Translate this page into:
Fibro-osseous Lesions of the Jaw: A Report of Two Cases
Address for correspondence: Dr. Guruprasad Yadavalli, Department of Oral and Maxillofacial Surgery, AME's Dental College Hospital and Research Centre, Raichur-584 103, Karnataka, India. E-mail: guru_omfs@yahoo.com
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Fibro-osseous lesions of the maxillofacial bones comprise a diverse group of pathologic conditions that include developmental lesions, reactive or dysplastic diseases, and neoplasms. The concept of fibro-osseous lesions has evolved over the last several decades and now includes two major entities: fibrous dysplasia and ossifying fibroma. The less common lesions include florid osseous dysplasia, periapical dysplasia, focal sclerosing osteomyelitis, proliferative periostitis of Garre, and osteitis deformans. We report two cases, the first, a craniofacial polyostotic fibrous dysplasia, and the second, a juvenile ossifying fibroma of maxilla.
Keywords
Craniofacial
fibro-osseous lesions
fibrous dysplasia
juvenile ossifying fibroma
INTRODUCTION

Fibro-osseous lesions are a diverse group of processes that are characterized by replacement of normal bone by fibrous tissue containing a newly formed mineralized product. Commonly included among the fibro-osseous lesions of the jaws are fibrous dysplasia, cemento osseous dysplasia, and ossifying fibroma.[1] We report two cases of which one is craniofacial polyostotic fibrous dysplasia and another is juvenile ossifying fibroma (JOF) of the maxilla.
CASE REPORTS
Case 1
A 16-year-old girl had developed a swelling on the right side of the face that had persisted for one year [Figure 1]. There was no history of pain, trauma, epistaxis, loosening of teeth, trismus, or diminished vision. Examination of the region revealed a smooth bone hard swelling involving the right maxilla, zygoma, temporal, and mandibular regions. The skin over the swelling was normal. The swelling was bulging into the gingivo-buccal sulcus area. The teeth were normal. There was no other swelling in the body and cafe-au-lait spots were not seen. The throat and nose examination was found to be normal. The blood and urine investigations were normal. The computed tomography (CT) scan [Figures 2–4] showed a radio-dense mass involving the right frontal, temporal, zygomatic, maxilla, and mandible causing facial asymmetry. There was a ground-glass appearance and expansion of the involved bones. Postero-anterior (PA) view of the skull showed a diffuse radiopacity with faint, linear to irregular central opacities [Figure 5]. An incisional biopsy was subsequently performed, providing a diagnosis of fibrous dysplasia. Based on the clinical history, radiographic, and histologic features of the lesion, a diagnosis of craniofacial polyostotic fibrous dysplasia was established.
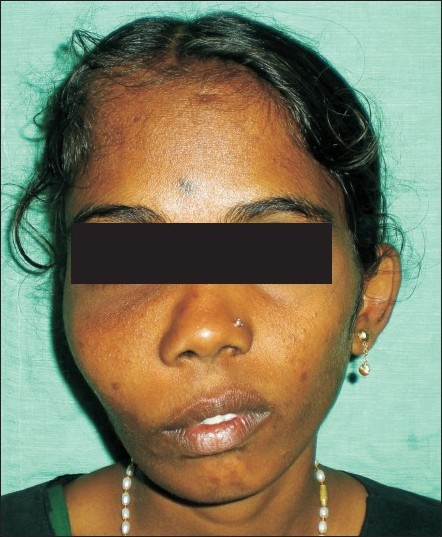
- 16-year-old girl with a swelling on the right-side of the face at the time of evaluation.
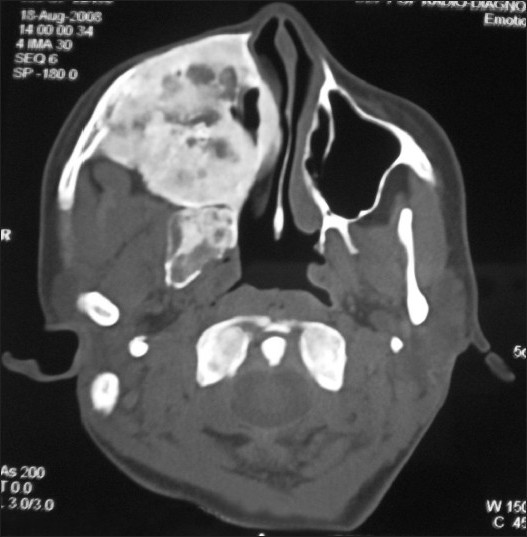
- Axial CT image shows a radioopaque lesion occupyng most of the facial area in the mid and upper facial skeleton on the right side, which is significantly expanded. The maxillary sinus and nasal airway on the right are obliterated.
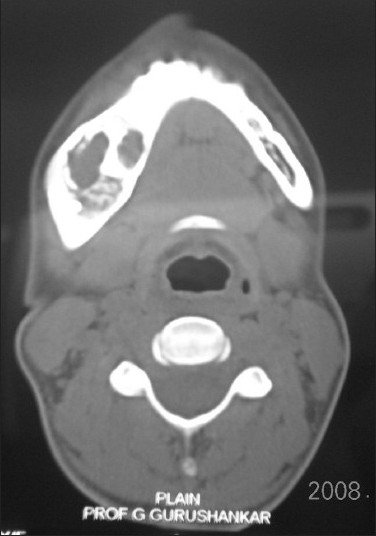
- Axial CT image shows expansion of the right mandibular buccal cortical plate with radiopaque and radiolucent changes.
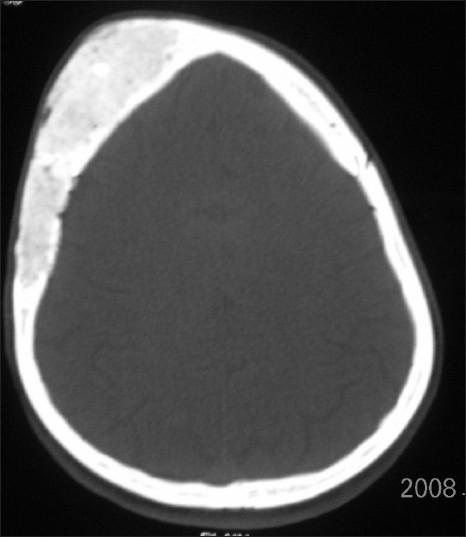
- Axial CT image shows expansion of the right frontal and temporal bones.
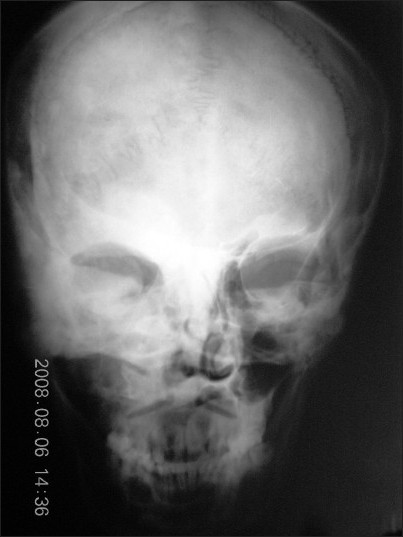
- PA view of skull shows diffuse radiopacity with faint, linear to irregular central opacities.
Case 2
A 14-year-old girl was referred for the evaluation of a left facial swelling [Figure 6]. Both the patient and her parents had been aware of the swelling for approximately 2 years, but had delayed evaluation because of economic circumstances. The lesion had been slowly increasing in size, since it was first noticed. There was no history of trauma, pain, paresis, paresthesia, or lymphadenopathy. Physical examination showed a healthy, normally developed young girl in no apparent distress. There was significant facial asymmetry caused by an approximately 5 cm × 5 cm mass involving the left maxilla. The mass was firm to palpation and not adherent to the overlying skin. No bruits or pulsations were detected. Intraoral examination showed expansion of the left buccal cortex, which was firm on palpation. There was no evidence of tooth mobility, abscess formation, dehiscence, or malocclusion. A panoramic radiograph showed a well-circumscribed radiopacity with faint, linear to irregular central opacities. Teeth 23, 24, and 25 were noted to be missing with a history of extraction due to mobility [Figure 7]. There was evidence of tooth displacement in relation to 21, 27, 28, and root re-absorption in relation to 21, 26 [Figure 8]. CT scan of the left maxilla showed medial and lateral cortical expansion and areas of central calcification with obliteration of the left maxillary sinus [Figure 9]. Laboratory values were within normal limits. An incisional biopsy was subsequently performed, providing a diagnosis of JOF.
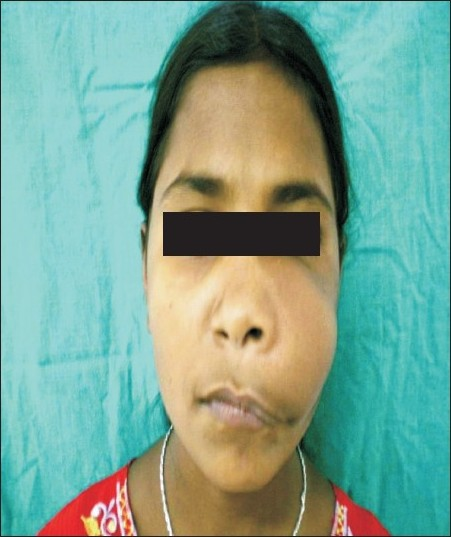
- 14-year-old girl with swelling on the left-side of the face at the time of evaluation.
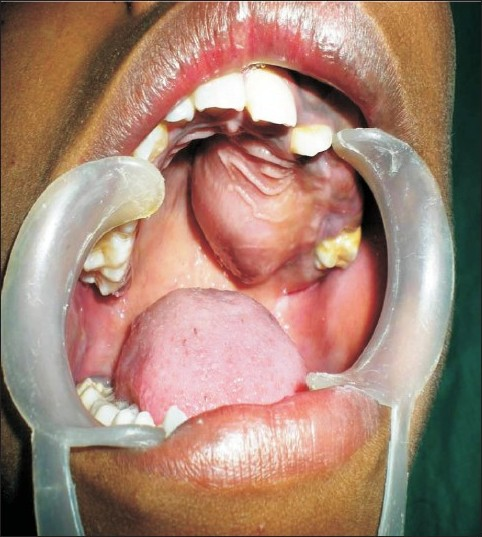
- Inside of the mouth shows intraoral swelling in the region of the palate, labial, and buccal sulcus region.
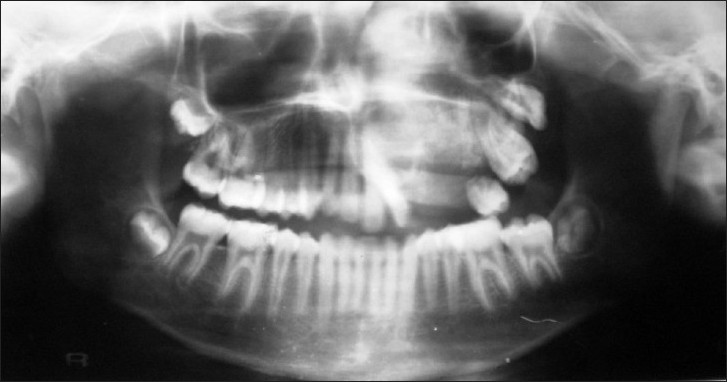
- Panoramic radiograph of the patient shows radiopacity and displacement of teeth.
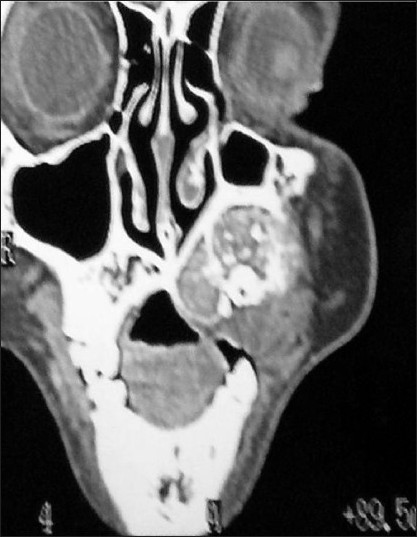
- Coronal CT shows obliteration of left maxillary sinus and displacement of teeth.
DISCUSSION
Fibrous dysplasia is a developmental or growth disorder in which normal bone is replaced by abnormal fibrous tissue that contains small, abnormally arranged bone trabeculae. It is considered by some authors to be a hamartomatous malformation that presumably results from an idiopathic arrest in maturation of bone at the woven bone stage.[12] Craniofacial involvement in fibrous dysplasia is seen in both monostotic and polyostotic forms. Monostotic fibrous dysplasia has a different skeletal distribution from polyostotic disease and occurs most commonly in the femur, followed by occurrences in the tibia, craniofacial bones, and the ribs.[23] Craniofacial involvement occurs in about 30% of monostotic fibrous dysplasia and typically affects the maxilla, mandible, and rarely, the calvarium. Polyostotic form of the disease has nearly 100% involvement of the craniofacial bones.[3] Clinical presentation of fibrous dysplasia varies with the primary bone involved and the extent of disease. Fibrous dysplasia has its onset during early life, usually in late childhood or early adolescence. Patients with polyostotic form of disease are considerably younger. There is an equal distribution in monostotic fibrous dysplasia among the sexes, but the polyostotic form has a clear female predilection.[3] Radiographic features of fibrous dysplasia vary depending on the amount of bony and fibrous matrix within the lesion and have been sub-classified into three different patterns: pagetoid type 56%, sclerotic type 23%, and the radiolucent type 21%.[3] Both the patients had sclerotic lesions, the commonest form of involvement seen in facial bones and bones of the base of the skull. The lytic and pagetoid types usually involve the calvarial bones. Radionuclide scanning in fibrous dysplasia shows areas of intensely increased uptake that is due to diffuse microscopic ossification. Scintigraphy is helpful in determining the activity and potential multicentricity of the lesion and is specifically helpful in diagnosing when plain radiographs are equivocal.[3] CT accurately establishes the diagnosis and extent of bone involvement. Involvement of optic canals, orbital fissures, frontonasal ducts, and ostiomeatal complex can be best evaluated by CT scanning. CT characteristics of fibrous dysplasia include expansion of the involved bone with heterogenous pattern of CT densities associated with scattered or confluent islands of bone formation. CT attenuation levels have been reported to range from 34 to 513 Hounsfield (HU) depending on the fibrous tissue and bone content.[3] On magnetic resonance imaging (MRI), fibrous dysplasia exhibits homogenous and moderately low signal intensity on T1-weighted images. On T2-weighted images, the tissue usually exhibits very high signal intensity. After intravenous Gd-diethylenetriaminepentaacetate (Gd-DTPA) lesions display moderate to significant central contrast enhancement with some rim enhancement. The degree of contrast enhancement on T1-weighted images depends on the amount and degree of bone trabeculae and collagen present. Both CT and MRI are excellent imaging modalities in defining the constrictive effect of craniofacial fibrous dysplasia on the orbit, optic canals, and adjacent paranasal sinuses.[4]
JOF is an uncommon, benign, bone-forming neoplasm that is distinguished from other fibro-osseous lesions primarily by its age of onset, clinical presentation, and potential behavior. This lesion most often occurs between 5 and 15 years of age, shows a male predilection,[56] and may exhibit rapid growth of the involved anatomic site, sometimes resulting in considerable facial disfigurement. Most juvenile ossifying fibromas arise in the vicinity of the paranasal sinuses. With regard to the incidence of JOF in the jaws, there are conflicting reports of maxillary and mandibular predilections. A recent study by El-Mofty identified two histopathological variants, trabecular JOF (TrJOF) and psamamatoid JOF (PsJOF). One clinical feature that helps differentiate TrJOF from PsJOF is the site of involvement, with TrJOF occurring mainly in the maxilla and PsJOF occurring mainly in the paranasal sinuses.[67] JOF may present clinically as either a gradual or rapid, painless expansion of the affected bone or region. The main characteristics are the location of the tumor, the radiologic pattern, and tendency to recur. JOF is often seen in very young children. In reviews published by Hamner et al., and Slootweg et al., the mean ages of onset were 11.5 and 11.8 years, respectively.[89] Clinically, this lesion has in general a more aggressive growth rate than ossifying fibroma. Most cases of maxillary JOF are asymptomatic, as was the present case.
Nasal obstruction, exophthalmos, and rarely, intracranial extension can be associated with those lesions arising within the paranasal sinuses and orbit.[8] Radiographic features are non-specific and depending on the location of the tumor, maturation stage, and stage of ossification, they are uni- or multi-locular well-defined lesions that may be radiolucent, mixed, or radio-opaque. Aggressive lesions may show cortical thinning and perforation.[8] The most frequent location of JOF is in the paranasal sinuses, accounting for about 90% of cases, whereas mandibular lesions account for approximately 10% of the facial JOF cases.[9] In general, JOF has a more aggressive growth pattern than the adult variant of ossifying fibroma. They are usually asymptomatic, exhibit rapid growth of the involved site, and the first presentation will be a clinically obvious swelling. All the above features were seen in our case.
Other less common fibro-osseous lesions include focal sclerosing osteomyelitis, florid osseous dysplasias periapical cemento-osseous dysplasia, and osteitis deformans.
Focal sclerosing osteomyelitis is a lesion characterized by growth of peri-radicular bone. The bone growth is caused by mild infection of dental pulp. Radiographically it appears as a uniform dense radiopaque mass adjacent to the apex of the tooth, with well-defined margins and vague transition to the surrounding bone combined with apical loss of lamina dura and widening of periodontal ligament space.[10]
Florid osseous dysplasias are a group of disorders known to originate from periodontal ligament tissues and involve, essentially, the same pathological process. Radiographically, the lesions appear as multiple sclerotic masses, located in two or more quadrants, usually in the tooth-bearing regions. They are often confined within the alveolar bone.[10]
Periapical cemento-osseous dysplasia predominantly involves the periapical region of the anterior mandible. Early lesions appear as circumscribed areas of radiolucency involving the apical area of a tooth. With time, adjacent lesions often fuse to form a linear pattern of radiolucency that envelopes the apices of several teeth. In the end stage, the lesions show a circumscribed dense calcification surrounded by narrow radiolucent rim.[10]
Paget's disease or osteitis deformans is a disease characterized by abnormal and anarchic resorption and deposition of bone, resulting in distortion and weakening of the affected bones. Radiographically, the early stages of Paget's disease reveal a decreased radiodensity of the bone and alteration of the bone. Particularly in the skull, large circumscribed areas of radiolucency may be present (osteoporosis circumscripta). During the osteoblastic phase of the disease, patchy areas of sclerotic bone are formed, which tend to become confluent. The patchy sclerotic areas are often described as having a “cotton wool” appearance.[10]
The rapid growth rate often exhibited by these lesions can be quite alarming and cause the clinician to suspect the presence of a malignancy. It is therefore important to maintain active communication between surgeon, radiologist, and pathologist to establish the benign nature of the lesion and prevent overtreatment.
Source of Support: Nil
Conflict of Interest: None declared.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp? 2011/1/10/76688
REFERENCES
- Fibro-osseous lesions of craniofacial bones: The role of imaging. Radiol Clin North Am. 1993;31:121-34.
- [Google Scholar]
- Craniofacial polyostotic fibrous dysplasia: A case report and review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;106:e49-55.
- [Google Scholar]
- Juvenile ossifying fibroma: Report of four cases. J Cranio Maxillofac Surg. 1990;18:125-9.
- [Google Scholar]
- Psammomatoid and trabecular juvenile ossifying fibroma of the craniofacial skeleton: Two distinct clinicopathologic entities. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2002;93:296-304.
- [Google Scholar]
- Benign fibro-osseous jaw lesions of periodontal membrane origin: An analysis of 249 cases. Cancer. 1968;22:861-78.
- [Google Scholar]
- Maxillofacial fibro-osseous lesions: Classification and differential diagnosis. Semin Diagn Pathol. 1996;13:104-112.
- [Google Scholar]
- Bone pathology. In: Neville, ed. Oral and Maxillofacial pathology (2nd ed). New Delhi: Elsevier; 2005. p. :533-87.
- [Google Scholar]






