Translate this page into:
Breast Hemangioma: MR Appearance with Histopathological Correlation
Address for correspondence: Dr. Rasha Ameen, 19 Grasmere Avenue, Kingston Vale, London, SW15 3RB, UK. E-mail: rashaameen@doctors.org.uk
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Breast hemangioma is a rare tumor and when small, it may be difficult to diagnose using conventional imaging techniques. In this report the MR appearance is described with histopathological correlation.
Keywords
Hemangioma
histopathology enhancement
mammogram
MRI
sonography
ultrasound
INTRODUCTION

Hemangiomas are benign vascular tumors rarely found in the breast. Ultrasound and mammography have been the mainstay for investigation of these breast lesions although diagnosis with these modalities may be difficult. This case report describes a case of a breast hemangioma with MRI findings.
CASE REPORT
A 33-year-old Caucasian female, presented to the breast clinic with a two week history of a palpable left breast lump. She denied any other symptoms and she had no relevant past medical history or family history of breast cancer. Physical examination revealed a small non-tender palpable nodule in the left superolateral quadrant lateral to the areola. The patient was initially referred for breast ultrasound which demonstrated a lesion. Mammography was not performed due to the age of the patient who was then referred for MR imaging for further detailed assessment.
The ultrasound showed a circumscribed hypoechoic nodule which was avascular on color Doppler ultrasound [Figure 1]. MRI demonstrated a small, circumscribed nodule just lateral to the left nipple of intermediate signal on T1-weighting [Figure 2] and intermediate to high signal on T2-weighting. There was avid early homogenous enhancement following contrast administration [Figure 3] with plateau formation seen on dynamic enhancement curve following initial early washout of contrast [Figure 4]. The nodule was of uncertain significance and was excised for histological assessment. This confirmed a diagnosis of capillary breast hemangioma [Figures 5, 6]. The nodule was completely excised.
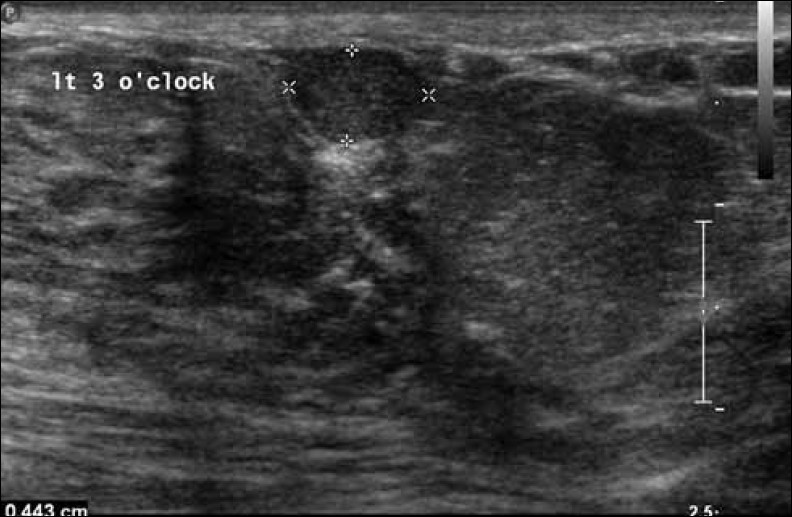
- Gray-scale ultrasound image shows a well-circumscribed nodule.
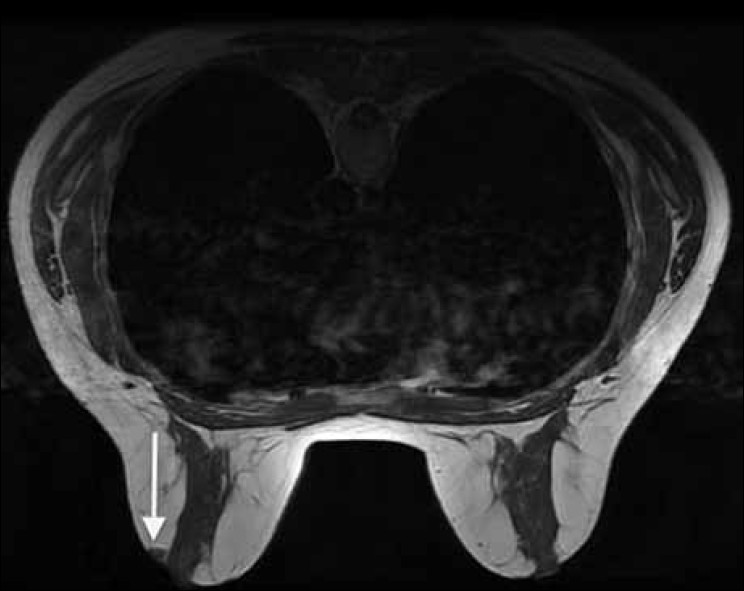
- Axial T1 –weighted MR image at the level of the nipple demonstrates a small, well circumscribed nodule lateral to left nipple of intermediate signal.
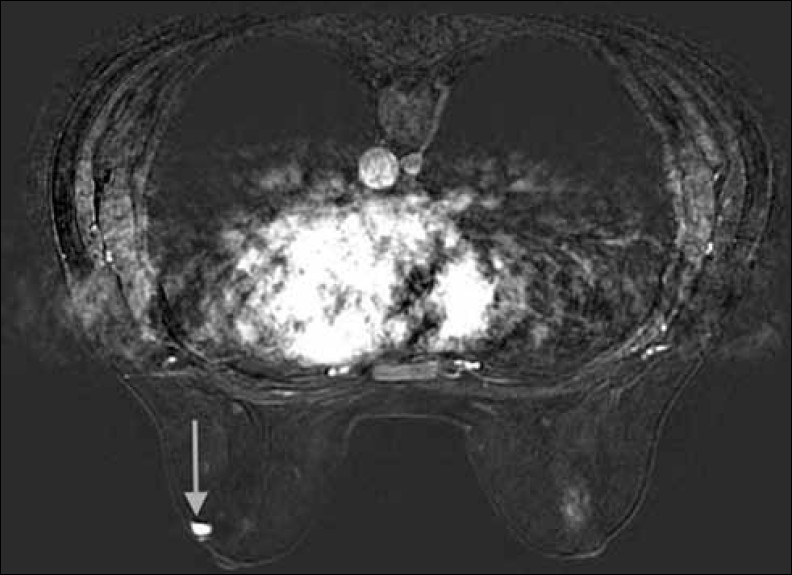
- Dynamic, fat saturated magnetic resonance performed immediately after intravenous contrast administration at the same level as Figure 2 demonstrates avid enhancement of the lesion lateral to the left nipple.
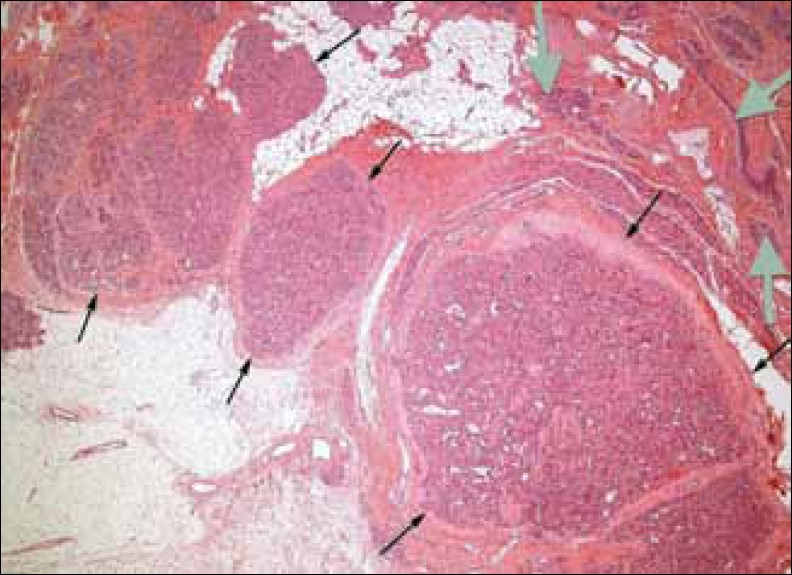
- Hematoxylin and Eosin stained tissue at ×40 low power view shows hemangioma (black arrows) and breast ducts and lobules (gray arrows).
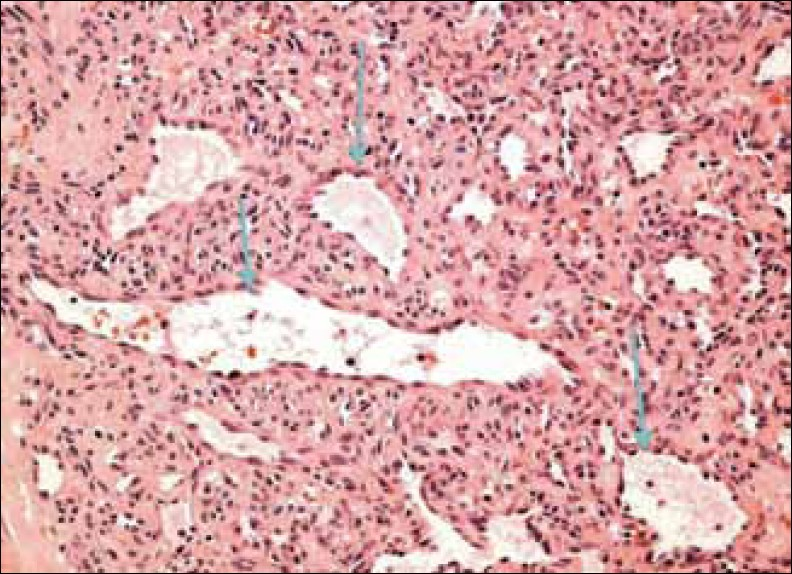
- Hematoxylin and Eosin stained tissue at ×400 high power view reveals abnormal vascular spaces in the hemangioma (arrows).
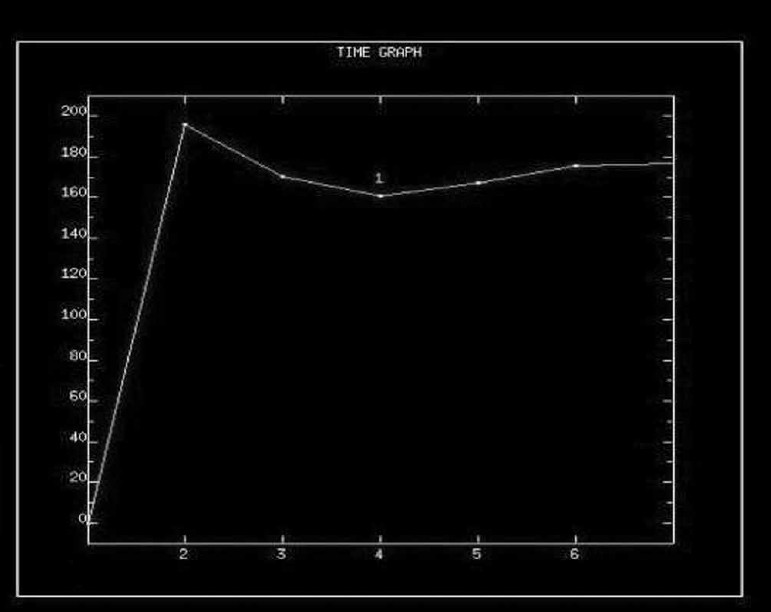
- This is a dynamic enhancement curve mapping lesion enhancement with time following contrast administration. It shows rapid initial enhancement, a peak, minor washout and then a plateau formation. This is an intermediate type of curve – malignant lesions have the rapid enhancement but also tend to washout rapidly as well – i.e. there is steeper curve drop as compared to what is seen in this image.
DISCUSSION
Hemangiomas are rare vascular tumors in the breast[12] with incidence between 1.2% and 11%.[34] Breast hemangiomas have a wide range of appearances and clinical behavior, with the potential to undergo malignant change.[3] They may be found incidentally following histological assessment of specimens taken during lumpectomy or mastectomy, often post mortem.[13] Hemangiomas are divided into two main types; capillary or cavernous; this is based on the size of the vessels involved,[3] the lesion in our case was a capillary hemangioma, not a cavernous one as the vessel size distinction was found with the help of the hispathological findings. Breast hemangiomas tend to be located superficially either in the subcutaneous tissue or subdermally and as such are palpable. However, conventional imaging modalities (sonography and mammography) may struggle to identify and characterise these lesions especially when they are small.[3] Studies have shown that the age variability of affected patients ranges from 18 months to 82 years.[1] Patients are often young making mammography of limited utility, due to the increased breast density. On mammogram, hemangiomas tend to appear as round opacities, which may contain internal calcification or phleboliths.[23]
The sonographic features of hemangiomas are variable and can be difficult to diagnose with confidence.[5] Small lesions located superficially can be isodense to the surrounding breast parenchyma making diagnosis difficult.[3] This is supported by examples where palpable and readily visible (to the eye) well-defined nodules were not detected sonographically.[1] Larger lesions appear more heterogeneous with serpiginous internal vessels present, and draining vessel may also be seen.
There is limited literature on the MR appearance of breast hemangioma, so far only 4 case reports have been described.[15–7] The available literature relates to large lesions with internal slow flow and draining vessels.[6] The hemangioma identified in our case report was small and highly vascular with avid enhancement. As shown previously in past clinical cases of breast lesions, it is often difficult to make a clear distinction between the two types of breast hemangiomas using MR images,[7] which is the reason why the breast hemangioma was excised in our case and confirmed to be capillary in nature using histopathological examinations. Although other MR morphological features suggested a benign nature, its avid early enhancement was a concerning factor which indicated the need for excision. Also the diagnostic dilemma posed by avid enhancement has been previously encountered and needs to be recognised.[56]
CONCLUSIONS
These rare tumors of the breast can pose radiological diagnostic challenges when using the conventional imaging techniques of ultrasound and mammography. The difficulty in confirming diagnoses of these lesions when small along with their avid enhancement can cause confusion with malignancy. Larger lesions may have more typical MR features associated with hemangioma, including slow flowing blood in internal vessel, areas of hemorrhage and thrombosis and venous lakes. The differentiation from angiosarcomas can be difficult.
ACKNOWLEDGMENT
The author would like to express gratitude and appreciation to K Ramesar., S M. Allan., and D. C. Howlett for their help in providing the relevant report and management of this patient.
Available FREE in open access from: http://www.clinicalimagingscience.org/text.asp?2012/2/1/53/100376
Source of Support: Nil
Conflict of Interest: None declared.
REFERENCES
- Sonographic and mammographic appearances of breast haemangiomas. AJR Am J Roentgenol. 2008;191:17-22.
- [Google Scholar]
- Incidence of perilobular hemangioma in the female breast. Arch Pathol Lab Med. 1983;6:308-10.
- [Google Scholar]
- Vascular tumours of the breast: Mammographic, sonographic and MRI appearances. AJR Am J Roentgenol. 2005;184:331-8.
- [Google Scholar]
- Gadolinium-enhanced dynamic MRI of breast haemangiomas. Comput Med Imaging Graph. 2003;27:493-5.
- [Google Scholar]






