient was in the average age range for Krukenberg tumors,[5] benign ovarian neoplasms and benign pathologies are typically more common. The most common tumor predisposed for ovarian torsion is the benign mature cystic teratoma.
Currently, in radiology literature, there are no reported cases of Krukenberg tumors presenting to the ED with acute ovarian torsion. Although uncommon, Krukenberg tumors should be considered in the differential diagnosis of ovarian torsion, in addition to benign entities such as mature cystic teratoma.
Source of Support: Nil
Conflict of Interest: None declared.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2012/2/1/6/93038
REFERENCES
- Krukenberg tumour of the ovary: A case report with light microscopy, immunohistochemistry and electron microscopy study. Anticancer Res. 2008;28:1417-20.
- [Google Scholar]
- Metastatic tumors of the ovary. In: Kurman RJ, ed. Blaustein's pathology of the female genital tract (4th ed). New York: Springer; 1994. p. :939-74.
- [Google Scholar]
- Krukenberg tumor from an occult appendiceal adenocarcinoid: A case report and review of the literature. Eur J Obstet Gynecol Reprod Biol. 2001;97:90-5.
- [Google Scholar]
- Krukenberg Tumors of the ovary: A clinicopathologic analysis of 120 cases with emphasis on their variable pathologic manifestations. Am J Surg Pathol. 2006;30:277-99.
- [Google Scholar]
- Early gastric cancer with Krukenberg tumor and review of cases of intramucosal gastric cancers with Krukenberg tumor. J Gastroenterol. 2003;38:1176-80.
- [Google Scholar]
- Risk factors for ovarian metastases following curative resection of gastric adenocarcinoma. Cancer. 1999;85:1490-9.
- [Google Scholar]
- A long surviving case of Pseudomeigs’ syndrome caused by Krukenberg tumor of the stomach. Jpn J Clin Oncol. 2005;35:221-3.
- [Google Scholar]






