Translate this page into:
Assessment of the Inferior Petrosal Sinus on T1-Weighted Contrast-Enhanced Magnetic Resonance Imaging
-
Received: ,
Accepted: ,
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Context:
Skull base venous anatomy.
Aims:
While prior studies have focused on the efficacy of conventional fluoroscopic venography and multidetector computed tomography venography to evaluate the inferior petrosal sinus (IPS) before image-guided intervention (such as dural venous sinus sampling), we believe that routine magnetic resonance imaging (MRI) may provide reliable structural information helpful for planning without the need for further imaging.
Settings and Design:
Retrospective review of brain MRI.
Materials and Methods:
Retrospective analysis was carried out on IPSs on contrast-enhanced T1-weighted MR images. Qualitative measurements were made regarding the grade of patency of the IPS, variation in IPS drainage pattern, and grading of the ipsilateral transverse and sigmoid sinuses (TS and SS).
Statistical Analysis Used:
Pearson's product-moment correlation.
Results:
Evaluation of a total of 148 IPSs revealed that 91% of cases were grade 3 or grade 2 (either fully or mostly visualized), with 65% of cases demonstrating “typical” (type A) drainage directly into the internal jugular vein and no statistically significant correlation between the patency of the IPS and the dominance of the ipsilateral TS/SS. A bilateral concordance rate of 77% was also observed.
Conclusions:
Our analysis indicates that routine thin-slice contrast-enhanced T1-weighted MRI can provide sufficient anatomic detail to identify typical drainage pattern of the IPS in a majority of cases. In cases where routine drainage was not identified, spatial resolution was not sufficient to further delineate complex drainage anatomy. No correlation was observed between the TS/SS dominance and patency of the ipsilateral IPS.
Keywords
Brain
dural venous sinuses
inferior petrosal sinus
magnetic resonance imaging
skull base
veins

INTRODUCTION
The inferior petrosal sinus (IPS) is one of the several paired dural venous sinuses that function to drain venous blood from the cavernous sinus. Beginning at the cavernous sinus bilaterally, the left and right IPSs course along a narrow groove between the petrous part of the temporal bone and the basilar region of the occipital bone until it empties into the jugular bulb (JB) of the internal jugular vein (IJV). In addition to receiving venous blood from the cavernous sinus, the medulla, pons, inferior cerebellum, and pituitary gland also have some degree of drainage into the IPS. Anatomical variations at the junction of the IPS and IJV have previously been classified using high-resolution computed tomography (CT) and cavernous sinus venography, but magnetic resonance imaging (MRI) has never before been used to characterize variations at the IPS–IJV junction. A priori knowledge of anatomical variants in this region may be helpful to facilitate particular venous neurointerventions, such as inferior petrosal venous sampling in the evaluation of Cushing's syndrome, and in transvenous embolization of dural arteriovenous fistulas that necessitate access through the IPS, and to avoid misinterpretation of normal anatomy in the evaluation of other pathologies. The purpose of this study is as follows:
-
Can the IPS be consistently and reliably visualized on standard contrast-enhanced (nonangiographic) MRI?
-
Can variant anatomy of the IPS be visualized on MRI?
-
Does dominance of the ipsilateral transverse sinus/sigmoid sinus (TS/SS) indicate anything about the anatomy about the IPS?
MATERIALS AND METHODS
A random collection of 100 postcontrast MRI brain studies was queried from the Picture archiving and communication system. Resultant studies ranged in date from January 2015 through August 2015. Studies were then initially reviewed by two authors (a radiology resident and a medical student) and were each reviewed by a second author (neuroradiology faculty member). All imaging was performed on either a 1.5 T or 3.0 T MR scanner with the administration of 15–20 mL of Multihance contrast (gadobenate dimeglumine, a gadolinium-based contrast agent) with imaging performed approximately 60 s after injection, including T1-weighted postcontrast SPACE (spin echo) sequences. The studies were reviewed for quality and were discarded if they contained images with prohibitive motion artifact, slice thickness >1 mm, or with incomplete postcontrast imaging (specifically with an absent axial postcontrast sequence). In addition, studies with imaging demonstrating pathologic states (excluding incidental and clinically insignificant findings) were excluded. Assessment of the visibility of each of the IPSs was made qualitatively, with categories of entirely nonvisualized (grade 0), partially visualized (grade 1), and mostly or entirely visualized throughout its course (grade 2). Assessment of the anatomic course of each IPS was also assessed to be either normal in course along the medial aspect of the petrous ridge with eventual emptying into the JB (type A) or with aberrant course with entry into the bony petrous ridge with an intratemporal course before rejoining the IJV at or immediately inferior to the JB (type B).
Concurrently, a qualitative assessment was made regarding the dominance of the ipsilateral dural venous TS and SS. If the ipsilateral sinuses were entirely nonvisualized or aplastic, a grade of 0 was given; if they were hypoplastic in relation to the contralateral side, a grade of 1 was given; if they were approximately equal in size bilaterally, a grade of 2 was given to that side; if they were dominant in size compared to the contralateral side, a grade of 3 was given; and if they were dominant to the exclusion of any visible counterpart TS/SS on the contralateral size, they were given a grade of 4 [Figure 1].
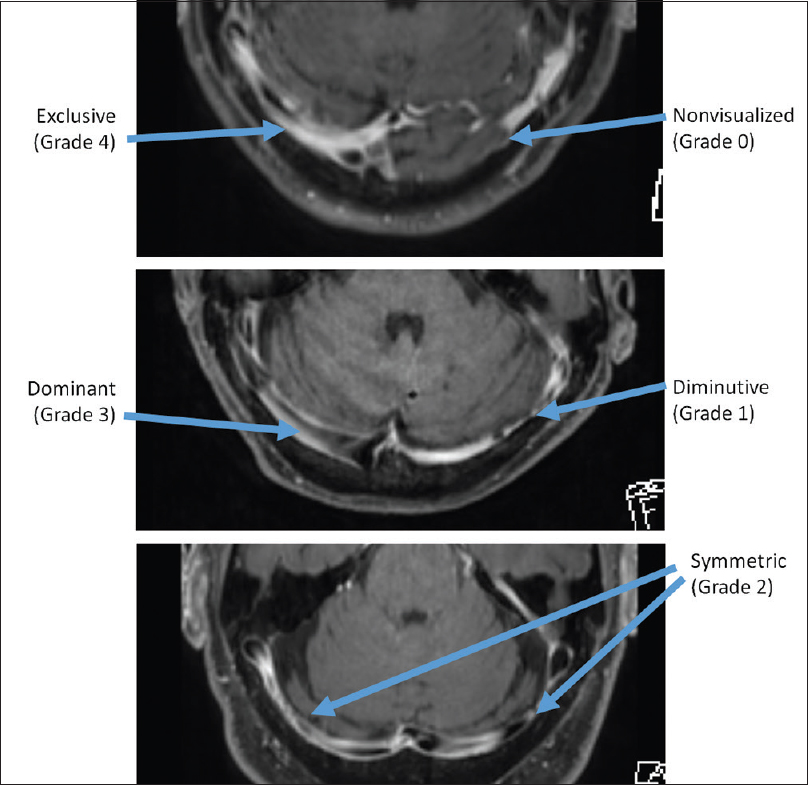
- Grading system used for the transverse and sigmoid sinuses, to assess correlation with ipsilateral inferior petrosal sinus grade.
RESULTS
A total of 100 postcontrast axial T1-weighted sequences of the brain were acquired. After exclusion criteria were applied, a total of 74 studies remained with usable images, resulting in a total analysis of 148 IPSs (74 left and 74 right). The male: female gender ratio is approximately 2.4 (52 males and 22 females), and the median age is 53 years old (range of 17–91) [Table 1].

With regard to visibility of the IPS, approximately 9% (14 total out of 148) cases received a grading of 0 (nonvisible), while 40% (59) received a grade of 1 (partially visible) and 51% (75) received a grade of 2 (mostly or completely visible) [Table 2]. Regarding anatomical variance, approximately 65% (87 out of 134) cases were type A and 35% (47) were type B. In cases where the IPS was incompletely visualized (type 1), the region of the sinus poorly visualized was nearly always either the proximal segment of the sinus (at the level of the cavernous sinus) or mid-distal segments (as it courses over/through the petrous ridge). The terminus of the IPS was always visualized at the level of the JB, either coursing over (type A) or emerging from the temporal bone (type B).
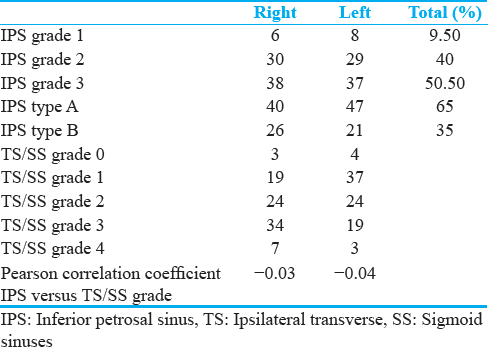
When assessing the dominance of the TS and SS on the side of interest, approximately 4% (7 out of 174) received a score of 0, 32% received a score of 1, 28% received a score of 2, 30% received a score of 3, and 6% received a score of 4.
Of the usable 74 pairs of IPSs evaluated, 57 were found to have symmetric IPS grades (bilateral concordance rate of 77%).
To evaluate the correlation between the grade of the IPS and its correspondence to the grade of the ipsilateral TS/SS, the Pearson's product-moment correlation coefficient was calculated for each side (74 left side and and 74 right side). No statistically significant correlation was determined (r = −0.03 on the right side [95% confidence interval: 0.27–0.20], r = −0.04 on the left side [95% confidence interval of 0.28–0.19]).
DISCUSSION
Comparing gradients of peripherally obtained venous adrenocorticotropic hormone (ACTH) levels with levels obtained from central venous blood from the IJV has been described as far back the 1960s, with subsequent sampling of the IPS sampling and attempts at establishing utility in lateralization following thereafter in the 1970s.[1] In the setting of sustained ACTH-dependent Cushing's syndrome, IPS remains a reliable means of diagnosing and lateralizing primary ACTH-secreting pituitary adenomas.[2]
While, to our knowledge, no large studies have been done to investigate the most commonly employed strategies used by interventional neuroradiologists to evaluate skull base venous anatomy, in our clinical experience, the most common strategies involve either primary investigation of the vascular anatomy in vivo in the angiography suite or review of high-resolution CT angiography/venography performed prior to the procedure.
The former strategy is often time and cost effective in the setting of many common procedures that do not require superselective catheterization such as diagnostic cerebral angiography; where anatomic variants are discovered in these instances, redirection of the catheter to a more appropriate location is done ad lib and with minimal consequences. However, in certain protocols that require superselective catheterization and sampling from specifc drainage sites, such as the IPS for the evaluation of Cushing’ s disease or for transvenous access for embolization of dural arteriovenous fstulas, anatomic variants (or in some cases complete absence) of this structure dramatically affects the ability for the procedure to be accomplished. In some cases, this may necessitate the abortion of the procedure itself, with wasted resources including angiographic suite time, sterile catheter hardware, anesthesia, anticoagulants, and the added stress to the patient having to undergo the process of preparing for the procedure (including stopping their antisteroidogenic medications such as metyrapone or ketoconazole).[3]
In the second case, the use of CT angiography/venography may avoid some of the problems mentioned above, but introduce new disadvantages. Iodinated intravenous contrast administration, although generally considered to be safe, is associated with low-frequency risks which may predicate the consideration of alternatives [Figure 2].
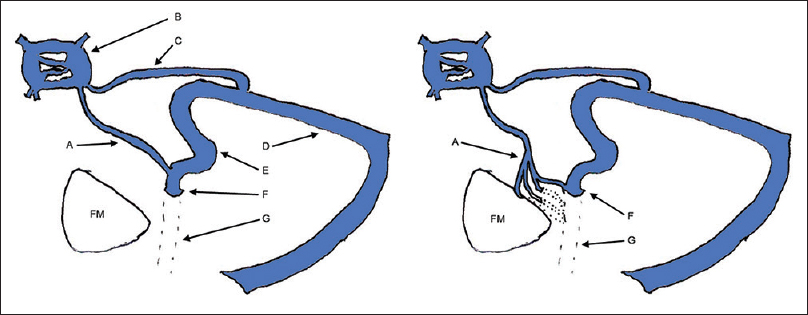
- Typical (left) and atypical (right) drainage patterns of the inferior petrosal sinus. (A) Inferior petrosal sinus. (B) Cavernous sinus. (C) Superior petrosal sinus. (D) Transverse sinus. (E) Sigmoid sinus. (F) Jugular bulb. (G) Internal jugular vein. FM: Foramen magnum.
In one of the earliest attempts to identify the complex anatomy of the IPS drainage, Shiu et al. described four drainage patterns, with the typical drainage of the IPS directly into the JB to be present in 45% of cases (n = 57).[4] A subsequent prospective attempt by Miller et al. to evaluate IPS anatomy on venography further described the relationship between the IPS and the vertebral venous plexus, which at that time had already been identified as a possible drainage pattern.[5] Their study revealed that 56.1% of IPS were of the “typical” drainage pattern, draining directly into the IJV with either a small (9.8%) or large (>5 Fr, 46.3%) anastomosis with the vertebral venous plexus; further characterization of this IPS–IJV drainage as being at the level of or below the JB was not done. In this report, symmetry of IPS drainage was seen 65% of the time. Mitsuhashi et al., performed independent investigation of IPS sampling through the use of 3-dimensional rotational venography, with their analysis revealing observable drainage of the IPS into the IJV in 73.4% of cases, although only 36.1% of cases showed this drainage to occur at or above the level of the hypoglossal canal; the remaining cases were either to the lower extracranial IJV or through various plexiform connections (or described absence of the IPS altogether).[6] Three years later, a study published by Tanoue et al. described the evaluation of the craniocervical venous structures through the use of thin-slice (0.5 mm or 1 mm axial-slice thickness) CT venography.[7] While their results describe approximately 92% of IPS demonstrating “typical” drainage into the JB, they go on to state that their “cases could not be evaluated with regard to connection pattern by MDCT,” suggesting that CT venography lacked the spatial resolution to evaluate the various complex and plexiform anatomic configurations of IPS drainage.
Although attempts have been made to use MR images to assess the venous structures of the craniocervical junction, the IPS was not addressed.[89] Our work represents an attempt to evaluate the morphology of the IPS on routine contrast-enhanced MRI.
Our results indicate that up to 91% of IPSs were either mostly or entirely visualized on routine, contrast-enhanced axial T1-weighted MR images, indicating that the presence/patency of the sinus at the least can be identified on routine MR alone [Figure 2]. Furthermore, in our study, up to 65% of IPSs were identified to be “usual” anatomy, that is, with clearly discernable drainage directly into the JB. These findings suggest that a close review of contrast-enhanced MRI in patients being evaluated for IPS sampling may provide an acceptable level of confidence regarding patency of the IPS–IJV anastomosis without the use of supplementary venographic studies which carry the associated risks of radiation and iodinated contrast administration [Figure 3].
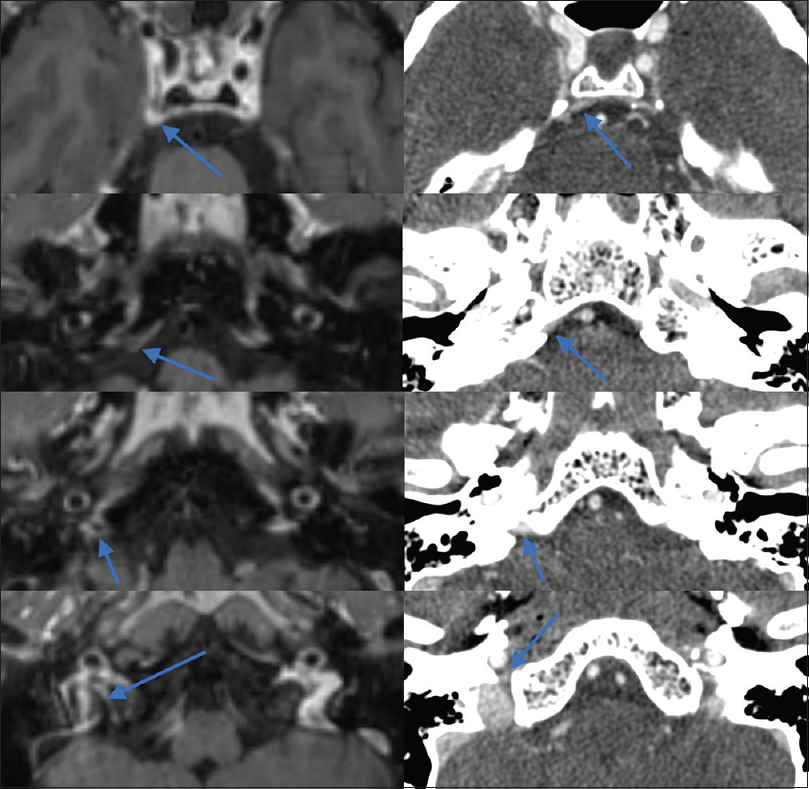
- Appearance of a grade 2 (fully visualized) right inferior petrosal sinus with drainage pattern of type A in the same patient on both contrast-enhanced T1-weighted magnetic resonance imaging (left) and computed tomography venography (right).
Conversely, in the 35% of cases where the “usual” drainage configuration was not identified, the exact anatomic variant of IPS drainage was not discernable, leaving in question which specific drainage pattern was at hand, such as into the anterior condylar vein and vertebral venous plexus, among myriad other possibilities [Figure 3]. In cases where contrast-enhanced MRI reveals lack of a typical drainage configuration, further investigation with fluoroscopic venography may be the only way to identify precise anatomy, such as for patients with indirect drainage of the IPS directly into the ACv in whom an ipsilateral IJV approach for superselective catheterization of the IPS would be difficult [Figure 4].[8]
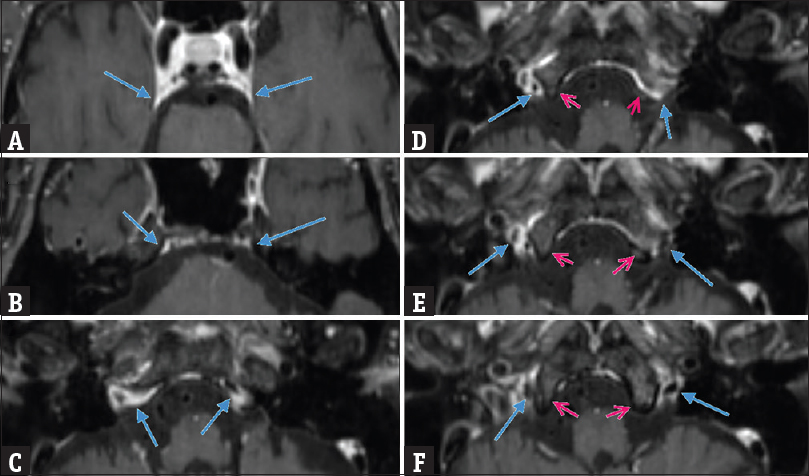
- Asymmetrical bilateral inferior petrosal sinuses as they course from the cavernous sinus to the skull base (A through F). The right inferior petrosal sinus demonstrates type A drainage, while the left inferior petrosal sinus demonstrates type B drainage. Frames D and E show the left inferior petrosal sinus (blue arrow) passing through the bony clivus (red arrow) rather than draining directly into the jugular bulb
Prior studies have suggested that the concordance rate between the IPS on each side is 65% (with the remaining 35% demonstrating asymmetric configuration).[8] Our study revealed concordance in IPS caliber in 77% of cases. Furthermore, suggestions made previously in the literature that dominance of the TS/SS may hold information regarding dominance of the IPS were not borne out in our study. Dominance of the TS/SS was not statistically correlated to the grade of the ipsilateral IPS.
CONCLUSIONS
Given the frequency of anatomic variety in the venous drainage system of the skull base, and given the high likelihood of clinically significant changes in approach for studies involving a skull base venous approach (such as unilateral IPS sampling or embolization of dural arteriovenous fistulas), preprocedural evaluation of the vasculature can be crucial. While informal review of current practices suggests frequent use of CT or MR angiography/venography in pursuit of such evaluation, our study demonstrates that in up to 91% of cases the IPS can be either mostly or entirely visualized on routine contrast-enhanced MRI. Future research may focus on prospective studies aimed at determining precise specificity and sensitivity of MRI in relation to other modalities where a typical drainage configuration is successfully identified. Although the general course and patency of the IPS can be evaluated in these cases, in our opinion, the spatial resolution of routine contrast-enhanced MRI was lacking for evaluation of complex IPS drainage patterns, similar to limitations described for CT venography by Tanoue et al., fluoroscopic venography remains the mainstay for evaluation of complex drainage. Furthermore, evaluation of the dominance of the TS/SS was demonstrated in our study not to be a statistically significant predictor of the dominance/patency of the ipsilateral IPS.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2018/8/1/22/234657.
REFERENCES
- Preoperative lateralization of ACTH-secreting pituitary microadenomas by bilateral and simultaneous inferior petrosal venous sinus sampling. N Engl J Med. 1985;312:100-3.
- [Google Scholar]
- The diagnosis and differential diagnosis of Cushing's syndrome and pseudo-Cushing's states. Endocr Rev. 1998;19:647-72.
- [Google Scholar]
- Anatomy of the junction of the inferior petrosal sinus and the internal jugular vein. AJNR Am J Neuroradiol. 1993;14:1075-83.
- [Google Scholar]
- Morphologic evaluation of the caudal end of the inferior petrosal sinus using 3D rotational venography. AJNR Am J Neuroradiol. 2007;28:1179-84.
- [Google Scholar]
- Venous structures at the craniocervical junction: Anatomical variations evaluated by multidetector row CT. Br J Radiol. 2010;83:831-40.
- [Google Scholar]
- Craniocervical junction venous anatomy around the suboccipital cavernous sinus: Evaluation by MR imaging. Eur Radiol. 2005;15:1694-700.
- [Google Scholar]
- Para-cavernous sinus venous structures: Anatomic variations and pathologic conditions evaluated on fat-suppressed 3D fast gradient-echo MR images. AJNR Am J Neuroradiol. 2006;27:1083-9.
- [Google Scholar]






