Translate this page into:
Benign Medullary Fibroma of the Kidney: A Rare Diagnostic Dilemma
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Renomedullary interstitial cell tumor or medullary fibroma, is a small tumor that commonly presents as an incidental finding, but in rare cases maybe large and symptomatic. Although it is a benign tumor, it is difficult to differentiate this lesion from other malignancies of the kidney on radiological basis and hence many patients undergo radical nephrectomy. We present a case of renal medullary fibroma and various nuances associated with radiological identification of this lesion and its management related dilemmas.
Keywords
Benign
histopathology
imaging
renal cancer
renal medullary fibroma
INTRODUCTION

Clinically evident renal medullary fibroma is a rare occurrence. These lesions are usually small and escape clinical detection.[1] However, an 8 cm size lesion has been reported in the literature.[2] Benign fibromatous tumors have also been described to affect other urogenital sites such as testis and paratesticular soft-tissues.[3] Clinical diagnosis of this entity on imaging is usually difficult. Diagnosis depends on awareness of imaging and pathological features of this entity.
It is difficult to distinguish benign renal medullary fibroma from renal malignancy pre-operatively and most of these clinical scenarios end up in radical nephrectomy.
A 32-year-old male patient presented with left flank pain and a single episode of gross hematuria. There was no palpable abdominal mass. The radiologic features suggested renal carcinoma; however, after surgery and histopathology investigations the lesion was identified as renal fibroma.
RADIOLOGIC FEATURES
Computed tomography (CT) scan of the abdomen revealed a calcified, partially exophytic soft-tissue mass involving the mid and interpolar regions of the right kidney [Figure 1]. Contrast enhanced CT revealed doubtful enhancement with perirenal mild inflammatory stranding [Figure 2]. There were no calculi either in the kidney or the ureter. There was no evidence of renal vein or venacaval extension and no obvious lymphadenopathy. The contra-lateral kidney was normal. Right renal cell carcinoma (RCC) was suspected and patient underwent laparoscopic right radical nephrectomy.
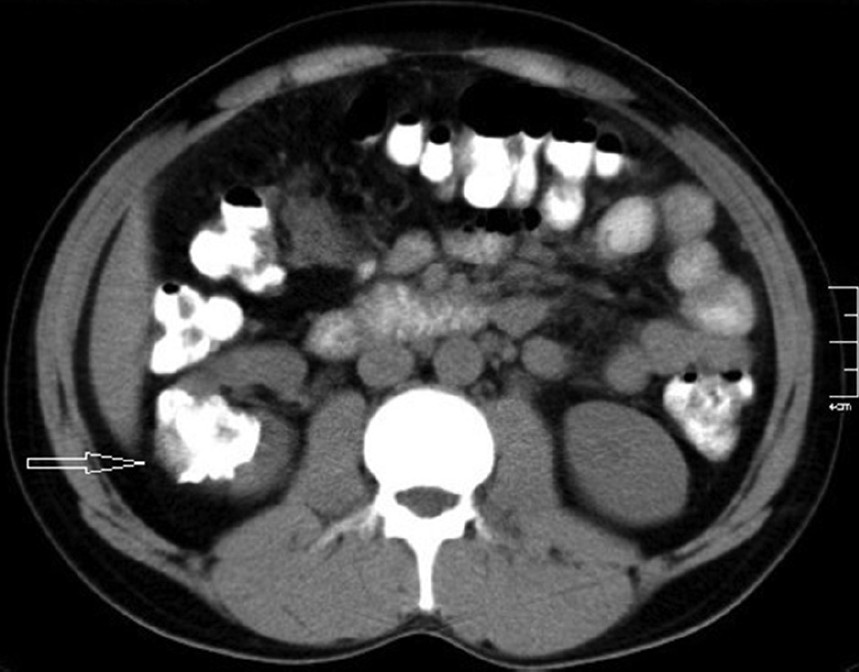
- 32-year-old male with left flank pain and gross hematuria diagnosed with renal medullary fibroma. Unenhanced computed tomography scan of the abdomen reveals a calcified, partially exophytic soft-tissue mass (arrow) involving the mid and interpolar regions of the right kidney.
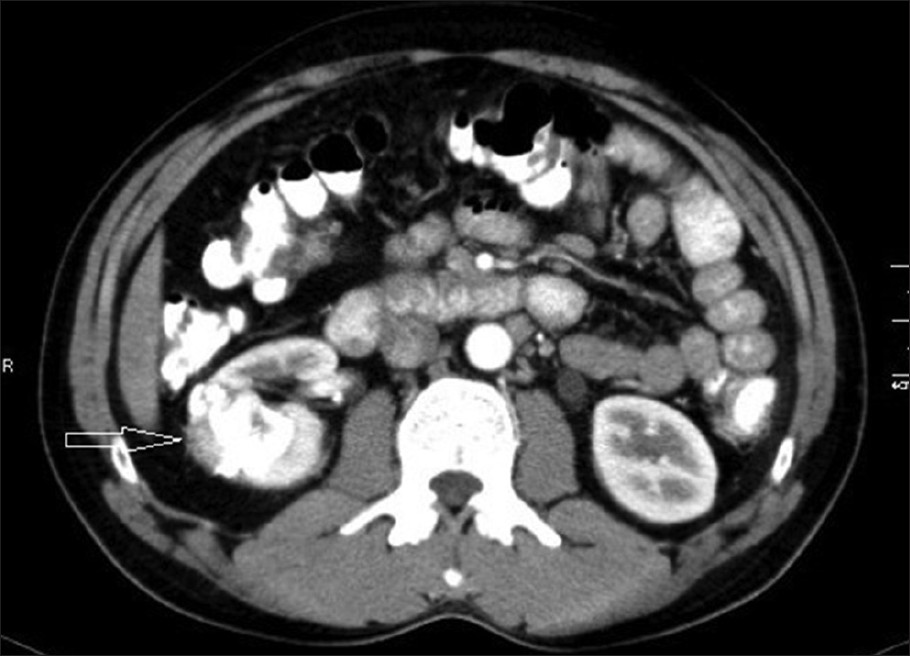
- 32-year-old male with left flank pain and gross hematuria diagnosed with renal medullary fibroma. Contrast enhanced computed tomography reveals doubtful enhancement around the calcified partially exophytic mass with perirenal mild inflammatory stranding (arrow).
PATHOLOGIC FEATURES
On cut section, the right kidney contained a well-circumscribed 4 cm × 4 cm, grayish-yellow tumor with areas of calcification [Figure 3]. The tumor was extending close to the pelvicalyceal system. Rest of the renal parenchyma was normal. Renal vessels and the ureter were free of tumor.

- 32-year-old male with left flank pain and gross hematuria diagnosed with renal medullary fibroma. Gross photograph shows a firm grayish yellow calcified tumor (black arrow), renal hilum (white arrow).
Histological analysis revealed an unencapsulated, paucicellular tumor with large areas of hyalinization, fibrosis and variable infiltrate consisting of lymphocytes and plasma cells. Scattered among the sclerotic stroma a few spindle cells in myxoid background with prominent nucleoli were observed. Thick collagen bundles with psammomatous and dystrophic calcification with osteoid formation were also noted [Figures 4 and 5].
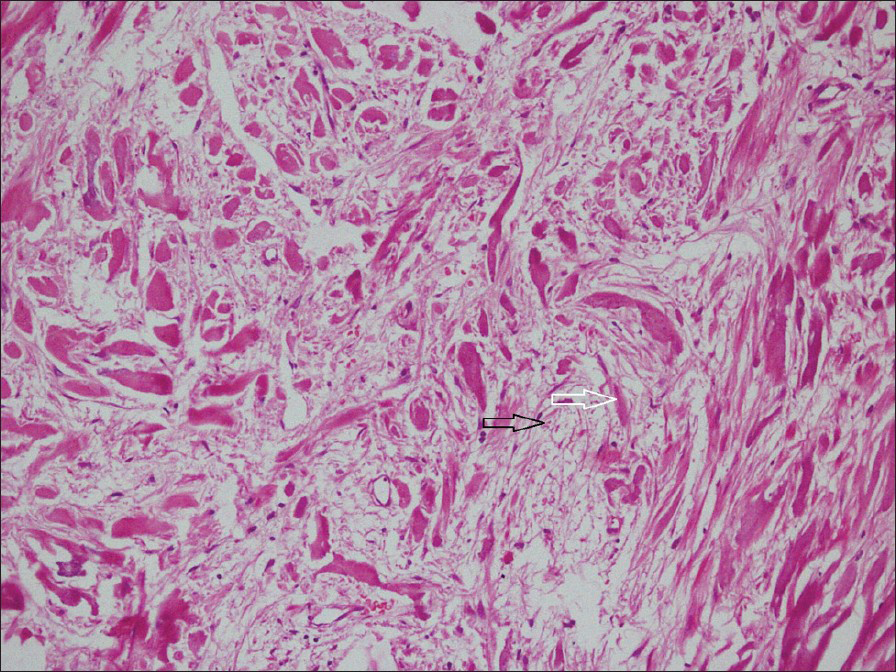
- 32-year-old male with left flank pain and gross hematuria diagnosed with renal medullary fibroma. Photomicrograph of hematoxylin and eosin, stained tissue (×100) shows bland spindle-shaped cells occurring singly within a loose stromal matrix (black arrow) and separated by thick collagen bundles (white arrow).
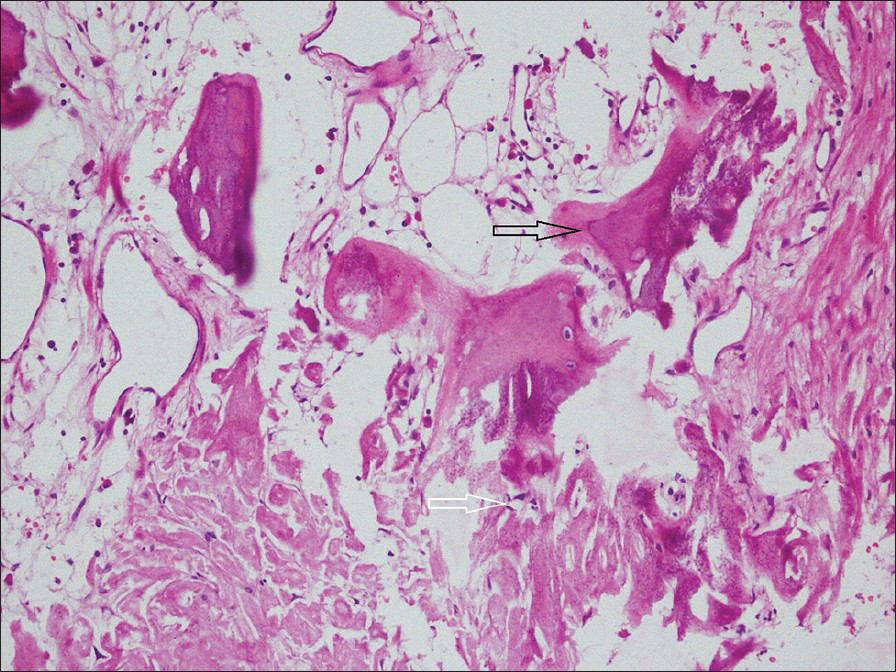
- 32-year-old male with left flank pain and gross hematuria diagnosed with renal medullary fibroma. Photomicrograph of H and E stained tissue (×100) shows foci of thick collagen bundles with calcification (white arrow) and osseous metaplasia (black arrow).
Convalescence was uneventful and the patient was discharged on the 3rd day post-operation.
DISCUSSION
Renomedullary fibromas are very common benign tumors arising from the interstitial cells of the renal medulla and commonly present as an incidental finding. The lesion localizes in the renal medulla and almost always measures less than 0.5 cm in diameter although tumors up to 8 cm have been reported. They are unencapsulated, but well-defined nodules that are usually solitary, but may sometime be multiple and bilateral. Prevalence increases with age and has an equal sex distribution. More than 50% of patients are older than 20 years of age. Few renal medullary fibromas are large enough to become clinically evident and cause symptoms due to torsion of the tumor about a pedicle causing venous stasis, infarction, vascular rupture, and subsequent hematuria.[4] Pre-operative diagnosis of renal medullary fibroma is difficult and the radiological spectrum of calcifications on plain X-rays, echogenicity on CT, neovascularity on arteriogram and filling defects on retrograde pyelogram, all simulate either renal cell carcinoma (RCC or transitional cell carcinoma. On ultrasonography, renal medullary fibroma is seen as an echogenic mass. On CT scan, a predominantly soft-tissue attenuation tumor with lack of hemorrhage and necrosis should draw attention toward this differential diagnosis. As such it needs to be differentiated from other calcified renal lesions. Osteosarcoma of the kidney is a rare tumor, which generally presents as a large mass with dense chunky calcification and may even replace whole of the kidney. Xantho-granulomatous pyelonephritis also present as a heterogenous non-enhancing mass and a staghorn calculus is present in 80% of the cases. The kidney is enlarged with paradoxically contracted renal pelvis with dilated calyces giving the appearance of the paw-print of a bear (bear paw sign). Magnetic resonance imaging (MRI) evaluation for renal medullary fibroma can be helpful. On MRI, renal medullary fibroma shows low signal intensity in both T1- and T2-weighted images presumably because of their dense collagen content and little cellularity[56] Malignant fibrous histiocytoma is yet another densely collagenous, but malignant tumor, which shows low intensity in T2 images. RCC on the other hand have an intensity intermediate between renal cortex and medulla on T1-weighted image and are isointense or hyperintense relative to normal parenchyma on T2-weighted image. Because it is unusual for RCC to have low signal intensity on both T1- and T2-weighted images, renal medullary fibroma should be considered in the differential diagnosis. Hematomas can also can have low signal intensity on both T1- and T2-weighted images especially when their hemosiderin content is substantial. Inflammatory pseudotumor is another rare lesion, which presents as hypointense lesion on T1- and T2-weighted images due to fibrotic changes and shows delayed gadolinium enhancement due to the accumulation of extravascular contrast media in the fibrotic component of the mass. Contrast enhanced CT picture is highly variable and may show homo- or heterogeneity and hypo-, iso-, or hyperdensity.[789] Renal leiomyoma may be considered in the differential diagnosis since renal leiomyoma manifests with homogenous soft-tissue density on CT and low signal intensity on T1- and T2-weighted images.
These patients usually undergo radical nephrectomy as malignancy cannot be ruled out with certainty. However, these entities are entirely benign and patients have an excellent prognosis and thus there may be a role for biopsy if this lesion is suspected radiologically. Role of positron emission tomography (PET) scan in renal masses is yet not clearly defined. In general, benign tumors are photopenic and malignant tumors shows fluorodeoxyglucose avidity, but exception has been reported.[10] MRI and PET scan evaluation of these clinical scenarios can prevent unnecessary removal of normal renal parenchymal tissue. Prudent use of the available modalities of imaging can help us in deciding to perform nephron sparing surgeries in these cases. Radiologists and clinicians need to be aware of the possibility of these kinds of lesions that warrant further evaluation.
CONCLUSION
Medullary fibroma is a very frequent small tumor that most commonly presents as an incidental finding, but in rare cases maybe large and symptomatic. These patients usually undergo radical nephrectomy as malignancy cannot be ruled out with certainty. However, these entities are entirely benign and patients have an excellent prognosis and thus there may be a role for biopsy if this lesion is suspected radiologically with available modalities including MRI. Role of PET scan in renal masses is not yet clearly defined.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2013/3/1/43/120776
Source of Support: Nil
Conflict of Interest: None declared.
REFERENCES
- Renomedullary interstitial cell tumor. In: Atlas of Tumor Pathology. Washington D.C: Armed Forces Institute of Pathology; 1975. p. :231.
- [Google Scholar]
- Benign fibromatous tumor (fibroma) of the kidney: A case report. Pathol Res Pract. 1998;194:123-7.
- [Google Scholar]
- Benign fibromatous tumors of the testis and paratesticular region: A report of 9 cases with a proposed classification of fibromatous tumors and tumor-like lesions. Am J Surg Pathol. 1997;21:296-305.
- [Google Scholar]
- MR imaging findings in renal medullary fibroma. AJR Am J Roentgenol. 1989;153:83-4.
- [Google Scholar]
- Mesenchymal neoplasms of the kidney in adults: Imaging spectrum with radiologic-pathologic correlation. Radiographics. 2010;30:1525-40.
- [Google Scholar]
- Diagnosis and staging of renal cell carcinoma: A comparison of MR imaging and CT. AJR Am J Roentgenol. 1987;148:749-53.
- [Google Scholar]
- Magnetic resonance imaging in the diagnosis and staging of renal and perirenal neoplasms. Radiology. 1985;154:709-15.
- [Google Scholar]
- Detection and staging of renal neoplasms: A reassessment of MR imaging. Radiology. 1988;166:643-9.
- [Google Scholar]
- Role of FDG PET/CT in imaging of renal lesions. J Med Imaging Radiat Oncol. 2010;54:347-57.
- [Google Scholar]






