Translate this page into:
Round Ligament Varicosity Thrombosis Presenting as an Irreducible Inguinal Mass in a Postpartum Woman

*Corresponding author: Carol Ng, Department of Radiology, Princess Margaret Hospital, 2-10 Princess Margaret Hospital Road, Lai Chi Kok, Hong Kong. carol26@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Ng C, Wong GT. Round ligament varicosity thrombosis presenting as an irreducible inguinal mass in a postpartum woman. J Clin Imaging Sci 2019;9:28.
Abstract
Round ligament varicosities occur almost exclusively in pregnant and postpartum women and present similarly to inguinal hernias clinically, thus posing diagnostic challenges to clinicians. The distinction of the two conditions is important as round ligament varicosities do not require surgery while inguinal hernias do. Rarely, round ligament varicosites may be complicated by thrombosis or hemorrhage. In this case report, we present a rare case of round ligament varicosity (RLV) which has been complicated by thrombosis. The radiological features on ultrasound and contrast computed tomography of a thrombosed RLV are presented.
Keywords
Inguinal mass in pregnancy
Round ligament varicosity
Thrombosis of round ligament varicosity
INTRODUCTION
When presented with a groin mass that becomes larger on Valsalva maneuver, the first differential diagnosis to consider is inguinal hernia. However, a condition which is uncommon in the general population but more common than inguinal hernias in pregnant women called round ligament varicosity (RLV) can present similarly to inguinal hernias and pose diagnostic difficulties to the clinicians.[1] Inguinal hernias can be complicated by strangulation and bowel obstruction. RLVs can be complicated by thrombosis or hemorrhage. A thrombosed RLV presents similarly to a strangulated inguinal hernia with an irreducible, erythematous, tender groin mass. Strangulated inguinal hernias need urgent surgical treatment, while uncomplicated inguinal hernia can be managed by elective surgery. However, RLVs whether simple or complicated by thrombosis do not require surgery. Simple RLVs often undergo spontaneous resolution, while the thrombosed RLVs may require anticoagulation.
We present a case of a tender, erythemaotus groin mass in a postpartum woman, who was diagnosed to have thrombosed RLV. The radiological features on ultrasound and contrast-enhanced computed tomography (CT) of a thrombosed RLV will be discussed in detail. To our knowledge, there is only one case report with CT and MRI images of a thrombosed RLV in the English medical literature.[2]
CASE REPORT
A 35-year-old Chinese woman, G2P1, presented to the accident and emergency department complaining of a right groin swelling extending from the inguinal canal to the right vulva for 1 day. She delivered a healthy baby boy at 39 weeks 5 days gestation just 7 days ago by normal vaginal delivery. On examination, there was a longitudinal right groin mass ~8 cm with ill-defined borders. It was associated with erythema and tenderness. The mass was irreducible and cough impulse was absent. Clinicians were concerned about an incarcerated inguinal hernia. As the patient complaint of vague abdominal pain, a contrast CT abdomen and pelvis were ordered to exclude associated intestinal obstruction. The CT demonstrated a hyperdense, mildly enhancing serpentine tubular structure extending from the right adnexa into the inguinal canal and down to the right labia majora with surrounding fat stranding [Figure 1a-c]. Supplementary ultrasound was performed for correlation, which showed multiple hypoechoic serpentine structures with a “bag of worm appearance” in the right inguinal region [Figure 2a]. No flow signal was detected on color Doppler [Figure 2b]. The diameter of the hypoechoic serpentine structures remained unchanged in size and morphology with Valsalva maneuver and on erect/supine positioning. The lesion was non-compressible.
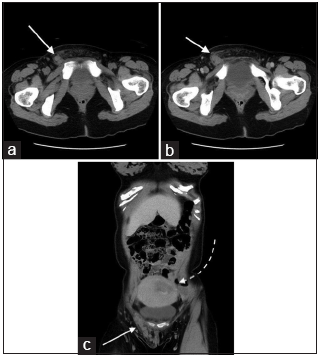
- A 35-year-old postpartum woman presenting with a right groin mass due to a thrombosed round ligament varicosity. (a) Axial non-contrast computed tomography (CT) scan of the pelvis at the groin level shows a hyperdense serpentine structure (white arrow), extending from the right deep inguinal ring along the inguinal canal to the labia majora compatible with a round ligament varicosity. Surrounding fat stranding is present due to thrombosis. (b) Axial contrast-enhanced CT scan of the pelvis at the groin level shows a lack of enhancement of the round ligament varicosity, supporting the presence of thrombosis. (white arrow). (c) Coronal contrast-enhanced CT again illustrates the thrombosed right round ligament varicosity in the right groin with better demonstration of its course in the inguinal canal (white solid arrow). The gravid uterus (white-dashed arrow) is seen.
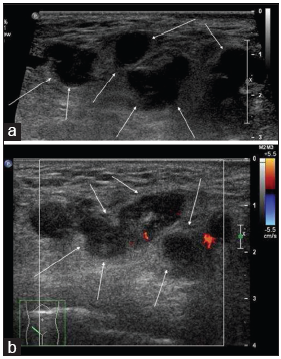
- A 35-year-old postpartum woman presenting with a right groin mass due to a thrombosed round ligament varicosity. (a) Grayscale USG of the right groin shows multiple hypoechoic serpentine structures (white arrows) in the subcutaneous layer with “a bag of worm” appearance, compatible with round ligament varicosity. (b) Corresponding color Doppler ultrasound of the right groin mass shows absence of Doppler signal within the vessels (white arrows) which suggest the presence of thrombosis.
Overall clinical and imaging features were consistent with right RLV. The lack of enhancement on CT and the absence of Doppler signal on USG suggested the complication of thrombosis.
The patient was given low molecular weight heparin 40 mg daily by subcutaneous injection for 6 weeks. Follow-up ultrasound showed resolution of the round ligament varicosities, and the veins showed a marked reduction in size. Reestablishment of flow signal within the residual veins suggested recanalization of the previously thrombosed veins [Figure 3]. Clinically, the patient’s groin swelling and erythema subsided.
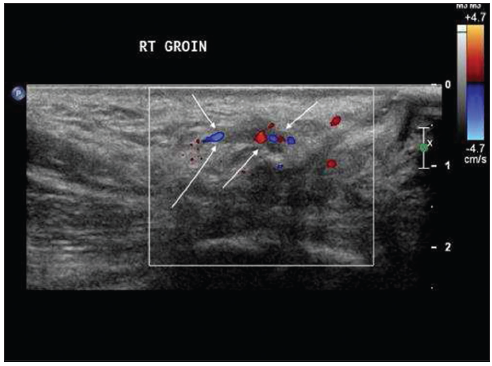
- Six weeks after initial presentation and treatment with enoxaparin, there was clinical resolution of the right groin mass in this 35-year-old postpartum woman. On this color Doppler ultrasound image, the round ligament veins are no longer dilated. The presence of flow signal (white arrows) within the veins suggests recanalization and resolution of varicosity.
With a clinical and radiological resolution of the thrombosed round ligament varicosities, low molecular weight heparin was stopped.
DISCUSSION
Anatomically, the round ligament anchors the uterus. It extends from the lateral aspect of the uterus bilaterally and courses through the deep inguinal ring and inguinal canal to the labia majora. The round ligament contains the veins, arteries, lymphatics, and nerves.
Round ligament varicosities (RLVs) are almost exclusively found in pregnant women. Three factors that contribute to varicose vein formation during pregnancy include (a) progesterone-mediated venous smooth muscle relaxation causing dilatation of the round ligament veins during pregnancy, (b) raised cardiac output causing increased venous return, and (c) engorgement of the venous system by the pressure from the gravid uterus.[2]
RLVs present most commonly during the second trimester of pregnancy. They present less commonly in the first trimester, third trimester, and post-partum period. One-third of the cases in the literature were reported to be bilateral.[3] Only 17% of cases present in the postpartum period, such as our index case.[3]
Inguinal swelling and pain during pregnancy are more commonly attributed to round ligament varicosities than hernias.[1] Inguinal hernias during pregnancy are reported to have an incidence of 0.03–0.1% (1 in 1000–3000). A case series by McKenna suggests the incidence of RLVs to be 0.13% (5/3816).[4]
A hernia of the inguinal region appearing for the 1st time during pregnancy is uncommon because most of the intra-abdominal structures that could potentially fill the hernia sac will be pushed aside by the growing uterus.[1]
Clinical examination alone cannot accurately distinguish inguinal hernias from round ligament varicosities.[5] They are both reducible and they both become larger with Valsalva maneuver. RLVs are often managed conservatively as most of them show spontaneous resolution postpartum. Inguinal hernias, however, need surgical treatment.
Radiologically, a RLV appears as a vascular structure, arises lateral to the inferior epigastric vessel, and courses through the inguinal canal as it tracks down to the labia majora. An indirect hernia follows a similar anatomical course as a RLV, also arising lateral to the inferior epigastric vessel. They are differentiated by (1) recognizing the peritoneal wall defect in hernias (2) recognising the hernia content which can be omentum, bowel or urinary bladder. A direct hernia, however, arises medial to the inferior epigastric vessel. The “bag of worms” in round ligament varicosities appear more prominent on standing up, and with cough impulse, similarly, a hernia protrudes on cough impulse or upright position. Patent round ligament varicosities are compressible while an uncomplicated inguinal hernia is reducible.
Round ligament varicosities and inguinal hernias are difficult to be differentiated clinically when uncomplicated. Furthermore, they present similarly when a RLV is thrombosed and when an inguinal hernia is strangulated.
Round ligament varicosities can be complicated by thrombosis or hemorrhage.[6] However, these complications are not common. In a case review series done by Ryu and Yoon, only one case of the 26 reported in the English literature was complicated by thrombosis.[3] The imaging appearance on USG and CT of thrombosed round ligament varicosities has not been widely reported. To the best of our knowledge, only one case report has been published in the English medical literature that showed CT/MRI findings of a thrombosed RLV. The lack of vascular flow signal on Doppler USG, the lack of compressibility on 2D ultrasound, and the CT pre-contrast hyperdensity and lack of enhancement on post-contrast CT as in our case illustrate the imaging appearance of thrombosed round ligament varicosities.
Ultrasound with Doppler is usually sufficient in differentiating uncomplicated round ligament varicosities from inguinal hernias, and it is the first modality of choice. However, ultrasound is operator dependent and may be suboptimal in obese patients. In cases where thrombosis is suspected, MRI or CT may be considered. On MRI, the RLV will appear as a dilated serpentine structure in the inguinal canal. In case of thrombosis, it will show high T1 signal and low T2 signal.[2] MRI will be the preferred modality if the patient is still pregnant. CT was chosen in our case as it was readily available and the patient is post-partum.
There are a few case reports of thrombosed round ligament varicosites in the English literature. There is no consensus as to how these complications should be managed. Some of these thrombosed cases were diagnosed on surgical exploration under the clinical impression of the groin mass being a strangulated inguinal hernia. Some cases were left alone without treatment and resolved spontaneously. In our case, the patient was given low molecular weight heparin for anticoagulation; eventually, the RLV and the thrombus were resolved.
CONCLUSION
Ultrasound and CT are useful in differentiating RLV and inguinal hernias, as well as recognizing their complications. Increased awareness among clinicians and radiologists of RLV and its prevalence in pregnant women can help prevent unnecessary surgical management due to mistakening RLVs as inguinal hernias. Furthermore, our case demonstrates that thrombosed round ligament varicosities can be managed successfully by anticoagulation.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given her consent for her images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Suspected inguinal hernias in pregnancy handle with care! Hernia. 2014;18:375-9.
- [CrossRef] [PubMed] [Google Scholar]
- Characteristic of computed tomography and magnetic resonance imaging finding of thrombosed varies of the round ligament of the uterus: A case report. J Comput Assist Tomogr. 2008;32:559-61.
- [CrossRef] [PubMed] [Google Scholar]
- Ultrasonographic diagnosis of round ligament varicosities mimicking inguinal hernia: Report of two cases with literature review. Ultrasonography. 2014;33:216-21.
- [CrossRef] [PubMed] [Google Scholar]
- Round ligament varices: Sonographic appearance in pregnancy. Ultrasound Obstet Gynecol. 2008;31:355-7.
- [CrossRef] [PubMed] [Google Scholar]
- Round ligament varicosities diagnosed as inguinal hernia during pregnancy: A case report and series from two regional hospitals in Japan. Int J Surg Case Rep. 2017;36:122-5.
- [CrossRef] [PubMed] [Google Scholar]
- Postpartum pain due to thrombosed varicose veins of the round ligament of the uterus. Postgrad Med J. 1993;69:820-1.
- [CrossRef] [PubMed] [Google Scholar]






