Translate this page into:
Complete Currarino Syndrome Recognized in Adulthood
Address for correspondence: Dr. Sinan Akay, Department of Radiology, Sirnak Military Hospital, Sirnak - 73100, Turkey. E-mail: akaysinan04@yahoo.com
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Currarino syndrome is a hereditary pathology that is characterized by sacrococcygeal bone defect, presacral mass, and anorectal malformation. Sacrococcygeal bone defect is almost always a part of the syndrome. The complete form of this entity displays all three abnormalities and is very uncommon. In this report, we present the magnetic resonance imaging findings of a case with complete form of Currarino syndrome recognized in adulthood.
Keywords
Anorectal
Currarino syndrome
meningocele
sacrococcygeal
INTRODUCTION

Currarino syndrome (CS) is a hereditary pathology that is characterized by a triad of malformations: Sacrococcygeal bone defect, presacral mass, and anorectal malformation. This pathology was first described by Currarino and his colleagues in 1981. The syndrome has complete and incomplete forms.[1] Radiologic imaging modalities such as ultrasonography (US), computed tomography (CT), and magnetic resonance imaging (MRI) play a vital part in diagnosis and follow-up of this pathology. In this report, we aim to present the magnetic resonance imaging (MRI) findings of a case with complete CS recognized in adulthood.
CASE REPORT
A 20-year-old male patient who underwent anal atresia operation in childhood was referred to our department for evaluation of anal sphincter status with transrectal US. Transrectal US could not be performed because of the severe anal canal stenosis. Therefore, MRI was performed for a detailed pelvic evaluation.
On MRI scan, calibration of one-third of the inferior rectum was observed to be very thin, while one-third of the superior and middle segments of the rectum was seen to be dilated. Bladder was displaced anteriorly because of the compression effect of dilated rectum. Partial cleft was detected at L5 vertebra corpus. S1 vertebra was partially deformed. The left half of S2 and S3 vertebrae, more distal sacral vertebrae, and coccyx were not seen. There was soft tissue heterogeneity around the anus secondary to earlier anal atresia operation. We also detected anterior meningocele related to spinal canal that originated from the neural foramen of S2 and S3 vertebrae. The lesion was isointense with cerebrospinal fluid in all of the sequences and its size was 4.5 × 3.5 cm. Anterior meningocele was slightly indented to adjacent rectum [Figure 1].
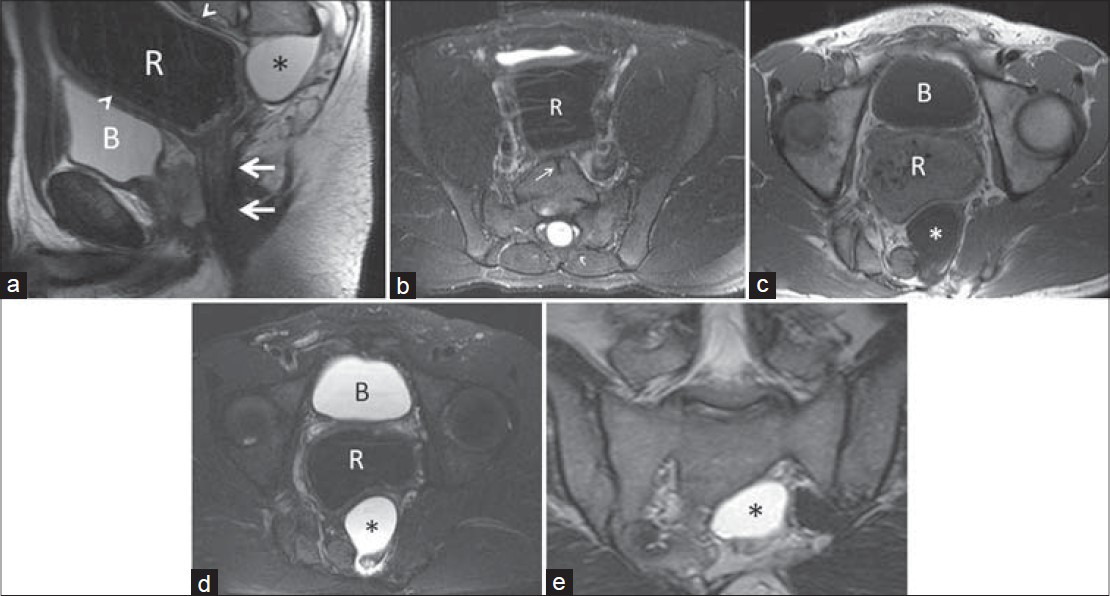
- 20-year-old man with anal atresia operation history in childhood diagnosed with Currarino syndrome. (a) T2-weighted sagittal magnetic resonance image shows calibre of one-third of inferior rectum is very thin (thick white arrows), while superior and middle segments of the rectum are dilated (arrowheads). Also, the images demonstrate anterior meningocele (asterisk) at the posterior of the rectum related to spinal canal that originated from the neural foramen of S2 and S3 vertebrae. The lesion is isointense with cerebrospinal fluid. (b) Fat-saturated T2-weighted axial magnetic resonance image shows partial cleft at L5 vertebra corpus (thin white arrow) and dilated rectum in front of it. On (c) T1-weighted and (d) Fat-saturated T2-weighted axial magnetic resonance images, left half of the sacrum is not seen. In this part, spinal canal relationship of anterior meningocele (asterisk) and its indentation to the adjacent rectum is also observed. (e) T2-weighted coronal magnetic resonance images demonstrate the contiguity of the sacral defect and anterior meningocele (asterisk) more clearly (R = rectum, B = bladder).
DISCUSSION
Currarino syndrome is a rare inherited disorder that is characterized by sacrococcygeal bone defect, presacral mass, and anorectal malformation.[1] The complete form of this syndrome shows all three abnormalities and is rarer than the incomplete form which includes one or two of the disease components mentioned above.[2] Sacrococcygeal bone defect is almost always a part of the syndrome.[3]
Although the patients with this syndrome may present with complex conditions like recurrent urinary system infections or meningitis, chronic constipation is the most common finding.[2] Some of the cases are asymptomatic and can be diagnosed during adulthood only on X-rays and US examinations that are performed for different reasons.[4] In addition to rectal digital examination, X-rays, US, CT, and MRI are very helpful in the diagnosis of the syndrome.[5]
Sacrococcygeal bone defect is a prerequisite for the diagnosis of CS and its spectrum changes from mild lateralization of the coccyx to multilevel hypoplasia of the sacral segments (“scimitar sacrum”).[6] In our case, there was partial cleft at L5 vertebra corpus and S1 vertebra was partially deformed. Also, the left half of S2 and S3 vertebrae, more distal sacral vertebrae, and coccyx were absent.
Rectal and/or anal stenosis which may be fistulized to ascending spinal canal is the most common anorectal malformation which is seen in CS.[6] Anal atresia or ectopy, imperforated anus, rectal duplication, and rectourethral, rectovaginal, and rectovesical fistulas may be also associated with the syndrome.[126] In our patient, calibration of the inferior rectal segment was very thin. Superior and middle segments of the rectum were dilated. There was heterogeneity of the cutaneous and subcutaneous soft tissue around the anus secondary to earlier anal atresia operation.
Presacral mass is yet another component of the syndrome. Anterior meningocele and benign teratomas are the most common presacral masses in CS. Enteric cyst, lipoma, hamartoma, dermoid and epidermoid cysts may be seen as well.[25] US, CT, and MRI are frequently used for diagnosing the mass lesion and determining its nature. MRI is an invaluable technique to recognize accompanying additional pathologies like tethered cord, syringomyelia, and intradural lipoma.[5] In our patient, we detected a 4.5 × 3.5 cm size anterior meningocele related to the spinal canal. It originated from the neural foramen of the S2 and S3 vertebrae.
Cloacal malformation with anal atresia, double vagina, rectovesical fistula, urogenital sinus, neurogenic bladder, vesicoureteral reflux, and multicystic kidney are other related pathologies of CS.[5]
MRI is a very useful imaging modality to diagnose CS and accurately detect all the three components. Besides, it can show the different aspects of other cloacal malformations including the uterus, vagina, maldeveloped puborectalis, and external anal sphincter. Although these anomalies are not surgically correctable, early detection almost always provides better prognosis and helps in patient management. Another major advantage of MRI over other imaging modalities is the ability to detect associated anomalies of anorectal malformations, especially of the spinal cord, spine, and urogenital system.[7] Kassir et al., also reported that MRI is a specific and sensitive non-invasive diagnostic tool in patients with anorectal malformations.[8]
MRI provides excellent information about the postoperative anatomy of anorectal malformations. Due to its superior soft tissue characterization, multiplanar imaging ability, and lack of ionizing radiation exposure, MRI has an advantage over CT.[9] These unique features make MRI a very appropriate modality in follow-up of patients treated for anorectal abnormalities.
The treatment strategy changes based on the type of pathology. The management of the anorectal anomaly and presacral mass may be performed with single-stage surgical procedure. If the mass is a meningocele, a staged operation must be preferred due to the risk of meningitis. The neurosurgical exploration should be performed before intestinal surgery.[10]
CONCLUSION
CS should be obviously considered in patients with sacrococcygeal bone defect, presacral mass, and anorectal malformation. Other associated pathologies should be investigated carefully as well. MRI may be used safely in diagnosis of the syndrome, in detecting the accompanying mass lesions and other pathologies, and in the follow-up investigations after treatment in patients with CS.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2015/5/1/10/152339
Source of Support: Nil
Conflict of Interest: None declared.
REFERENCES
- Triad of anorectal, sacral, and presacral anomalies. AJR Am J Roentgenol. 1981;137:395-8.
- [Google Scholar]
- The Currarino syndrome--hereditary transmitted syndrome of anorectal, sacral and presacral anomalies. Case report and review of the literature. Eur J Pediatr Surg. 1996;6:114-9.
- [Google Scholar]
- Currarino triad-diagnostic dilemma and a combined surgical approach. J Pediatr Surg. 2000;35:1790-4.
- [Google Scholar]
- MRI of anorectal malformations and relationship of the developmental state of the spincter muscle complex with fecal continence. World J Pediatr. 2006;3:223-30.
- [Google Scholar]
- A late-recognized Currarino syndrome in an adult revealed by an anal fistula. Int J Surg Case Rep. 2014;5:240-2.
- [Google Scholar]
- Results following treatment of anorectal malformations. In: Holschneider AM, Hutson JM, eds. Anorectal Malformations in Children (1st ed). Berlin, Heidelberg: Springer-Verlag; 2006. p. :361-77.
- [Google Scholar]
- Currarino triad associated with Hirschsprung's disease. J Pediatr Surg. 2003;38:1086-9.
- [Google Scholar]






