Translate this page into:
Intestinal Obstruction from Congenital Bands at the Proximal Jejunum: A Case Report and Literature Review
Address for correspondence: Dr. Debkumar Sarkar, Department of Radiology, Cooper University Hospital, 1 Cooper Plaza, Ste. B-23, Camden, NJ 08103, USA. E-mail: sarkar debkumar@cooperhealth.edu
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Congenital anomalous bands at the proximal jejunum resulting in obstruction have been described sporadically in the literature and are otherwise rare. We present a case of an 8 year-old girl with a nine-month history of intermittent vomiting and no history of prior surgery. The imaging workup includes an abdominal ultrasound, a single contrast upper gastrointestinal series, and a dual contrast computed tomography of the abdomen and pelvis. Surgical intervention revealed the presence of dense bands at the proximal jejunum without evidence of malrotation. Our report reviews the embryology and radiologic findings of this entity using different imaging modalities.
Keywords
Congenital bands
intestinal obstruction
proximal jejunum
INTRODUCTION

Intussusception is the most common cause of bowel obstruction in infants and young children.[12] Congenital causes of intestinal obstruction include duodenal atresia, malrotation, duodenal obstruction from Ladd bands, other congenital bands, superior mesentery artery syndrome, enteric duplications as well as several other entities. Congenital anomalous bands resulting in proximal jejunal obstruction are a rare entity that should be considered in the differential in patients with clinical signs of obstruction and no prior history of abdominal surgery. We present a case of an 8 year-old girl with a nine-month history of intermittent vomiting and no history of prior surgery and review the embryology and radiologic findings of this entity using different imaging modalities.
CASE REPORT
An 8 year-old girl with a past medical history of constipation presented with a history of vomiting for nine months. The vomiting was intermittent, non-bloody, at times bilious, and occasionally contained food particles. An abdominal ultrasound was performed which demonstrated debris within a dilated proximal duodenum. The superior mesenteric artery (SMA) and superior mesenteric vein (SMV) were visualized with the SMA lying to the left of the SMV with normal anatomic alignment [Figure 1]. No large solid or cystic masses were seen.
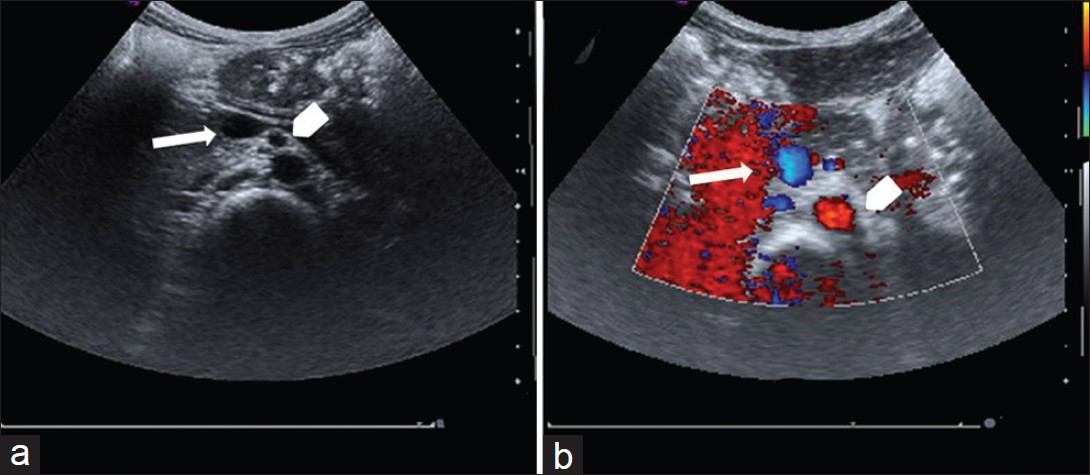
- (a) Ultrasound of mid abdomen shows superior mesentery vein (arrow) and superior mesentery artery to the left (b) The doppler flow study confirms arterial flow in the superior mesentery artery (arrowhead) and the venous flow in the uncompressed superior mesenteric vein (arrow).
A standard barium single contrast upper gastrointestinal (UGI) series was performed with the contrast entering the antrum and duodenal bulb. The proximal duodenum and descending duodenum were markedly dilated in caliber with apparent tapering of the third part of the duodenum. There was an abrupt cutoff with no contrast extending beyond approximately the mid abdomen [Figure 2]. Delayed images were obtained while the patient was supine with contrast never extending beyond the third portion of the duodenum [Figure 3].
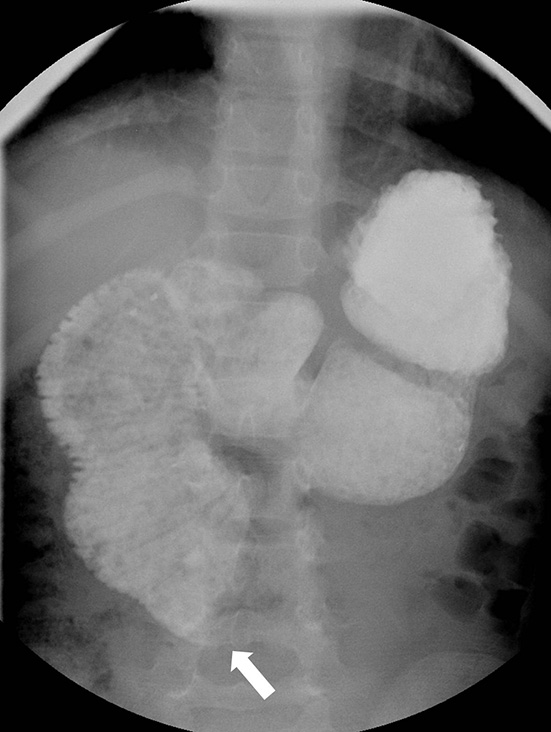
- Single contrast upper gastrointestinal series shows on a single view plain radiograph the contrast abruptly cutting off approximately at the mid abdomen (arrow).
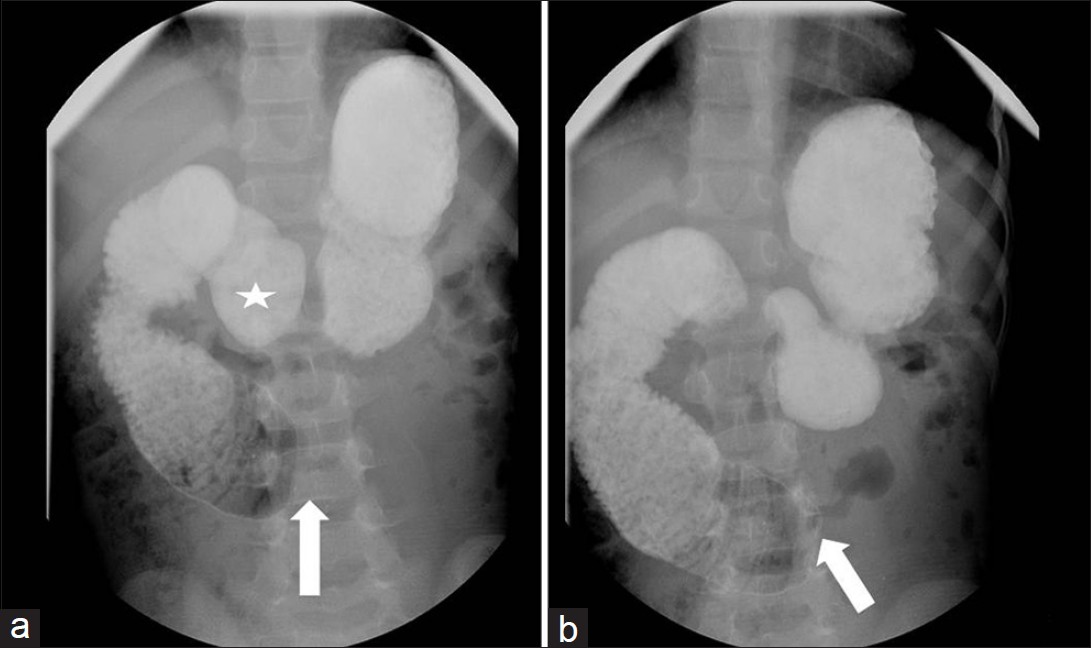
- Single contrast upper gastrointestinal series shows on delayed images with patient laying supine, contrast never extending beyond third portion of duodenum with persistent cutoff (arrow). Contrast is seen in antrum of stomach (star), proximal duodenum, and descending duodenum.
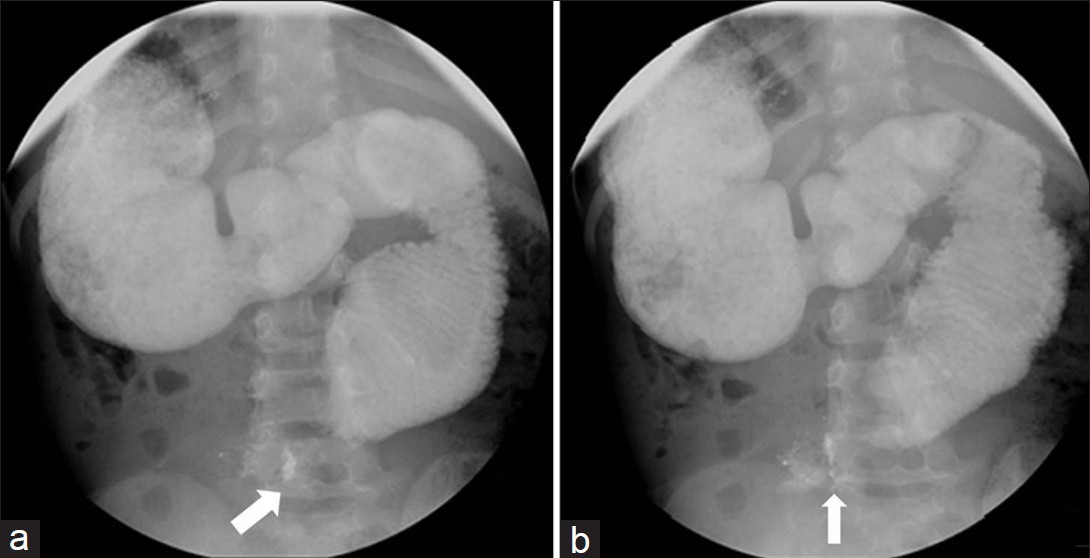
Patient was subsequently placed prone for several minutes with eventual slight transit of contrast [Figure 4]. Thirty minute delayed prone images demonstrated contrast in the proximal small bowel, however proximal duodenum remained markedly dilated and contrast/debris filled [Figure 5]. Additionally delayed overhead images demonstrated contrast extending to the distal small bowel after patient had been upright for greater than 30 minutes [Figure 6]. Markedly dilated proximal duodenum with abrupt cutoff in the third portion of the duodenum raised concern for a questionable mass like positionally dependent extrinsic compression of the third portion of the duodenum.
- Delayed prone images demonstrated contrast in the proximal small bowel with persistent dilatation of the proximal duodenum.
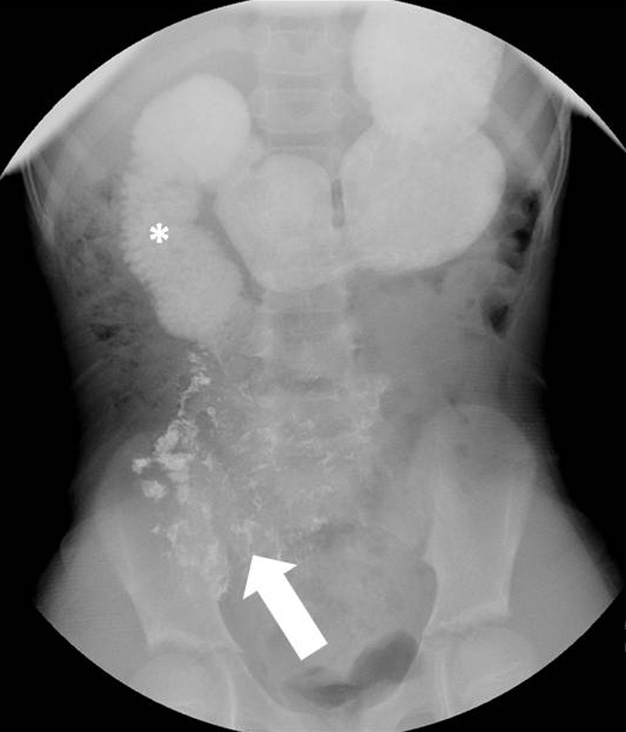
- Additional delayed image following several minutes of prone position demonstrates a small amount of contrast progressing to the jejunum (arrow). There is persistent dilatation of the proximal duodenum (asterisk).
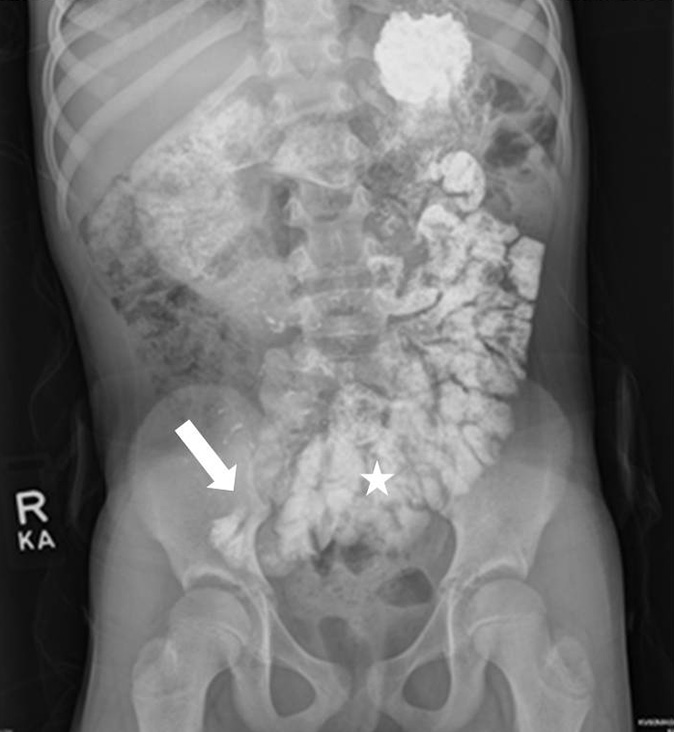
- Delayed abdominal radiograph following the upper gastrointestinal series after patient had been upright for greater than 30mins demonstrates further progression of contrast into the jejunum and ileum (star). Distal most extent of contrast near the cecum (arrow).
A subsequent computed tomography (CT) of the abdomen and pelvis was performed with oral and intravenous contrast. The duodenum was distended with the third part of the duodenum tented downward [Figure 7]. The duodenal/jejunal junction was severely narrowed and coursed distally anterior to the right common femoral artery below the bifurcation [Figure 7].
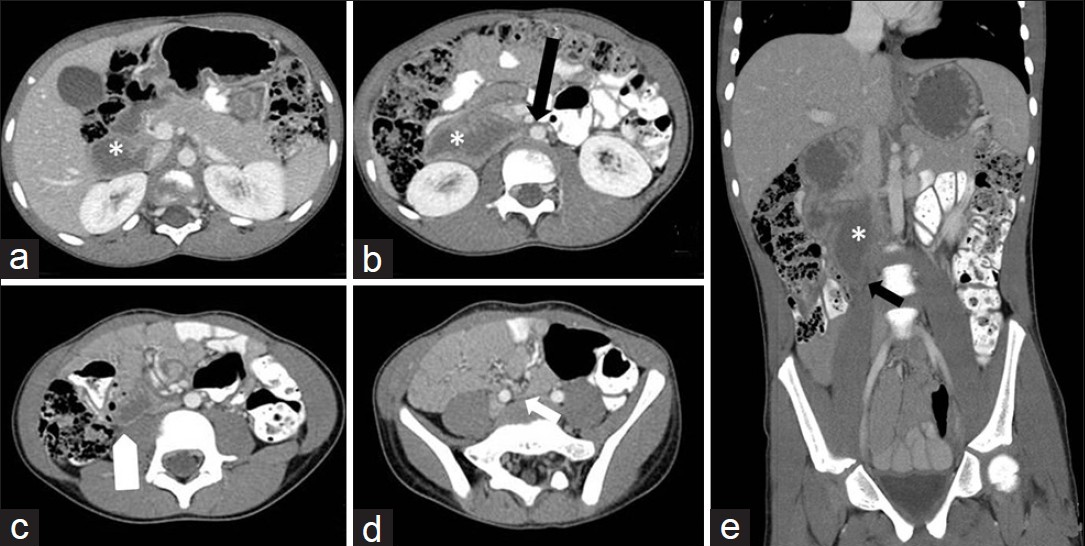
- Computed tomography (CT) of the abdomen and pelvis shows dilated fluid filled duodenum (asterisk, a). Duodenum tented medially (black arrow, b) and downward (white arrow, c, black arrow, e). Duodenum severely narrowed as it crosses anterior to right femoral vein below the bifurcation (white arrow, d).
The patient was taken for an exploratory laparotomy and found to have dense vascularized bands without intestinal malrotation. Upon entering the abdomen, the cecum was noted to be in normal anatomical position. Further exploration in the abdomen revealed the proximal jejunum tethered by dense vascularized bands running from approximately five inches distal to the ligament of Treitz down into the pelvis. The cecum was incidentally noted to be folded back on itself and adherent to this tented portion of the jejunum. After these adhesions were ligated, the bowel was examined and no other anatomical abnormalities were discovered. The patient experienced a normal post-operative course with subsequent complete resolution of symptoms.
DISCUSSION
The congenital causes of intestinal obstruction in infants and children are intestinal atresia and stenosis, congenital bands, remnants of embryologic structures such as vitelline arteries or veins, omphalomesenteric ducts or a mesourachus.[34] In addition abnormal mesenteric fixation can lead to intestinal malrotation with possible midgut volvulus. Intestinal obstructions caused by other anomalous congenital bands have only been described sporadically in the literature and are otherwise rare.[5–7]
An example of anomalous congenital bands is Ladd bands. These bands are made of peritoneal fibrous tissue and result in anomalous mesenteric fixation.[8] They arise from the cecum and extend to the sub-hepatic region, posterior peritoneum or abdominal wall. Ladd bands result in compression of the 2nd or 3rd duodenal portions, which lead to intestinal obstruction.[8]
The origin of anomalous congenital bands is not well understood. However, the location of these bands is different from embryonic remnants such as vitelline vessels or omphalomesenteric ducts.[679] Akgur et al., cited a few series of cases to suggest that these bands are the result of a mesenteric developmental anomaly. Mesenteric anomalies have not been well documented aside from cases of malrotation and anomalous intestinal fixation.
In our patient, upper gastrointestinal (UGI) barium examination showed a dilated duodenum near the ligament of Treitz with sharp obstruction. Therefore, external compression was more likely than intrinsic stenosis. Most duodenal obstructions by external compression are caused by abnormal duodenal rotation with internal herniation or Ladd bands. In our patient the duodenal rotation was normal.[7]
Our case is particularly rare as abnormal dense vascularized bands were seen distal to the ligament of Treitz, which is not characteristic of Ladd bands. This resulted in dilatation of the proximal jejunum which was not readily identified on the UGI barium examination. Though imaging demonstrated a high grade obstruction, the patient's symptoms were chronic and mild. Furthermore prone positioning partially alleviated the degree of obstruction presumably by altering the position of the anomalous bands and relieving the obstruction.
Finding an anomalous band tethering the proximal jejunum to the pelvis and adhering the jejunum and cecum is unique and unlike previously described congenital peritoneal bands. As no previous operation had been performed on this patient and operative findings did not show any other abnormal post inflammatory adhesions between the small and large intestines, the etiology of these bands was determined to be congenital.[9]
A similar case described by Liu et al., discovered a band running from the antimesenteric wall of the proximal jejunum just distal to the Treitz's ligament to the root of the mesentery. The anomalous congenital band in that case was considered to be the remnant of ventral mesentery that failed to resorb completely.[7] In both our case and the case described by Liu et al., the location excludes known embryogenic remnants and thus suggests anomalous mesenteric development.
External compression of the proximal jejunum by an anomalous band should be included in the differential diagnosis of obstruction of the distal duodenum or duodeno-jejunal junction for patients without previous history of surgery, especially when UGI barium examination shows normal duodenal rotation and duodeno-jejunal fixation.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2012/2/1/78/105130
Source of Support: Nil
Conflict of Interest: None declared.
REFERENCES
- Exploratory laparotomy for acute intestinal conditions in children: A review of 10 years of experience with 334 cases. Afr J Paediatr Surg. 2011;8:62-9.
- [Google Scholar]
- Assessment of recurrent abdominal symptoms after Ladd procedure: Clinical and radiographic correlation. J Pediatr Surg. 2011;46:1720-5.
- [Google Scholar]
- Vitelline artery remnant causing intestinal obstruction in an adult. Surgery. 2012;21
- [Google Scholar]
- Anomalous congenital bands causing intestinal obstruction in children. J Pediatr Surg. 1992;27:471-3.
- [Google Scholar]
- Sigmoid adhesion caused by a congenital mesocolic band. J Gastroenterol. 1999;34:626-8.
- [Google Scholar]
- Obstruction of the proximal jejunum by an anomalous congenital band-A case report. J Pediatr Surg. 2005;40:E27-9.
- [Google Scholar]
- Radiographic patterns of intestinal malrotation in children. Radiographics. 1996;16:547-56.
- [Google Scholar]
- Anomalous congenital band: A rare cause of intestinal obstruction and failure to thrive. Pediatr Surg Int. 2005;21:1018-20.
- [Google Scholar]






