Translate this page into:
Can COVID-19 worsen racial disparities in breast cancer screening and diagnosis?

*Corresponding author: Haley Letter, Department of Radiology, Mayo Clinic, Jacksonville, Florida, United States. haley.letter@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Yacona K, Hanna MW, Niyazi S, Sharma S, Hatch P, Hernandez M, et al. Can COVID-19 worsen racial disparities in breast cancer screening and diagnosis?. J Clin Imaging Sci 2022;12:35.
Abstract
Background
Health disparities among minority groups, especially African Americans, can limit their access to quality medical care and lead to disproportionate medical management and disease outcomes. The aim of this study was to compare the COVID-19-related change in mammogram volumes and cancer detection at two affiliated academic breast centers, one that serves a predominantly African American patient population and one that serves a predominantly non-African American patient population.
Materials and methods
For the purpose of anonymity, racial demographics were collected and the center with a higher African American patient population was designated as institution A, while the center with a higher non-African American patient population was designated as institution B. Careful selection of the two breast centers was instituted in order to limit the impact of potential confounders other than race.
An Institutional Review Board (IRB) exemption was obtained and two Mammography Quality Standards Act (MQSA) reports were generated; one for March 2020 through September 2020, during the height of the COVID-19 pandemic, and one for March 2019 through September 2019 to serve as the pre-pandemic control group. The i2b2 Query Analysis Tool® was used to obtain racial demographic data and compare the percent change in screening and diagnostic mammograms, image-guided biopsies, total cancers diagnosed by imaging, and percent of minimal cancers for both institutions.
Results
Screening mammograms and breast cancer detection decreased in 2020 compared to 2019 at both institutions. However, the percent change from 2019 to 2020 was greater at institution A than at institution B. Percent minimal cancers, an indicator of early-stage breast cancer also decreased more drastically at institution A than at institution B. Interestingly, the total number of diagnostic exams and image-guided biopsies increased in 2020 at institution B, whereas both decreased at institution A.
Conclusion
The COVID-19 pandemic may lead to worsening racial disparities in breast cancer screening. In an effort to narrow future disparity, it is crucial for radiologists and other health care providers to be aware of this inequality and educate all women on the importance of obtaining routine screening mammography. More studies are needed.
Keywords
COVID-19
pandemic
mammography
screening
disparities
INTRODUCTION
Breast cancer is the most common non-cutaneous malignancy among women in the United States.[1] While the incidence of breast cancer is similar between Caucasian and African American women, the rate of dying from breast cancer differs among these racial groups, with African American women being 42% more likely to die of breast cancer in the United States.[2] African American women are also more likely to develop triple-negative breast cancer, be diagnosed with breast cancer at a younger age and present with a more advanced stage of breast cancer at diagnosis.[3]
Racial disparities are an ongoing societal issue, and various studies have aimed to identify potential causes for the disproportions seen in cancer screening and survival rates. There appears to be a spectrum of contributing variables, ranging from differences in molecular properties to issues with patient mistrust and access to adequate health care. One potential biological factor is the different subtypes of breast cancer that exist and have the potential to cause varied outcomes among individuals. These subtypes include but are not limited to, the estrogen receptor-positive, progesterone receptor-positive, human epidermal growth factor receptor 2 (HER2) positive subtype, the estrogen receptor-positive, progesterone receptor-negative, HER2 negative subtype, and the basal-like subtype, which is also known as triple-negative breast cancer and is the most aggressive.[4] African American women are at increased risk of developing the more aggressive triple-negative phenotype, and studies have identified differences in reproductive factors, tumor suppressor genes, chromosomal abnormalities, and primary tumor characteristics between African American women and Caucasian women.[4-8]
Aside from molecular nuances, inadequacies in trust and patient-physician communication may also play a role in the breast cancer burden among African American women. The history of discrimination, societal abuse, and medical experimentation endured by African Americans is said to have led to medical distrust, influencing the decision to pursue recommended mammography screening and physician follow-up.[9] Finally, socioeconomic imbalances in the distribution of healthcare resources and insurance selection in the United States is a hindrance throughout African American communities, with studies demonstrating that income and choice in the selection of physicians are significant predictors of consistency in health care visits.[9]
Racial disparities continue to impact the outcome of disease and illness in the United States, and the aim of this study was to assess how the COVID-19 pandemic has affected these known disparities. Changes in mammogram volumes and cancer detection during the first 6 months of the COVID-19 pandemic were assessed at two affiliated academic breast centers, one that serves a predominantly African American population and one that serves a predominantly non-African American population.
MATERIALS AND METHODS
Study design
The objective of this quantitative study was to compare the percent change in screening and diagnostic mammograms, image-guided biopsies, total cancers diagnosed by imaging, and percent of minimal cancers between two institutions. For the purpose of anonymity, racial demographics were collected and the center with a higher African American patient population was designated as institution A, while the center with a higher non-African American patient population was designated as institution B [Figure 1]. IRB exemption was granted for this study.
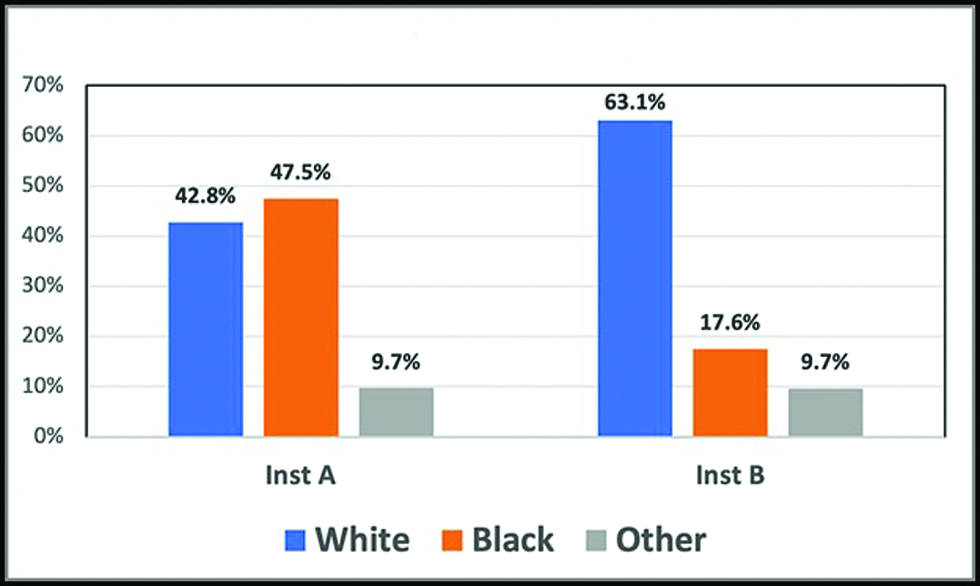
- Racial demographics: Percent population of patients who classify themselves as White, Black and Other at Institution A (Inst A) versus Institution B (Inst B).
Careful selection of the two breast centers was instituted in order to limit the impact of potential confounders other than race. For example, both centers are located in the same geographical region and were afflicted with similar COVID-19 infection rates and control measures. Both centers were also closed for screening exams for the same interval of time, approximately 8 weeks, between March 2020 and May 2020.
The i2b2 Query Analysis Tool® was used to analyze clinical and demographic data for the study. Institutions were analyzed and controlled based on location, facility closure duration, types of screenings provided, and patient race. Two Mammography Quality Standards Act (MQSA) reports were generated for both institutions, one report for March 2020 through September 2020, during the height of the COVID-19 pandemic, and the second report for March 2019 through September 2019 to serve as the pre-pandemic control group.
Analysis
Using the i2b2 Query Analysis Tool®, racial demographic data was obtained for both institutions. The study examined data from a total of 13,215 patients at institution A and 12,825 patients at institution B. At institution A, a total of 5,656 patients self-identified as Caucasian and 6,274 self-identified as African American. At institution B, a total of 8,095 patients self-identified as Caucasian and 2,252 self-identified as African American. The remaining 1,285 patients self-identified as Asian, Hispanic, or Other. The percent change in screening and diagnostic mammograms, image-guided biopsies, total cancers diagnosed by imaging, and percent minimal cancers for both institutions were collected on a population level using reports generated through MQSA.
RESULTS
At both institutions, screening mammograms and cancer detection decreased in 2020 when compared to 2019, with total and percent change in both categories being greater at institution A than at institution B [Figures 2 to 4]. When comparing the total number of screening versus diagnostic mammograms performed, the largest change was seen in screening mammograms performed at institution A, which had a decline of 20.9% [Figure 3]. When comparing the total number of diagnostic exams performed at each institution, it was found that institution A had a decrease of 17.9%, while institution B had an increase of 6.6% [Figure 3].
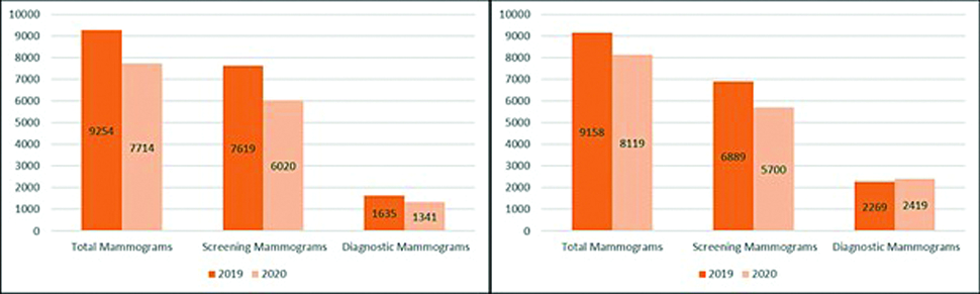
- Mammograms performed at Institution A and Institution B in 2019 and 2020. Amount of total, screening, and diagnostic mammograms performed at institution A (left graph) and institution B (right graph) in 2019 and 2020.
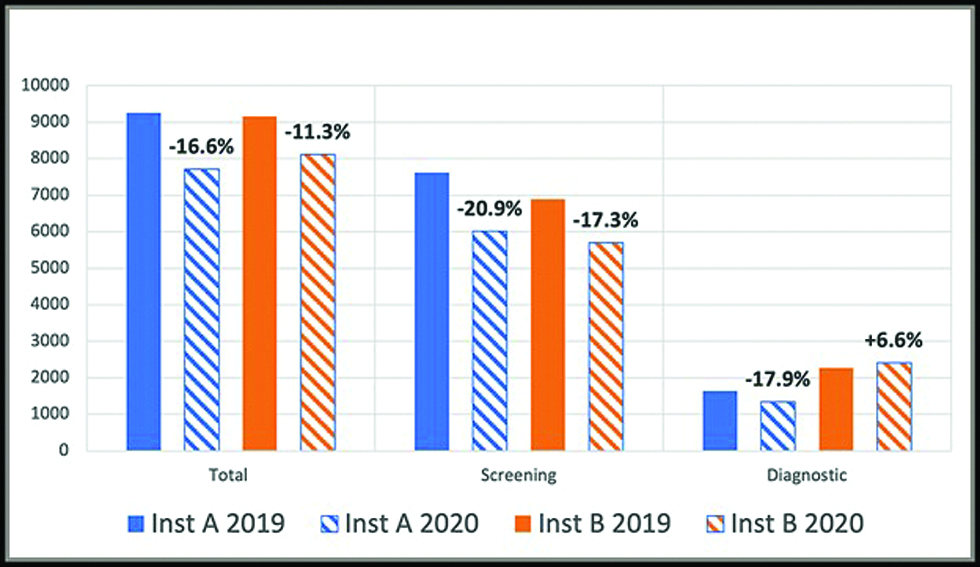
- Percent change in mammograms performed: 2019-2020. Total, screening, and diagnostic mammograms performed at Institution A (Inst A) and Institution B (Inst B) in 2019 and 2020. Percent increase or decrease from 2019 to 2020 at each respective institution is illustrated.

- Cancer detection: 2019-2020. Screen-detected cancers, total cancers detected, and percent minimal cancers from screening at Institution A (Inst A) and Institution B (Inst B) in 2019 and 2020. Percent decrease from 2019 to 2020 at each respective institution is illustrated.
Amount of total, screening, and diagnostic mammograms performed at institution A (left graph) and institution B (right graph) in 2019 and 2020.
The largest decline in total cancer detection was seen at institution A, which had 125 detections in 2019 and 72 detections in 2020, with an overall percentage decrease of 42.4% [Figure 4]. Institution B saw less of a decline in total cancer detection, with 123 detections in 2019 and 118 detections in 2020, a decrease of 4.1% [Figure 4]. Percent minimal cancer detection, an indicator of early-stage breast cancer, also decreased more drastically at institution A than at institution B, with a decline of 15.6% at institution A and 4% at institution B [Figure 4]. The most drastic change in screen-detected cancers was also seen at institution A, which had a total of 56 detections in 2019 and 22 detections in 2020, a percent decrease of 60.7% [Figure 4]. Institution B saw less of a decline, with 51 detections in 2019 and 34 detections in 2020, a percent decrease of 33.3% [Figure 4].
When comparing the total number of image-guided biopsies, there was a total of 349 biopsies performed at institution A in 2019 and 322 performed in 2020, a decrease of 7.7%. Interestingly, institution B had an increase of 3.1 %, with 447 biopsies performed in 2019 and 461 performed in 2020 [Figure 5].

- Image-guided biopsies: 2019-2020. Total image-guided biopsies were performed at Institution A (Inst A) and Institution B (Inst B) in 2019 and 2020. Percent increase or decrease from 2019 to 2020 at each respective institution is illustrated.
DISCUSSION
The COVID-19 pandemic continues to impact health and economies globally, and it has significantly disrupted access to cancer screening. When examining the relationship between COVID-19 and cancer screenings conducted in 2020, one cohort study determined that a total cancer screening deficit of 9.4 million remains throughout the United States.[10] A report published by IQVIA has also estimated that, overall, breast cancer screening in the United States saw a decrease of 87% by April of 2020 when compared to previous 5-year averages for that month.[11] In addition, when examining breast cancer screening rates in community centers that primarily provide health care to lower-income populations, one study found a decline of 8% between 2019 and 2020.[12] A separate study conducted at a safety-net hospital that provides screening to low-income individuals in San Francisco, California also found that during the first stay-at-home order between February 1, 2020, to May 31, 2020, the number of screening mammograms decreased by 41% in March and 100% in April.[13]
While various studies have examined the impact of COVID-19 and cancer screening, the goal of our study was to examine the potential disparate impact of the pandemic on breast cancer screening between racial groups. With many variables controlled for, including geography, technology, facility closure duration, and COVID-19 incidence in the community, the main variable in our study appears to be the racial demographics of the two patient populations. Therefore, our comparison is believed to highlight on a population level how the early effects of the COVID-19 pandemic resulted in lower breast cancer screening and cancer diagnosis when compared to the previous year, with these effects being more pronounced at the institution serving a predominantly African American patient population. Our assessment has shown that, when compared to the institution serving a predominantly Caucasian population, the institution serving a predominantly African American population experienced more of an impact from COVID-19 with regards to total mammograms performed, total biopsies performed, cancer detection rate, and percent minimal cancers. These findings appear to be consistent with a study recently conducted in Washington State, which also examined the impact of COVID-19 on breast cancer screening rates and found a greater reduction in screenings performed among African American women (−53.9%) than Caucasian women (−49.2%) from 2019 to 2020.[14]
There are various factors that potentially contributed to the decline in breast cancer screenings performed in 2020, including an increased demand at home due to school and daycare closures, an increase in unemployment and poverty rates, and reduced access to health insurance due to job loss. These factors seem to also be supported by findings in the Washington State study, as women who self-paid and who were insured by Medicaid appeared to experience the largest reduction in breast cancer screening during the pandemic.[14] Loss of employment also leads to loss of health insurance for many individuals, and since historically, African American women are already more frequently uninsured than Caucasian women, these factors may have had an even larger impact on African American women than on Caucasian women.[15] Studies are now also showing that the impact of COVID-19 on unemployment was different between men and women.[16] When comparing the impact of COVID-19 between men and women, the National Bureau of Economic Research found that social distancing and quarantine policies have had a larger effect on women’s unemployment than on men’s unemployment.[17] In addition, when comparing the implications of COVID-19 on family roles and work loss between men and women it was also found that losses in childcare support due to the pandemic have significantly impacted paid and unpaid labor of parents, with a more significant impact on mothers.[16] In many families, the mother takes on more childcare duties, offering a proposed reason for the disproportionate effect that the pandemic has had on women’s unemployment and their increased role in the household. Furthermore, when comparing recent unemployment data through the U.S Bureau of Labor and Statistics, it was found that the September 2020 unemployment rate of African American women was 10.8, while the unemployment rate of Caucasian women was 6.9.[18] This suggests that African American women have faced a larger rate of unemployment and potential subsequent loss of health insurance than Caucasian women have faced during the pandemic, and among the major racial groups examined in the 2020 census, African Americans also had the highest poverty rate (19.5%) in 2020.[19] Considering that the poverty rate has been independently associated with never having been screened for breast cancer, increases in poverty could potentially lead to even higher deficits in recognizing breast cancer among African American women.[20] In terms of school and daycare closures, there seems to also be a difference in effect among men and women. The National Bureau of Economic Research found that 21% of all children in the United States live only with their mother, compared to 4% who live only with their father, suggesting that school and daycare closures may have affected mothers disproportionately.[17] In addition, the Population Reference Bureau estimates that 64% of African American children in the United States live in a single-parent home, while 24% of Caucasian children live in a single-parent home, further suggesting that the burden of school and daycare closures may have more significantly impacted single African American mothers.[21]
Overall, the COVID-19 pandemic seems to have contributed to further increases in delayed breast cancer screenings and diagnosis that already exists among African American women. The principles behind these findings are multifaceted and highlight the importance of recognizing and counteracting disparities currently experienced among racial groups. As noted previously, studies have shown that African Americans are faced with the highest mortality rates for breast cancer, thus efforts to increase patient awareness of the risks of delaying breast cancer screening in this racial group is imperative. While our study highlights the effects of COVID-19 on breast cancer screening in a small population, there are several limitations that could be addressed in future studies. These limitations include small sample size, limited timeframe, and the restriction of using localized population data rather than wide-scale individualized data. Given the methods used, generalizability to other institutions and populations is also a limiting factor. While this study provides preliminary data on the possible effects of the COVID-19 pandemic on breast cancer diagnosis and outcomes, the use of more long-term data is needed to accurately assess this relationship and its implication on women’s health.
CONCLUSION
Prompt assessment of COVID-19-related trends in breast cancer screening is timely and imperative. It is crucial for radiologists and other health care providers to be aware of these findings and educate women on the importance of obtaining routine screening mammography. Our study has highlighted that, although breast cancer screening declined at both centers involved in the study, the decline in screenings and diagnosis seems to have disproportionately affected African American women. This highlights the fact that reducing clinical barriers to mammography screening, especially in African American women, must not be overlooked. While the COVID-19 pandemic has brought about new barriers to screening and access to health care, an effort is needed to adequately overcome these barriers and continue to provide cancer screening to patients. Improved education is also indicated, with a proactive effort to build trust and improve patient-physician communication. Research studies and screening protocols must also take into account racial disparities in breast cancer, and leaders and medical professionals from minority population groups must be represented in the decision-making process of these projects. Given the differences in biological factors and the varied breast cancer outcomes among racial groups, it is possible that more individualized screening guidelines and treatment options would provide greater success in closing the gap on racial disparities and decreasing breast cancer deaths in African American women.
Declaration of patient consent
Institutional Review Board (IRB) permission obtained for the study.
Financial support and sponsorship
Nil.
Conflict of interest
There are no conflicts of interest.
References
- Health and racial disparity in breast cancer. Adv Exp Med Biol. 2019;1152:31-49.
- [CrossRef] [PubMed] [Google Scholar]
- Breast cancer statistics, 2015: Convergence of incidence rates between black and white women. CA Cancer J Clin. 2015;66:31-42.
- [CrossRef] [PubMed] [Google Scholar]
- Racial disparity and triple-negative breast cancer in African-American women: A multifaceted affair between obesity, biology, and socioeconomic determinants. Cancers (Basel). 2018;10:514.
- [CrossRef] [PubMed] [Google Scholar]
- Ethnicity and breast cancer: Factors influencing differences in incidence and outcome. J Natl Cancer Inst. 2005;97:439-48.
- [CrossRef] [PubMed] [Google Scholar]
- Patterns and trends in age-specific black-white differences in breast cancer incidence and mortality-United States, 1999-2014. MMWR Morb Mortal Wkly Rep. 2016;65:1093-8.
- [CrossRef] [PubMed] [Google Scholar]
- Estrogen receptor/progesterone receptor-negative breast cancers of young African-American women have a higher frequency of methylation of multiple genes than those of Caucasian women. Clin Cancer Res. 2004;10:2052-7.
- [CrossRef] [PubMed] [Google Scholar]
- p53 as a marker of prognosis in African-American women with breast cancer. Ann Surg Oncol. 2010;17:1398-405.
- [CrossRef] [PubMed] [Google Scholar]
- Genome-wide copy number alterations in subtypes of invasive breast cancers in young white and African American women. Breast Cancer Res Treat. 2011;127:297-308.
- [CrossRef] [PubMed] [Google Scholar]
- Racial/ethnic disparities in breast and gynecologic cancer treatment and outcomes. Curr Opin Obstet Gynecol. 2007;19:31-36.
- [CrossRef] [PubMed] [Google Scholar]
- Association of cancer screening deficit in the United States with the COVID-19 pandemic. JAMA Oncol. 2021;7:878-84.
- [CrossRef] [PubMed] [Google Scholar]
- Accessed: September 10, 2021: https://www.iqvia.com/insights/the-iqvia-institute/covid-19/shifts-in-healthcare-demand-delivery-and-care-during-the-…
- Changes in breast cancer screening rates among 32 community health centers during the COVID-19 pandemic. Cancer. 2021;127:4512-5.
- [CrossRef] [PubMed] [Google Scholar]
- Trends in breast cancer screening in a safety-net hospital during the COVID-19 pandemic. JAMA Netw Open. 2021;4:e2119929.
- [CrossRef] [PubMed] [Google Scholar]
- Socioeconomic and racial inequities in breast cancer screening during the COVID-19 pandemic in Washington State. JAMA Netw Open. 2021;4:e2110946.
- [CrossRef] [PubMed] [Google Scholar]
- Closing the gap: Disparities in breast cancer mortality among African American women. Radiol Imaging Cancer. 2020;2:e200124.
- [CrossRef] [PubMed] [Google Scholar]
- The gendered pandemic: The implications of COVID-19 for work and family. Sociol Compass. 2021;15:e12881.
- [CrossRef] [PubMed] [Google Scholar]
- Accessed: November 02, 2021: https://www.bls.gov/news.release/empsit.t02.htm
- Accessed: November 02, 2021: https://www.census.gov/library/publications/2021/demo/p60-273.html
- Effect of area poverty rate on cancer screening across US communities. J Epidemiol Community Health. 2006;60:202-7.
- [CrossRef] [PubMed] [Google Scholar]
- Accessed: October 30, 2021: https://datacenter.kidscount.org/data/TABtables/107-children-in-single-parent-families-by-race#detailed/1/any/false/1729…






